Department of Radiology
Welcome to the Department of Radiology
We are committed to providing comprehensive educational programs to train the next generation of clinicians so they can provide exceptional patient care.
We support 10 research programs and six core facilities with more than 90 dedicated research faculty and lab staff.
We provide more than 1.2 million image interpretations annually to our hospitals and clinics, in addition to image-guided interventional procedures.
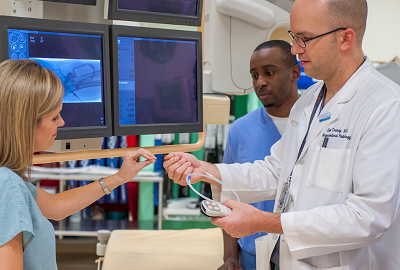
Welcome to the Department of Radiology at UT Southwestern, where state-of-the-art medical imaging meets human caring and compassion.
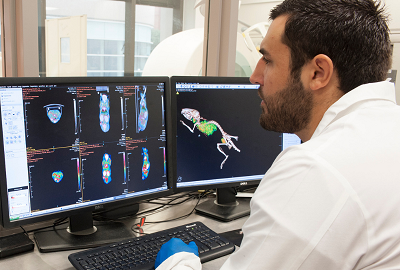
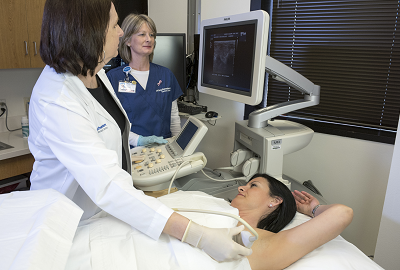
In keeping with the university's mission of providing the very best medical education, patient care and scientific research, we offer an unparalleled level of clinical prowess that covers every known disease and injury and spans 13 divisions. A primary focus of our efforts is the accurate interpretation and insightful and timely reporting of imaging exams. We are fortunate to have specialists who provide high-level interpretation of CT, MRI, PET/CT, radiography, ultrasound and fluoroscopy, as well as vascular and nonvascular interventional procedures.
In the Department of Radiology, our focus is on patient health. At the same time, an array of expanding facilities and programs, supported by excellent basic science and research programs, enables us to offer unique and varied training opportunities to residents and fellows in Radiology.
Our vision
In all that we do, our Department is guided by these six core principles:
- Intellectual vibrancy
- Innovation
- Iteration
- Integrity
- Inspiration
- Impact
Patient imaging services are provided at UT Southwestern Hospitals & Clinics, Parkland Health & Hospital System, Children’s Health℠, and other affiliated hospitals and clinics throughout the region. Each facility offers patients, as well as physicians, residents, fellows, and researchers, access to some of the most advanced imaging technology available.