New drug combo could treat some resistant breast cancers
Mixing two inhibitors killed cells with double mutations in HER2 gene, UT Southwestern study finds
DALLAS – Aug. 24, 2023 – A novel combination of drugs successfully killed breast cells carrying double mutations in the HER2 gene that had rendered them resistant to a commonly used cancer therapy, a study led by UT Southwestern Medical Center researchers showed. The findings, published in Cancer Research, a journal of the American Association for Cancer Research, could lead to new ways to treat patients harboring HER2 mutations, which occur in 5%-7% of metastatic breast cancers.

“We think the drug combination we explored here could be a promising clinical strategy to overcome resistance to HER2 inhibitors for this subset of patients who have double HER2 mutations,” said Ariella B. Hanker, Ph.D., Assistant Professor of Internal Medicine and a member of the Harold C. Simmons Comprehensive Cancer Center at UT Southwestern. She co-led the study with Arnaldo Marín, a visiting M.D./Ph.D. student from the University of Chile who performed his dissertation work under Dr. Hanker’s mentorship.
The HER2 gene encodes a growth factor receptor found on the surface of breast cells. It attracted attention in the late 1980s for its role in breast cancer, and several other cancer types, when it was shown that cells harboring extra copies of this gene – and thus expressing more receptor on their surface – undergo uncontrollable growth. HER2-positive tumors account for about 20% of breast cancer diagnoses. More recently, researchers found that a smaller subset of breast cancer tumors harbor cancer-promoting HER2 mutations that lead to excessive receptor activity. Although these tumors initially respond to HER2-inhibiting drugs, studies have shown that they eventually stop responding after new mutations develop. While several of these secondary HER2 mutations have been identified, how they induce drug resistance and how to overcome this resistance have been unknown.
To answer these questions, Drs. Hanker and Marín and their colleagues genetically altered healthy breast cells to carry one of two different HER2 mutations – known as HER2L869R and HER2L755S – due to their propensity to occur in conjunction with secondary HER2 mutations. They also created three breast cell lines with either of these two HER2 mutations in combination with different secondary mutations. Although the cells with single mutations remained sensitive to neratinib, a drug commonly prescribed to treat HER2-positive tumors, the cells with double mutations were all neratinib-resistant.
To better understand why this resistance occurred, the researchers worked with collaborators at Vanderbilt University to perform computational modeling of the receptor proteins produced by these mutated cells. Their results showed that in double-mutated cells, the resulting HER2 protein was even more active than in cells in which HER2 had a single mutation or no mutations at all. That allowed the double-mutated HER2 protein to more efficiently launch molecular signals that helped cells survive and divide. In addition, the double mutations partially blocked neratinib from binding to HER2 to inhibit it.
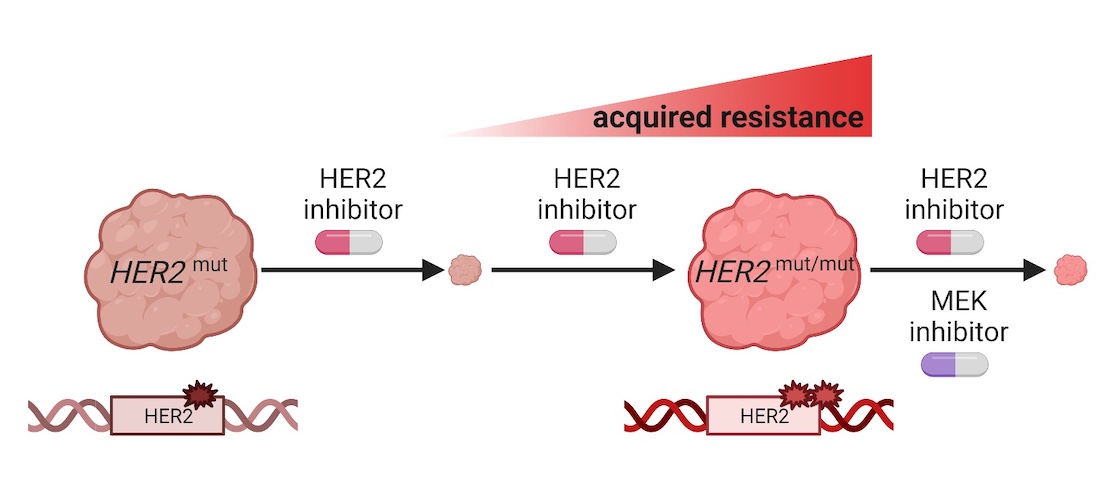
Additional experiments revealed that double-mutated HER2 proteins resisted not only neratinib, but also most other drugs in its class. However, when the researchers treated cells carrying the double mutations with MEK inhibitors, which block one of the signaling pathways turned on when the HER2 growth factor receptor is active, their division slowed, and some of the cells died. This effect was amplified when the MEK inhibitors were combined with neratinib.
Together, Dr. Hanker said, these results suggest that giving patients an MEK inhibitor with a HER2 inhibitor could overcome the resistance to HER2-inhibiting drugs that typically develops with double mutants.
“Both classes of drugs are FDA-approved and have proved safe and tolerable for patients. Our results suggest that using them together to overcome HER2 inhibitor resistance is worth testing in clinical trials,” she added.
Other UTSW researchers who contributed to this study include Carlos L. Arteaga, M.D., Professor of Internal Medicine and Director of the Simmons Cancer Center, and Dan Ye, M.D., Research Scientist. Dr. Arteaga disclosed his financial interests in the manuscript.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
