Simmons Cancer Center, MD Anderson scientists develop artificial intelligence method to predict anti-cancer immunity
Machine learning algorithms are shedding light on neoantigen T cell-receptor pairs
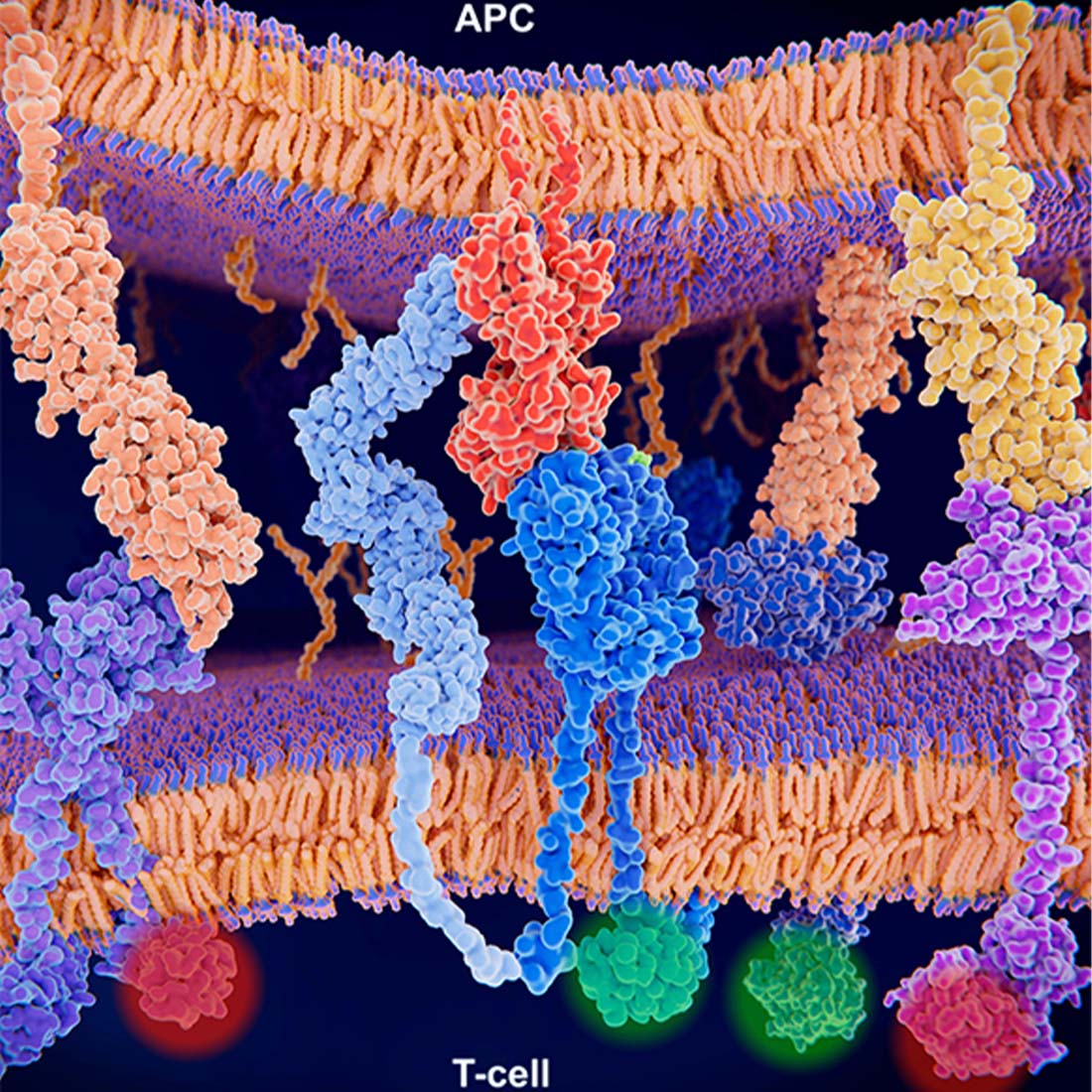
DALLAS – Sept. 23, 2021 – Researchers and data scientists at UT Southwestern Medical Center and The University of Texas MD Anderson Cancer Center have developed an artificial intelligence technique that can identify which cell surface peptides produced by cancer cells called neoantigens are recognized by the immune system.
The pMTnet technique, detailed online in Nature Machine Intelligence, could lead to new ways to predict cancer prognosis and potential responsiveness to immunotherapies.

“Determining which neoantigens bind to T cell receptors and which don’t has seemed like an impossible feat. But with machine learning, we’re making progress,” said senior author Dr. Tao Wang, Ph.D., Assistant Professor of Population and Data Sciences, and with the Harold C. Simmons Comprehensive Cancer Center and the Center for Genetics of Host Defense at UT Southwestern.
Mutations in the genome of cancer cells cause them to display different neoantigens on their surfaces. Some of these neoantigens are recognized by immune T cells that hunt for signs of cancer and foreign invaders, allowing cancer cells to be destroyed by the immune system. However, others seem invisible to T cells, allowing cancers to grow unchecked.
“For the immune system, the presence of neoantigens is one of the biggest differences between normal and tumor cells,” said Tianshi Lu, first co-author with Ze Zhang, doctoral students in the Tao Wang lab, which uses state-of-the-art bioinformatics and biostatistics approaches to study the implications of tumor immunology for tumorigenesis, metastasis, prognosis, and treatment response in a variety of cancers. “If we can figure out which neoantigens stimulate an immune response, then we may be able to use this knowledge in a variety of different ways to fight cancer,” Ms. Lu said.
Being able to predict which neoantigens are recognized by T cells could help researchers develop personalized cancer vaccines, engineer better T cell-based therapies, or predict how well patients might respond to other types of immunotherapies. But there are tens of thousands of different neoantigens, and methods to predict which ones trigger a T cell response have proven to be time-consuming, technically challenging, and costly.
Searching for a better technique with support of grants from the National Institutes of Health (NIH) and Cancer Prevention and Research Institute of Texas (CPRIT), the research team looked to machine learning. They trained a deep learning-based algorithm that they named pMTnet using data from known binding or nonbinding combinations of three different components: neoantigens; proteins called major histocompatibility complexes (MHCs) that present neoantigens on cancer cell surfaces; and the T cell receptors (TCRs) responsible for recognizing the neoantigen-MHC complexes. They then tested the algorithm against a dataset developed from 30 different studies that had experimentally identified binding or nonbinding neoantigen T cell-receptor pairs. This experiment showed that the new algorithms had a high level of accuracy.
The researchers used this new tool to gather insights on neoantigens cataloged in The Cancer Genome Atlas, a public database that holds information from more than 11,000 primary tumors. pMTnet showed that neoantigens generally trigger a stronger immune response compared with tumor-associated antigens. It also predicted which patients had better responses to immune checkpoint blockade therapies and had better overall survival rates.
“As an immunologist, the most significant hurdle currently facing immunotherapy is the ability to determine which antigens are recognized by which T cells in order to leverage these pairings for therapeutic purposes,” said corresponding author Alexandre Reuben, Ph.D., Assistant Professor of Thoracic-Head & Neck Medical Oncology at MD Anderson. “pMTnet outperforms its current alternatives and brings us significantly closer to this objective.”
Other UTSW researchers who contributed to this study include James Zhu, Yunguan Wang, Xue Xiao, and Lin Xu. Other MD Anderson scientists who contributed to this work include Peixin Jiang, Chantale Bernatchez, John V. Heymach, and Don L. Gibbons. Dr. Jun Wang from NYU Langone Health also contributed to this work.
UT Southwestern’s Simmons Cancer Center and MD Anderson are among the exclusive 51 designated comprehensive centers with the National Cancer Institute, which includes a joint effort with the National Human Genome Research Institute to oversee The Cancer Genome Atlas project. The study was supported by the NIH (grants 5P30CA142543/TW and R01CA258584/TW), CPRIT (RP190208/TW), MD Anderson (Lung Cancer Moon Shot), the University Cancer Foundation at MD Anderson, the Waun Ki Hong Lung Cancer Research Fund, Exon 20 Group, and Rexanna’s Foundation for Fighting Lung Cancer.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
