Hospital-acquired anemia more common, increases risks

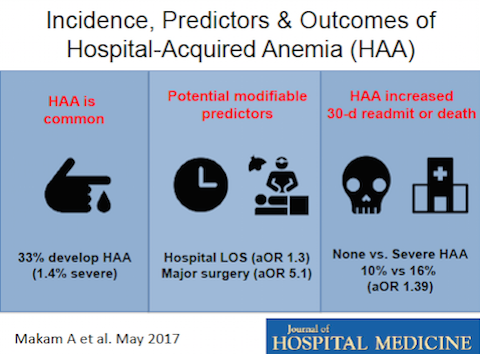
DALLAS – May 17, 2017 – One in three patients hospitalized for medical problems experienced a drop in their red blood cell count due to the hospitalization – a concept called hospital-acquired anemia, new research showed.
Moreover, the worse the hospital-acquired anemia – or the more blood lost – the higher the risk of death or readmission, even after adjusting for other important factors, UT Southwestern Medical Center researchers reported in a study involving 11,000 patients cared for in six hospitals.
“This study shines a spotlight on a very common but underappreciated risk of hospitalization, hospital-acquired anemia, which has traditionally been viewed as an incidental change in the red blood count of no significance. However, our results showed that hospital-acquired anemia was associated with worse clinical outcomes after leaving the hospital so it needs to be taken more seriously,” said senior author Dr. Ethan Halm, Director of UT Southwestern’s Center for Patient-Centered Outcomes Research and Chief of the William T. and Gay F. Solomon Division of General Internal Medicine at UT Southwestern. Dr. Halm, Professor of Internal Medicine and Clinical Sciences, holds the Walter Family Distinguished Chair in Internal Medicine in Honor of Albert D. Roberts, M.D.
Hospital-acquired anemia is defined as having a normal blood count on admission but developing anemia during the course of hospitalization. The most severe form of hospital-acquired anemia was independently associated with a 39 percent increase in the odds of being readmitted or dying within 30 days after hospital discharge compared with not developing hospital-acquired anemia. The most severe form was defined as a hematocrit of 27 percent or less at the time of discharge, occurring in 1.4 percent of all hospitalizations in the study, which appears in the Journal of Hospital Medicine.
“This is the first study of post-discharge adverse outcomes of hospital-acquired anemia among a diverse group of patients who were hospitalized for different reasons,” said lead author Dr. Anil Makam, Assistant Professor of Internal Medicine and Clinical Sciences and a member of the Center for Patient-Centered Outcomes Research. Other studies have examined post-discharge outcomes in patients hospitalized for heart attacks.
While the study does not establish preventability, it points to several directly associated risk factors of developing hospital-acquired anemia. “Our findings suggest that reducing blood loss during major surgeries and reducing unnecessary testing during hospital stays may lower a patient’s risk of developing severe hospital-acquired anemia, and potentially improve their recovery,” said Dr. Makam.
In the current study, researchers found that the two strongest potentially modifiable predictors of developing moderate or severe hospital-acquired anemia are length of hospital stay and patients undergoing major surgery. In the future, researchers hope to examine other patient-centered outcomes that may be related to hospital-acquired anemia, such as fatigue, functional impairment, and the trajectory of post-hospital recovery.
Others involved in the study included Dr. Oanh Nguyen, Assistant Professor of Internal Medicine and Clinical Sciences, and analyst Christopher Clark in the Office of Research Administration at Parkland Health and Hospital System.
The study was supported by UT Southwestern’s Center for Patient-Centered Outcomes Research (PCOR) and the National Institute on Aging. PCOR helps facilitate studies designed to ensure delivery of high-quality, patient-centered, evidence-based, equitable care. The UT Southwestern PCOR Center is funded through a grant from the Agency for Healthcare Research and Quality (AHRQ), with a mission to produce evidence to make health care safer, higher quality, more accessible, equitable, and affordable, and to work with the U.S. Department of Health and Human Services and other partners to ensure that the evidence is understood and used.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty includes many distinguished members, including six who have been awarded Nobel Prizes since 1985. The faculty of almost 2,800 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide medical care in about 80 specialties to more than 100,000 hospitalized patients and oversee approximately 2.2 million outpatient visits a year.
###
Media Contact: Remekca Owens
214-648-3404
remekca.owens@utsouthwestern.edu
To automatically receive news releases from UT Southwestern via email, subscribe at www.utsouthwestern.edu/receivenews