Multidisciplinary care improves outcomes of patients with brain metastases
Study shows life expectancy moved from months to years
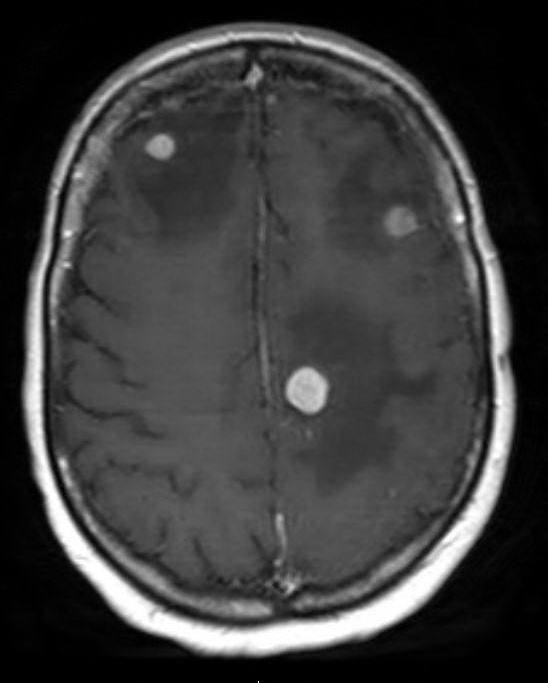
DALLAS – Dec. 5, 2018 – New data reveals the life expectancy of patients with kidney cancer that’s traveled to the brain has now stretched from months to years. UT Southwestern Kidney Cancer Program investigators report survival rates beyond 2.5 years for some patients with specialized multidisciplinary care.
Historically, patients whose kidney cancer had spread to the brain were believed to have only about six months to live, and patient care was often focused on comfort and pain relief. Patients with multiple tumors had especially poor prognosis. But with advances in brain surgery and new radiation treatments, survival rates are similar to those of patients without brain metastases, the UT Southwestern Medical Center researchers found.
Two companion reports described the outcomes of 56 patients with renal cell carcinoma that presented with brain metastases or were diagnosed with them shortly thereafter (during first line therapy). In the first report, investigators found that modern treatment allowed for good survival even for patients with five or more tumors. The second report compared the same 56 patients to matched control patients without brain metastases similarly treated at UT Southwestern, there was no significant difference in survival between the two groups.
Furthermore, life expectancy for the majority of patients (except for those with poor-risk disease) often extended beyond 2.5 years.
The investigators attribute these results to advances in radiation therapy, neurosurgery, and a team approach. Quite often, treatment at UT Southwestern involves radiosurgery – highly focused, precisely delivered, high-dose radiation. In the studies, soon to be published in the journal Clinical Genitourinary Cancer, the authors report upwards of 90 percent of brain metastases were under control at one year when treated with radiosurgery. These results are based on treatment of 177 brain metastases.

In some patients, more than 20 such brain metastases were treated by skilled radiation oncologists, said Dr. Robert Timmerman, senior author of one of the two studies and Professor of Radiation Oncology and Neurological Surgery. Dr. Timmerman holds the Effie Marie Cain Distinguished Chair in Cancer Therapy Research.
Advances in neurosurgery as well as in systemic therapies are also likely contributors to these improved results.
“In the past, it was a bad sign when someone presented with brain metastases, but with newer therapies, both systemic and local, patient survival rates are similar between those with and without brain metastases,” said the first author of the other manuscript, Dr. Alex Bowman, Assistant Professor of Internal Medicine and a member of the Kidney Cancer Program of the Harold C. Simmons Comprehensive Cancer Center.
“These results reflect our multidisciplinary approach and, in particular, the skill of our radiation oncologists and neurosurgeons,” said senior author Dr. James Brugarolas, Professor of Internal Medicine and Director of the Kidney Cancer Program at UT Southwestern.
“We believe that most patients with brain metastases deserve aggressive treatment and we are pleased to be able to deliver this level of care to our patients,” said Dr. Brugarolas, who holds the Sherry Wigley Crow Cancer Research Endowed Chair in Honor of Robert Lewis Kirby, M.D. These results likely contribute to the improved survival rates of stage 4 kidney cancer patients at the UT Southwestern Kidney Cancer Program, which are more than double national benchmarks.
Approximately 170,000 cases of brain metastases in patients with metastatic renal cell carcinoma occur each year.

Other UT Southwestern faculty members who contributed to the studies include: Dr. Samuel Barnett, Professor of Neurological Surgery and Otolaryngology; Dr. Kevin Courtney, Assistant Professor of Internal Medicine; Dr. Hans Hammers, Associate Professor of Internal Medicine; and Dr. Raquibul Hannan, Associate Professor of Radiation Oncology and Immunology; Dr. Bruce Mickey, Professor of Neurological Surgery, Otolaryngology, and Radiation Oncology; Dr. Lucien Nedzi, Associate Professor of Radiation Oncology; Dr. Toral Patel, Assistant Professor of Neurological Surgery, and Neurology and Neurotherapeutics; Dr. Strahinja Stojadinovic, Associate Professor of Radiation Oncology and in the School of Health Professions; Dr. Zabi Wardak, Assistant Professor of Radiation Oncology; and Dr. Tony Whitworth, Professor of Neurological Surgery and Radiation Oncology.
Dr. Barnett holds the Trammell Crow Professorship in Neurosurgery and Dr. Mickey holds the William Kemp Clark Chair in Neurological Surgery. Dr. Hammers is a Eugene P. Frenkel, M.D., Scholar in Clinical Medicine.
The Harold C. Simmons Comprehensive Cancer Center, one of 49 NCI-designated Comprehensive Cancer Centers in the U.S. and the only one in North Texas, is among just 30 U.S. cancer research centers to be designated by the NCI as a National Clinical Trials Network Lead Academic Participating Site.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty has received six Nobel Prizes, and includes 22 members of the National Academy of Sciences, 17 members of the National Academy of Medicine, and 15 Howard Hughes Medical Institute Investigators. The faculty of more than 2,700 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in about 80 specialties to more than 105,000 hospitalized patients, nearly 370,000 emergency room cases, and oversee approximately 2.4 million outpatient visits a year.