Saving Ryan: A story of hope, persistence, and medical ingenuity
Ryan Dant was afraid. He knew he likely wouldn’t live to see his 11th birthday due to a virulent disease that would stiffen his limbs, attack his heart, and destroy his brain.
Diagnosed with the rare, incurable disease mucopolysaccharidosis (MPS), Ryan and his family embarked on a desperate mission to save his life. Enrollment in a clinical trial in California initially brought hope, then disappointment. Ryan’s search for help led him back to UT Southwestern.
“Things happen for a reason. Things you don’t think are possible happen, and you’re shocked and upset. I’m going to continue to march in the direction I was going. Nothing is going to stop me from fulfilling my dreams,” Ryan wrote in a July 11, 2011, Facebook post.
“Are you OK? Text me,” responded UT Southwestern research nurse Sarah McNeil to Ryan, then age 24. Thus began a cascade of questions and answers that led to an experimental treatment at UT Southwestern and an amazing recovery, transforming Ryan’s life and saving much of his brain function.

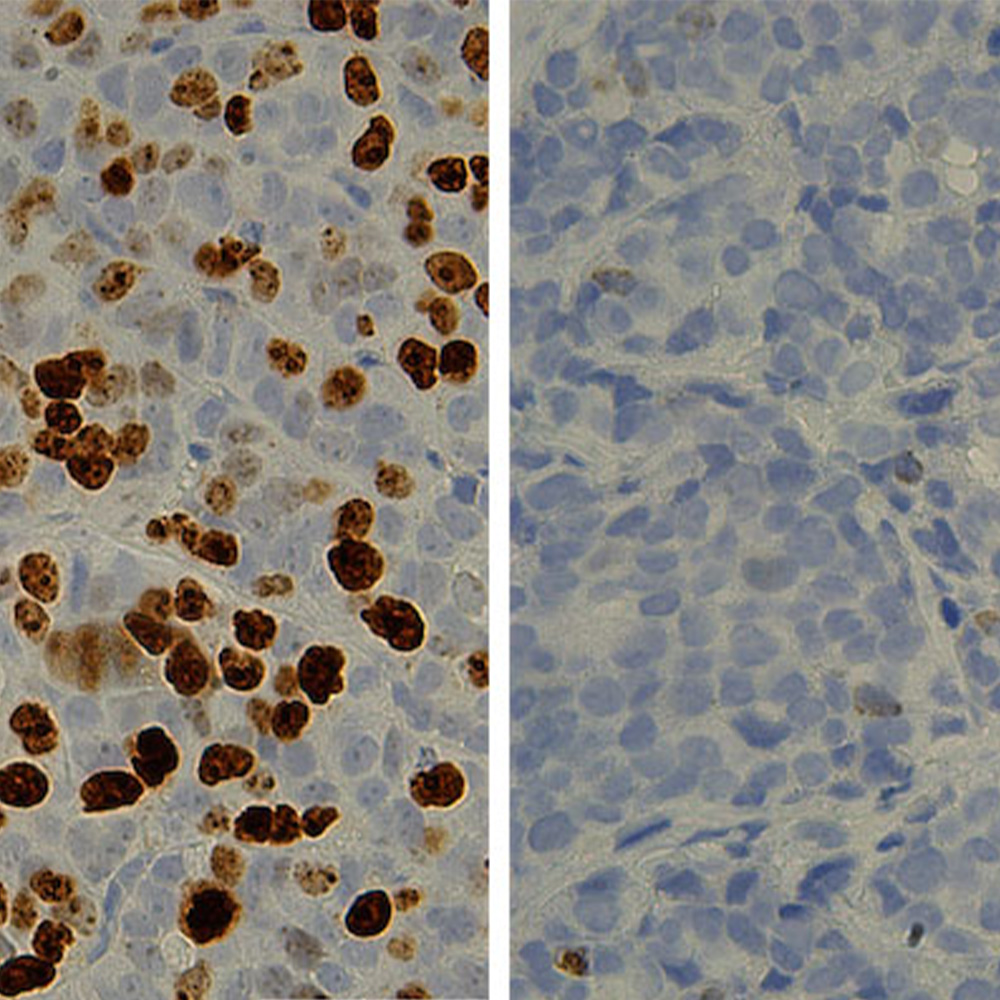
Ms. McNeil had known and treated Ryan for years. He first came to UT Southwestern as a 3-year-old and soon after was diagnosed with MPS 1, a subset of the disease in which a deadly enzyme deficiency blocks the body’s ability to break down proteins. Symptoms range from abnormal bone growth and lack of joint flexibility to respiratory problems and, eventually, brain damage. At the time, the average life span of MPS 1 patients was 10 years.
His father, a police officer, went to work raising money for MPS 1 research, resulting in donations of more than $1 million. In 1998, just before his 10th birthday, Ryan entered a UCLA clinical trial of a synthetic enzyme that his father’s fundraising helped bring beyond the lab.
The protocol allowed follow-up treatments with the synthetic enzyme at UT Southwestern, where Ms. McNeil was part of the team providing his care. Ryan’s fingers and limbs gradually uncurled and loosened, his breathing improved, and by age 12 he was back playing baseball.
However, midway through high school, his grades began to slide. He would study for hours, yet remember almost nothing the following day. Annual cognitive testing indicated his brain was in dangerous decline.
That situation, some years later, prompted the Facebook post and the nurse’s question.
After he texted details to Ms. McNeil, she contacted Dr. Elizabeth Maher, Director of UT Southwestern’s translational research program in neuro-oncology, part of the Annette G. Strauss Center for Neuro-Oncology. Dr. Maher, also Professor of Internal Medicine and Neurology and Neurotherapeutics with UT Southwestern’s Peter O’Donnell Jr. Brain Institute, holds the Theodore H. Strauss Professorship in Neuro-Oncology.
The major question they faced was, “What more can we do?”
Dr. Maher initiated the process to ask for a compassionate-use clinical trial. It would be based on the earlier protocol, but the synthetic enzyme would be injected directly into the spinal fluid in hopes it would reach the brain and start to break down the proteins that were disrupting Ryan’s brain function. Because Ryan’s spinal cord was severely narrowed by clogged proteins, the medical team hoped that repeated injections would unclog the canal and provide a clear path to the brain.
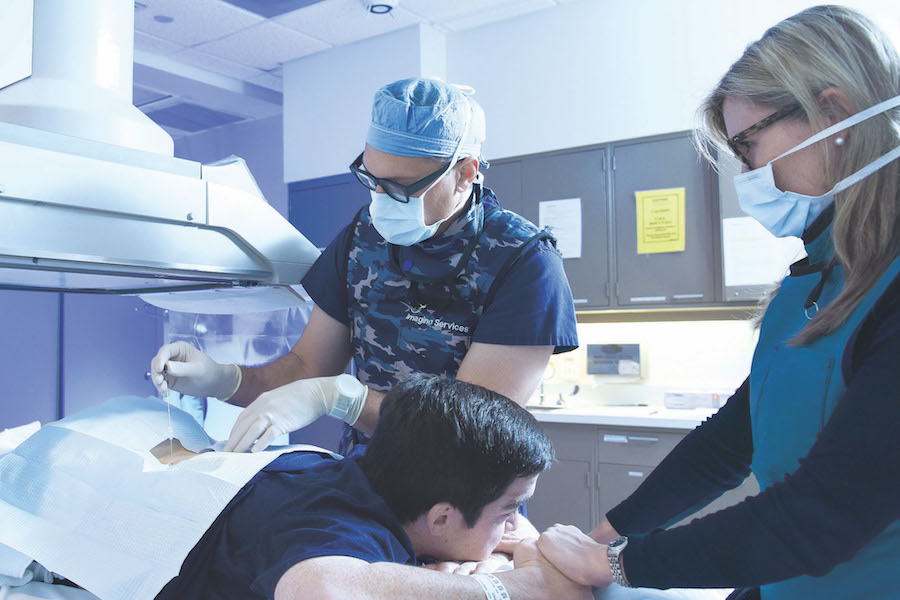
Ryan’s first spinal injection was performed in 2012 by Dr. Edward Stehel, Assistant Professor of Radiology.
The effects were dramatic: Ryan was again able to process complex information, he started remembering what he studied as a Dallas-area junior college student, he began earning A’s and B’s, and he improved enough to transfer to his dream school, the University of Louisville.
“We had only hoped to stop the neurocognitive decline, but as the enzyme worked to break down the proteins, Ryan got better. This stunning result is giving us a road map to how we can think about other diseases in the brain. Ryan’s journey will impact the lives of countless other children,” said Dr. Maher, who authored a study published last year that documents his cognitive recovery.
Ryan has lived long beyond the life expectancy of MPS 1 patients. He is one of only four survivors of the 10 initial clinical trial participants. Ryan has a girlfriend. He is a college graduate. And he’s looking forward to pursuing a career in sports administration, perhaps one day working in operations for a Major League Baseball team.
“It’s an incredible story that shows us there is so much recovery that can go on in the brain. Ryan will be forever my grounding to the idea that sometimes you must get out on the leading edge and push the boundaries,” Dr. Maher said.
Mark Dant, who still tears up when talking about his son’s battle to survive, watched Ryan walk across the stage to receive a college degree last year.
“Sarah [McNeil] could have said they don’t do experimental MPS treatments here. Dr. Maher could have said that it’s a really great story; they should go find someone to do that treatment,” he said. “But they gave it a shot, and look at where we’re at today. It was worth the try.”