UTSW physicians first in Texas to transplant lungs using new technology to make more organs viable
DALLAS – June 1, 2016 – Transplant surgeons at UT Southwestern Medical Center have performed the first lung transplant in Texas using donated lungs treated with new technology known as ex-vivo lung perfusion.
Ex-vivo lung perfusion (EVLP) allows physicians to evaluate and recondition lungs, making lungs that would have been unsuitable for transplantation potentially viable. UT Southwestern is one of 16 medical centers across the country – and the only one in Texas – participating in a national clinical trial of the technology, which, if effective, could significantly expand the number of donor lungs available for transplantation.
“Currently, more than 70 percent of potential donor lungs are deemed unusable,” said Dr. Fernando Torres, Professor of Internal Medicine and Medical Director of the Lung Transplantation Program at UT Southwestern. “EVLP technology is an assessment tool that will allow us to evaluate organs that are marginal over an extended period of time. We can see how well these lungs inflate and deflate, see how well gas exchange is happening, and some of these lungs will be found to be suitable for transplant.”
In 2015, 2,075 lung transplants were performed in the U.S., but more than 200 people died while awaiting a lung transplant, including 22 Texans, according to data from the United Network for Organ Sharing (UNOS), the non-profit organization that manages the nation’s organ transplant system. UT Southwestern, one of the leading medical centers in the country in lung transplants, has performed more than 60 lung transplants each year for the last three years, and more than 500 lung transplants overall, ranking the medical center No. 8 among all the centers in the country that are currently performing lung transplants, according to UNOS.
“Some of the lungs we see are clearly not usable because of infections, bad contusions, and so on, but with others, it’s simply not clear,” said Dr. Pietro Bajona, Assistant Professor of Cardiovascular and Thoracic Surgery and Director of the EVLP Program. “We can put the questionable lungs in the machine, ventilate them, perfuse them with a special solution, and then after a few hours test them.
“There are many people who are waiting for a transplant who are very sick, and even though the number of donors is increasing, there are still not enough lungs available to meet demand,” Dr. Bajona said.
EVLP is expected to increase the number of lungs available for transplant by 10 to 15 percent.
John Herzig became the first patient in Texas to be transplanted with lungs that were evaluated with EVLP technology. The 58-year-old former Oklahoma school superintendent was forced to retire early because of deteriorating health due to pulmonary fibrosis, a scarring of the lungs that leads to severe breathing problems. He was so weak before the transplant, he couldn’t play with his grandson.
“Before the transplant, I could ride on the tractor with my grandson, but I couldn’t do anything else with him. I was just too weak,” said Mr. Herzig, who led a robust life before being sidelined. “So when they called it was not a hard choice. I trusted my care to these doctors and I didn’t want to turn down an opportunity.”
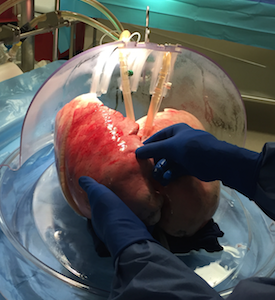
Mr. Herzig had been on the waiting list for a week, when a potentially viable set of lungs was donated. In April, Mr. Herzig waited in a hospital room as Dr. Bajona removed the lungs from the donor to test them in the dome-shaped technology. The XVIVO device, created by a Swedish company, has already been approved for use in Europe and Canada, and the current study will help determine whether it is approved for general use in the United States.
After examining the inside of the lungs with a bronchoscope, the EVLP team began running a fluid that provides nutrients and removes waste products through the blood vessels of the lungs. Pulmonologist Dr. Amit Banga, Assistant Professor of Internal Medicine, along with the rest of the EVLP team assessed the lungs, paying particular attention to three measures: the transfer of oxygen; pressure in the blood vessels; and compliance, which is a measure of the ability of the lung tissue to stretch and expand.
“The basic job of the lungs is to get oxygen into the blood and that’s something that we can assess and maybe even improve with this technology,” Dr. Banga said. “If the pressure in the blood vessels of the lungs is too high, that’s a sign of worsening, so we pay close attention to that. And we like the lungs to be like a nice balloon that expands appropriately and then goes back to its regular size.”
The EVLP not only allows for careful assessment of the lungs but even improves the condition of the lungs by providing an opportunity for excess fluid that has accumulated in the lungs to dissipate.
“EVLP means we can save people like Mr. Herzig, which is very rewarding,” said Dr. Bajona.
After about three hours, the team of physicians determined the lungs were usable and Dr. Matthias Peltz, Surgical Director of Cardiac Transplantation and Mechanical Circulatory Support, led the surgical team that performed the transplant.

“There are more lungs declined in the operating room than any other organ,” said Dr. Peltz, Associate Professor of Cardiovascular and Thoracic Surgery. “Ex-vivo perfusion technology allows us to evaluate organs for transplantation that we either would not previously have considered for transplantation or would have declined in the operating room. If the ex-vivo evaluation is favorable, we can then implant the perfused lungs, significantly increasing the number of available organs for our patients.”
“This new technology, which improves the physical status of lungs while outside the human body, is a great example of how technology is expanding our existing donor pool so that we may save more lives,” said Patti Niles, CEO of Southwest Transplant Alliance, the federally designated organ procurement organization serving much of Texas.
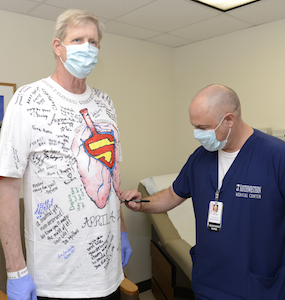
Though it will be some months before he can return to his Oklahoma farm, Mr. Herzig is especially looking forward to playing a bigger role in the life of his 4-year-old grandson, Harrison. While recovering in the ICU, Mr. Herzig’s daughter, Abbie, decorated a T-shirt with a drawing of his new “super lungs,” which many of the physicians and nurses signed. He plans to wear it for his first game of catch with Harrison.
“I’m so grateful to the family who agreed to donate these lungs,” said Mr. Herzig, “and thankful for the new technology that helped make them available, so now I’ll have that opportunity to play with my grandson and watch him grow.”
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty includes many distinguished members, including six who have been awarded Nobel Prizes since 1985. The faculty of almost 2,800 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide medical care in about 80 specialties to more than 100,000 hospitalized patients and oversee approximately 2.2 million outpatient visits a year.
###
Media Contact: Cathy Frisinger
214-648-3404
cathy.frisinger@utsouthwestern.edu
To automatically receive news releases from UT Southwestern via email, subscribe at www.utsouthwestern.edu/receivenews