Study links cancer metabolism to DNA replication errors
Inhibiting cellular process called lipoylation makes cancer cells more vulnerable to existing class of drugs known as PARP inhibitors, UTSW study shows
DALLAS – May 01, 2026 – Loss of an enzyme necessary for a process called lipoylation disrupts the way cancer cells copy their DNA, increasing their vulnerability to a class of anticancer drugs known as PARP inhibitors, a study led by UT Southwestern Medical Center researchers shows. The findings, published in Science Advances, reveal a previously unrecognized mechanism to protect DNA replication and genome stability that could lead to new treatments for some cancers.

“This study shows that metabolism doesn’t just fuel cancer cells – it also directly shapes how DNA is copied and protected. This helps explain why inhibiting lipoylation could make tumors especially sensitive to PARP inhibitors,” said Yuanyuan “Faith” Zhang, M.D., Ph.D., Assistant Professor of Radiation Oncology and a member of the Experimental Therapeutics Research Program in the Harold C. Simmons Comprehensive Cancer Center at UT Southwestern. Dr. Zhang co-led the study with first author Zengfu Shang, Ph.D., Assistant Professor of Radiation Oncology in the Zhang Lab.
Lipoylation is a process in which an enzyme called LIPT1 adds lipoic acid to other enzymes in the energy-producing organelles known as mitochondria. In 2025, Dr. Zhang, Dr. Shang, and their colleagues showed that blocking lipoylation with a drug called CPI-613 enhanced the effect of radiation in preclinical models of lung cancer. That study showed that this effect stemmed from problems in DNA damage repair.
To better understand this phenomenon, researchers used gene editing to delete the LIPT1-producing gene in three different cell lines. Each altered cell line multiplied significantly slower and formed fewer colonies than unaltered cells. Further investigation suggested that this behavior was due to replication stress, an impaired ability of cells to copy their DNA in preparation for cell division.
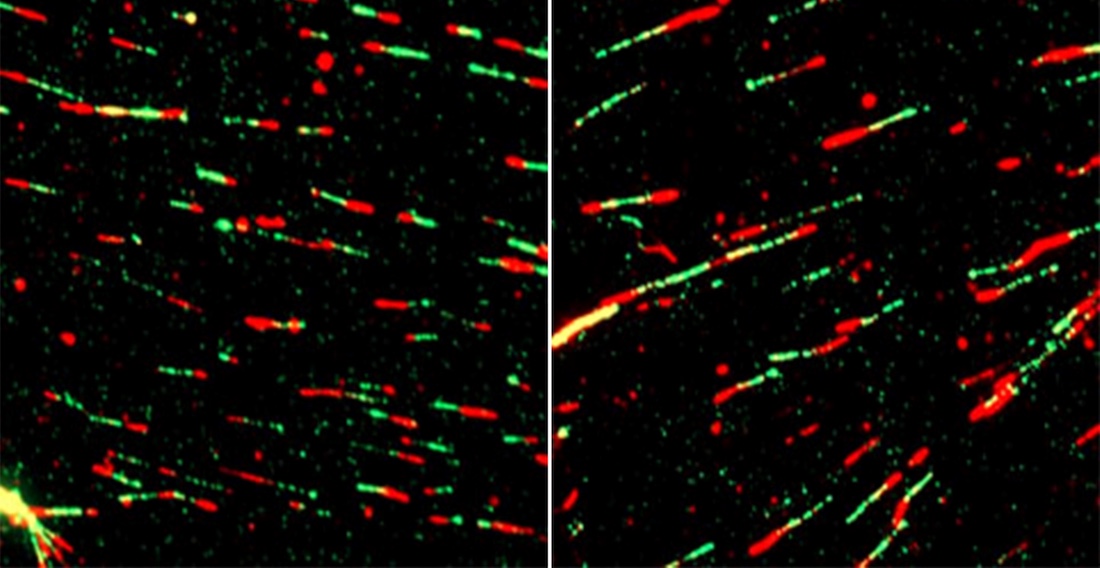
Further experiments showed that deleting LIPT1 led to an accumulation of the metabolite 2-hydroxyglutarate, which caused DNA to become tightly compacted in cell nuclei. In turn, this slowed new DNA synthesis at replication forks, structures in which double strands of DNA separate to begin the copying process. The cells’ attempt to restart the stalled replication fork subsequently prompted the formation of single-strand DNA breaks that necessitated repair with another protein known as poly (ADP-ribose) polymerase 1, or PARP1.

PARP1 is a known target for PARP inhibitors, a class of cancer-fighting drugs, Dr. Shang explained. When the team treated cells missing LIPT1 with a PARP inhibitor, the cancer cells couldn’t repair their damaged DNA, a deficit that proved lethal.
Drs. Zhang and Shang said that low levels of LIPT1, frequently present in some cancer types, could potentially serve as a biomarker for sensitivity to PARP inhibitors. Similarly, combining CPI-613 – a lipoylation inhibitor designated as an orphan drug by the Food and Drug Administration with well-documented safety data in cancer patients – with PARP inhibitors could offer a new strategy for treating non-small cell lung cancers and other cancer types with low LIPT1. The team plans to investigate both possibilities in future studies.
Other UTSW researchers who contributed to this study are Anthony J. Davis, Ph.D., Associate Professor of Radiation Oncology; Ching-Cheng Hsu, Ph.D., Research Associate; Jui-Chung Chiang, Ph.D., postdoctoral fellow; and Ciara Newman, B.S., a former research assistant who is now a graduate student researcher.
This study was funded by a Lung SPORE Career Enhancement Award; a Distinguished Researcher Award from the President’s Research Council; an Institutional Research Grant from the American Cancer Society (IRG-21-142-16); a National Cancer Institute (NCI) Cancer Center Support Grant (P30CA142543); awards from the National Center for Advancing Translational Sciences of the National Institutes of Health (KL2TR003981 and CTSA-PP-YR1-D-009); a Startup Award from UT Southwestern Department of Radiation Oncology; a Disease-Oriented Clinical Scholar Award from UT Southwestern; and grants from the National Institutes of Health (R01CA276058 and R01CA29290), the Department of Energy (DE-SC0025578), and the National Aeronautics and Space Administration (20-20HHCSR_2-0033).
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 27 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of nearly 3,400 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
