Less expensive, post-acute care options for seniors underutilized

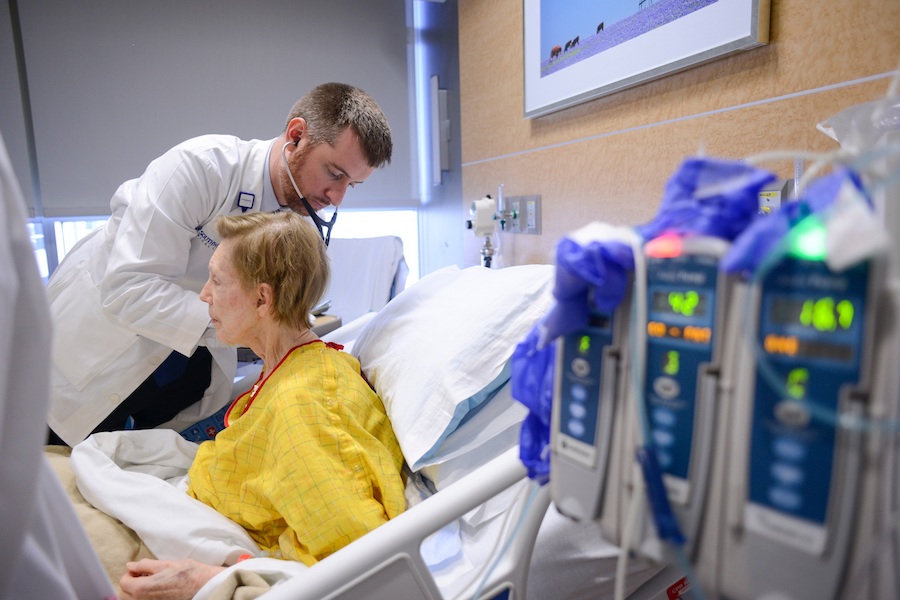
DALLAS – Feb. 22, 2018 – Long-term acute care (LTAC) facilities are designed to meet the needs of older adults with severe, complex illnesses who are recovering from hospitalization, but less expensive options sometimes overlooked may also be available, population health researchers at UT Southwestern found.
Only about half of older adults are transferred to LTACs for reasons related to the severity or complexity of their illnesses. For the other half, hospital preferences and regional trends often influence whether more cost-effective options are chosen, researchers in UT Southwestern’s Center for Patient-Centered Outcomes Research (PCOR) found.
“We found that many older adults are being sent to LTACs based on the preference of hospital providers and regional availability, when they may potentially be cared for as effectively in other, less expensive post-acute care settings, such as skilled nursing facilities,” said lead author Dr. Anil Makam, Assistant Professor of Internal Medicine at UT Southwestern Medical Center, which is recognizing its 75th anniversary this year.
Post-acute care is the single largest increase in and source of variation in Medicare spending nationally, and LTACs are the fastest growing and most expensive type of post-acute care. Researchers hope the findings in JAMA Internal Medicine highlight an opportunity to improve healthcare value by prompting doctors to consider transferring less ill patients to high-quality skilled nursing facilities that can still offer an appropriate and effective level of care.
The study, based on national Medicare data from 2010 to 2012, also showed that certain regions of the country have far higher rates of LTAC use, in part because of differences in long-term acute care availability.
“The extreme regional differences in long-term acute care use across the country suggest that there is overuse of LTACs in the South, including the Dallas-Fort Worth Metroplex, and possibly underuse of LTACs in the Pacific Northwest, the North, and the North Northeast. Nonetheless, geography is not entirely destiny, since hospitals located within the same region use LTACs very differently.”
Despite these findings, more research is needed to better understand when an LTAC versus a skilled nursing facility is the best option for individual patients.
“A key challenge is that no one knows what the right rate of LTAC use is, or even who the right person is to transfer to an LTAC,” said Dr. Makam. “There are some people who we know clearly benefit from long-term acute care services, such as those recovering from certain critical illnesses, but there are also a lot of grey areas that we’re not sure about. It is critical that we understand which individuals are most likely to benefit from LTACs for post-acute care so that we can make the smartest decisions about how to best use these resources to help older adults recover.”
UT Southwestern’s PCOR Center is funded through a grant from the Agency for Healthcare Research and Quality and helps facilitate studies designed to ensure delivery of high-quality, patient-centered, evidence-based, equitable care.
Other UT Southwestern researchers involved in the study include: Dr. Oanh Nguyen, Assistant Professor of Internal Medicine and Clinical Sciences, Lei Xuan and Mike Miller, data analysts in Department of Clinical Sciences, and Dr. Ethan A. Halm, Chief of the William T. and Gay F. Solomon Division of General Internal Medicine, Chief of the Division of Outcomes and Health Services Research in the Department of Clinical Sciences at UT Southwestern, and Director of UT Southwestern’s Center for Patient-Centered Outcomes Research. Dr. Halm holds the Walter Family Distinguished Chair in Internal Medicine in Honor of Albert D. Roberts, M.D. Dr. James S. Goodwin from the Sealy Center on Aging at the University of Texas Medical Branch also participated in the study, which was funded by a grant from the National Institute on Aging.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty has received six Nobel Prizes, and includes 22 members of the National Academy of Sciences, 17 members of the National Academy of Medicine, and 14 Howard Hughes Medical Institute Investigators. The faculty of more than 2,700 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in about 80 specialties to more than 100,000 hospitalized patients, 600,000 emergency room cases, and oversee approximately 2.2 million outpatient visits a year.