Scientists use parasite’s internal clock to attack sleeping sickness
DALLAS – The parasite that causes deadly sleeping sickness has its own biological clock that makes it more vulnerable to medications during the afternoon, according to international research that may help improve treatments for one of Africa’s most lethal diseases.
The finding from the Peter O’Donnell Jr. Brain Institute could be especially beneficial for patients whose bodies can’t handle side effects of toxic treatments used to eradicate the parasite. By knowing the optimal time to administer these medications – which can be fatal – doctors hope to reduce the duration and dosage of the treatment and save more lives.

“This research has opened a door,” said Dr. Filipa Rijo-Ferreira, first author of the study from the O’Donnell Brain Institute at UT Southwestern Medical Center. “If the same therapeutic effect can be obtained with a lower dose, then it may be possible to reduce the mortality associated with the treatment.”
Establishing that parasites have their own internal clock is a key step in finding new ways to treat a variety of parasitic conditions, from sleeping sickness to malaria. While many of these diseases are often not deadly, sleeping sickness has been among the most lethal.
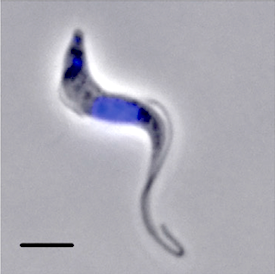
The condition – known formally as African trypanosomiasis – is transmitted through the bite of the Tsetse fly and threatens tens of millions of people in sub-Saharan African countries. After entering the body, the parasite causes such symptoms as inverted sleeping cycles, fever, muscle weakness, and itching. It eventually invades the central nervous system and, depending on its type, can kill its host in anywhere from a few months to several years.
Control efforts have significantly reduced the number of cases over the last decade. However, an unknown number of people still die annually from sleeping sickness as scientists continue seeking a vaccine and alternative treatments to the arsenic-based medications that are occasionally fatal to patients.
Dr. Joseph S. Takahashi, who oversaw the collaborative study published in Nature Microbiology with Dr. Luisa Figueiredo at the University of Lisbon in Portugal, said the finding will likely apply to all types of parasites and perhaps lead to improved treatment for their associated conditions.

“There have been many observations of the presence of daily patterns in parasites, but until now we didn’t know if this was the result of an intrinsic molecular clock. In the future, we may consider biological rhythms when defining therapies to treat sleeping sickness and potentially other infections,” said Dr. Takahashi, Chairman of Neuroscience at UT Southwestern, holder of the Loyd B. Sands Distinguished Chair in Neuroscience.
Researchers from UT Southwestern and the Institute of Molecular Medicine at the University of Lisbon in Portugal made their finding after isolating the parasite – known as Trypanosoma brucei – in the lab and obtaining a type of genetic fingerprint to gauge its daily cycles independent of a host. They found the parasite has daily metabolic cycles that make it more vulnerable to treatments in the afternoon.
Parasite Extras
|
Scientists now hope to learn what drives the parasite’s internal clock so they can target specific genes and disrupt its circadian rhythms. Much like humans struggle to cope when their sleep cycle is interrupted, scientists expect the parasite would become weaker if its cycle is disturbed.
“We know that in other organisms if we mutate their clock they are less adapted to the world,” said Dr. Rijo-Ferreira, an HHMI Associate. “We’re trying to jetlag these parasites, trying to make them less fit.”
The work was supported by an HHMI International Early Career Scientist award, and EMBO Installation Grant, and Foundation for Science and Technology awards.
5 parasite diseases to watch for in the U.S.
Illustration courtesy of Fernando Augusto.
While deadly sleeping sickness is primarily transmitted in rural regions of Africa, millions of people in the U.S. are exposed to other forms of parasitic diseases. Here are five such diseases the U.S. Centers for Disease Control and Prevention lists as public-health priorities. ChagasChagas disease is most commonly acquired through contact with the feces of an infected kissing bug, a blood-sucking insect. There may be swelling where the parasite enters the body, and in rare cases the disease results in life-threatening inflammation of the heart or brain. If untreated, infection is lifelong. CDC estimates about 300,000 people in the U.S. have the condition. ToxoplasmosisThis condition is a leading cause of death related to food-borne illness in the U.S. More than 30 million Americans carry the parasite, though few show symptoms because their immune systems protect against the illness. People can become infected by eating undercooked, contaminated meat, and women who are infected during pregnancy sometimes pass the parasite to their unborn children. This transfer can result in a miscarriage, a stillborn child, eye disease, or unusual head size. ToxocariasisToxocariasis is caused by two species of roundworm and is typically spread through the feces of dogs and cats. Most infected people don’t show symptoms, though in some cases the parasite can travel through parts of the body such as the liver, lungs, or central nervous system. The larvae can also travel to the eye and cause blindness. Each year about 70 people, mostly children, are blinded by the condition. CysticercosisCysticercosis is spread through ingesting larval cysts of a tapeworm, causing infections in the muscles, brain, or other tissue. People become infected when they drink water or eat food contaminated with tapeworm eggs, or if they put contaminated fingers in their mouths. Cysts in the brain or spinal cord commonly cause seizures or headaches. The condition may also cause life-threatening brain swelling or strokes. CDC estimates that at least 1,000 people are hospitalized each year with the more severe brain-related form of the disease. TrichomoniasisThe parasite that causes trichomoniasis is transferred from human to human during sex. About 3.7 million people in the U.S. have the condition, though most do not know they have it. Symptoms may include itching, burning, redness or soreness in the infected areas. The parasite can be eradicated through medications. Without treatment, the infection can last for months or years. Source: U.S. Centers for Disease Control and Prevention. |
About UT Southwestern Medical Center
UT Southwestern, one of the nation's premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution's faculty members have received six Nobel Prizes and include 26 members of the National Academy of Sciences, 20 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,100 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in more than 80 specialties to more than 120,000 hospitalized patients, more than 360,000 emergency room cases, and oversee nearly 5 million outpatient visits a year.
###
Media Contact: James Beltran
214-648-3404
James.Beltran@utsouthwestern.edu
To automatically receive news releases from UT Southwestern via email, subscribe at www.utsouthwestern.edu/receivenews