Study shows Zika virus directly infects brain cells and evades immune system detection

DALLAS – June 3, 2016 –The mosquito-borne Zika virus linked to microcephaly and other neurological problems in newborns of affected mothers directly infects the brain progenitor cells destined to become neurons, UT Southwestern Medical Center researchers report in a study published online today in Cell Reports.
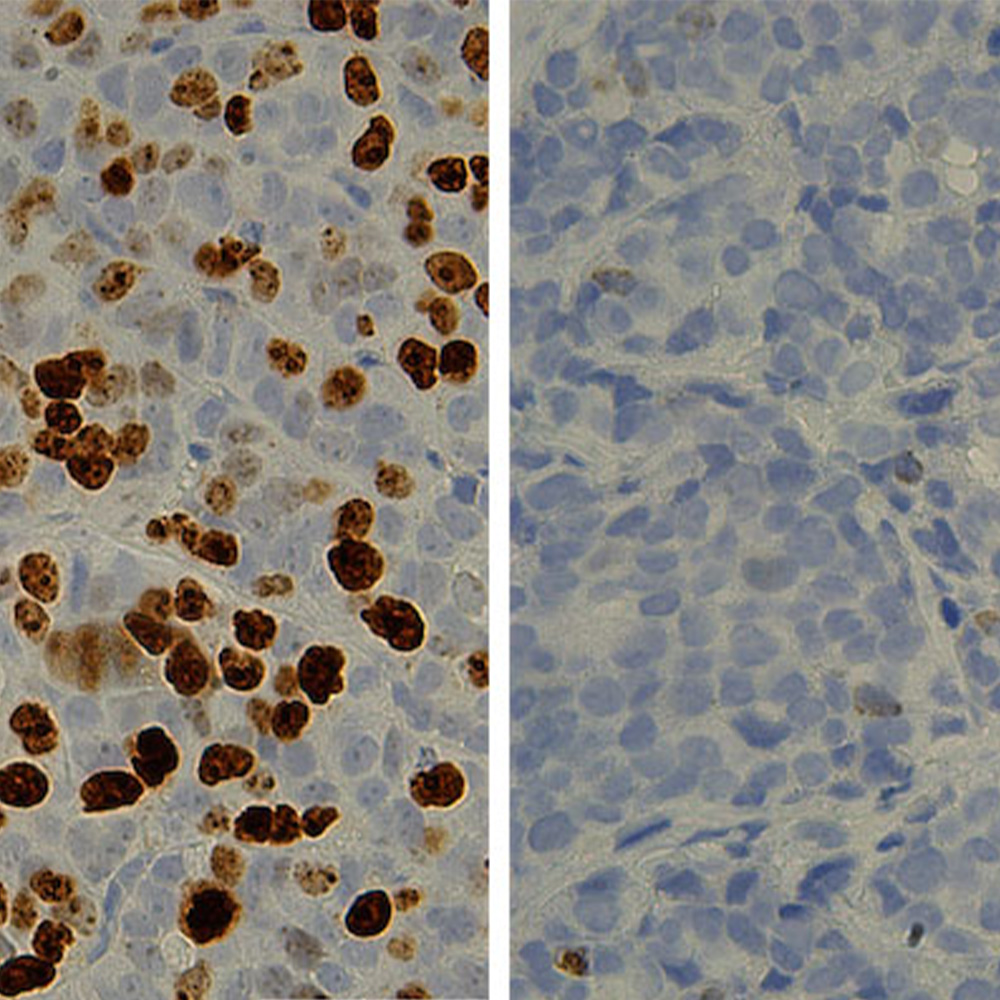
The team of researchers used a strain of Zika currently impacting the Americas, and found that the virus infects about 20 percent of cells on average, evades immune system detection, and continues to replicate for weeks.
“The cellular system we studied mirrors what pathologists are finding in the brain tissue of affected infants and will be valuable for further understanding how Zika causes severe brain-related problems. The system may also serve as a platform for testing new therapies targeting the virus,” said Dr. John Schoggins, Assistant Professor of Microbiology at UT Southwestern and senior author of the study.
Zika can be spread by infected mosquitos or through sexual intercourse. In adults, the symptoms are generally mild and include fever, rash, joint pain, and red eyes. However, Zika virus can cause a serious birth defect called microcephaly, and other severe neurological effects such as eye problems, hearing loss, and impaired growth in infants born to women who contracted the virus when pregnant, according to the Centers for Disease Control and Prevention (CDC).
The CDC’s website lists a series of unanswered questions about the virus that the World Health Organization (WHO) has declared a public health emergency of international concern. The unanswered questions include when during pregnancy the infection may harm the fetus and how the virus affects individual pregnancies.
“There was a suggestion that the detrimental effects of the virus might be linked to its ability to infect brain cells, specifically the progenitor cells that give rise to neurons,” said Dr. Schoggins, a Nancy Cain and Jeffrey A. Marcus Scholar in Medical Research, in Honor of Dr. Bill S. Vowell.
“We showed that neural progenitors can be infected by a strain of Zika virus that is currently infecting people in the Americas,” Dr. Schoggins said. “We found that the virus kills some neural progenitor cells, but not all. Other cells survive the infection, and surprisingly, continue to replicate the virus for many weeks. In addition, it appears that Zika virus does not stimulate much of an immune response.”
Dr. Schoggins collaborated on the study with Dr. Genevieve Konopka, Assistant Professor of Neuroscience and a Jon Heighten Scholar in Autism Research, whose expertise includes working with neural progenitor cells, cells similar to stem cells that tend to differentiate into neurons. Other UT Southwestern co-authors included: lead author Dr. Natasha Hanners, a pediatric infectious diseases fellow training in Dr. Schoggins’ lab; Jennifer Eitson, a research assistant in Microbiology; Dr. Noriyoshi Usui, a postdoctoral researcher in Neuroscience; and Microbiology graduate student R. Blake Richardson. A researcher from UCLA also participated.
This project received support from the National Institutes of Health and the Rita Allen Foundation.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty includes many distinguished members, including six who have been awarded Nobel Prizes since 1985. The faculty of almost 2,800 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide medical care in about 80 specialties to more than 100,000 hospitalized patients and oversee approximately 2.2 million outpatient visits a year.
###
Media Contact: Deborah Wormser
214-648-3404
deborah.wormser@utsouthwestern.edu
To automatically receive news releases from UT Southwestern via email, subscribe at www.utsouthwestern.edu/receivenews