Residency Program
UTSW Urology Residency Mission
The mission of the UT Southwestern Urology residency program is to match the highest caliber of physician-graduates from diverse backgrounds and experiences, and provide them an educational experience to ultimately develop into highly skilled, knowledgeable, compassionate, and resilient urologists, fully prepared to lead and excel in the areas of patient care, service, education, and research across all corners of the United States and beyond.
The program balances graduated clinical responsibilities with faculty supervision, organized conferences, and mentored research. Our program offers a robust surgical experience covering all areas of urological surgery, with internationally recognized leaders in each urology subspecialty. Additionally, we offer fellowships in
- URPS (ACGME)
- MIS/Robotics/Laparoscopy (WCE)
- Pediatric Urology (ACGME)
- Trauma, Reconstruction, and Prosthetics (GURS)
- Urologic Oncology (SUO)
Overall, approximately 50 percent of our graduates go on to additional fellowship training with the remainder entering the urology workforce as comprehensively trained general urologists.
Residents are provided abundant opportunity to develop their clinical and surgical skills within a supervised environment, while developing the confidence to practice independently.
Rotation Sites
Residents spend clinical rotations in a variety of hospital settings. This allows for a diverse clinical experience, with the opportunity to provide care for patients afflicted by the most complex urological conditions, presenting from all corners of society both locally and throughout the North Texas region and beyond. The Department feels strongly that having exposure to busy tertiary hospital settings (William P. Clements Jr. University Hospital and Children's Medical Center Dallas), large county hospitals (Parkland Health and Hospital System and John Peter Smith Health Network), and a Veteran's Hospital that draws from the entirety of North Texas will allow trainees the experiences they need to flourish once completing their training. Each affiliated hospital has one or more robotic surgical systems including a dual console Si robot at Children's Medical Center, three dual console Xi systems at the Veterans Affairs Medical Center, two dual console Xi systems at Parkland, two dual console (one Xi, one Si) systems at John Peter Smith, and 2 dual console Si systems, 3 dual console Xi systems, and 1 SP system at Clements University Hospital.
- Clements University Hospital
- Parkland Memorial Hospital
- Children's Medical Center Dallas
- VA Medical Center of North Texas
- John Peter Smith Hospital, Fort Worth
Resident Training Sequence
PGY-1 Year
Training begins with an internship at UT Southwestern. Six months of the year are spent in Urology, with three months in general surgery, and an additional three months in ICU, trauma, and/or other surgical subspecialties. Basic surgical skills training is also provided at the newly constructed Simulation Center at UT Southwestern.
PGY-2 Year
During the PGY-2 year, substantial time is devoted to diagnostic urologic skills, including endoscopy, ultrasound, and urodynamics. Rotations at Children's Medical Center (CMC), Parkland Memorial Hospital (PMH), the Dallas Veteran Affairs Medical Center (VAMC), and UT Southwestern's William P. Clements Jr. University Hospital (CUH) provide the PGY-2 resident with substantial experience in the clinic and operating room.
PGY-3 Year
The PGY-3 year offers a diverse introduction and expansion of open, robotic, and endourological surgical techniques. In addition to rotations at VAMC and CMC, residents rotate at John Peter Smith Hospital (JPS) in Fort Worth where they are introduced to robotics, major oncology, and male lower and upper tract reconstructive surgery while also enhancing their percutaneous and transurethral endoscopy skills. Additionally, two 10-week outpatient blocks are used to hone outpatient urology skills and to explore specific interest areas within urology. Residents are expected to participate in research during these blocks, with close faculty mentorship in an area of their choosing, and ultimately submit one or multiple research projects for regional or national presentation and publication.
PGY-4 Year
During the PGY-4 year, trainees function at the Chief Resident level at CMC, performing a variety of complex pediatric urology procedures. Residents also act as senior residents at PMH and CUH where they serve as primary surgeon for a myriad of complex open reconstructive and oncology cases. An outpatient adult rotation brings mentored exposure to tertiary care clinics with faculty in each of the urology subspecialties at our main outpatient campus, while allowing flexibility for further operative, outpatient, and research exposure in any area of interest to the PGY-4.
PGY-5 Year
Chief residents direct each of the urology inpatient services at PMH, VAMC, JPS and CUH. Each of these rotations serve as part of the "capstone" year where PGY-5s develop increasing mastery of robotic surgery, complex oncology, and advanced lower and upper tract reconstructive surgery in men and women. At each of these high-volume centers, chiefs have the option to tailor their surgical experience to their needs or interests, depending on their future career plans.
Sample Resident Rotation Schedule
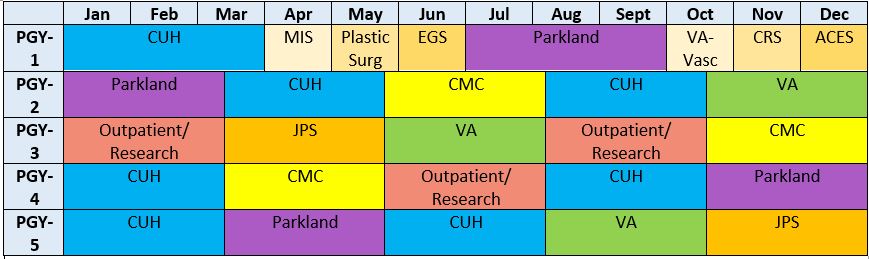
- Sample Resident Rotation Schedule
Optional Content Header - Start with H3
Top row from left to right: Jan, Feb, Mar, Apr, May, Jun, Jul, Aug, Sept, Oct, Nov, Dec
Row two from left to right: PGY-1, January through March would be spent at CUH (Clements University Hospital), April would be spent doing MIS, May would be spent doing Plastic Surgery, June would be spent doing EGS, July through September would be spent at Parkland, October would be spent at VA-Vasc, November would be spent at the CRS, December would be spent at the ACES
Row three from left to right: PGY-2, January through the first half of March would be spent at Parkland, the second half of March through the first 3 weeks of May would be spent at CUH, the last week of May through the first week of August would be spent at Children's Medical Center (CMC), the rest of August through half of October would be spent at CUH, the rest of October through all of December would be spent at the VA
Row four from left to right: PGY-3, January through the first half of March would be spent at outpatient clinics and doing research, the second half of March through the first 3 weeks of May would be spent at John Peter Smith Hospital (JPS), the last week of May through the first week of August would be spent at the VA, the rest of August through half of October would be spent at outpatient clinics and doing research, the rest of October through all of December would be spent at CMC
Row five from left to right: PGY-4, January through the first half of March would be spent at CUH, the second half of March through the first 3 weeks of May would be spent at CMC, the last week of May through the first week of August would be spent at outpatient clinics and doing research, the rest of August through half of October would be spent at CUH, the rest of October through all of December would be spent at Parkland
Row five from left to right: PGY-4, January through the first half of March would be spent at CUH, the second half of March through the first 3 weeks of May would be spent at Parkland, the last week of May through the first week of August would be spent at CUH, the rest of August through half of October would be spent at the VA, he rest of October through all of December would be spent at JPS
