Is vaping more harmful than smoking cigarettes? More people incorrectly think so
Rising perceptions of health risks associated with e-cigarettes have public health implications, UTSW study shows
DALLAS – March 11, 2026 – A growing number of U.S. adults consider electronic cigarettes (e-cigarettes) more harmful than conventional cigarettes, UT Southwestern Medical Center researchers show in a study. The findings, published in Nicotine and Tobacco Research, could have significant implications for public health policymakers, tobacco control strategies, and people who use either of these cigarette types.

“The perception that e-cigarettes are more harmful than cigarettes has been linked to both a decreased willingness to use e-cigarettes for smoking cessation and an increased likelihood of switching from vaping to smoking. Understanding the ramifications of this perception change represents a critical consideration when developing cessation strategies,” said David Gerber, M.D., Professor of Internal Medicine and in the Peter O’Donnell Jr. School of Public Health and Co-Director of the Office of Education and Training in the Harold C. Simmons Comprehensive Cancer Center at UT Southwestern.
Dr. Gerber co-led the study with Cristina Thomas, M.D., Assistant Professor of Dermatology and Internal Medicine, and Alexander Wu, B.S., a medical student at UTSW and the study’s first author.
Cigarette smoking has declined significantly over the past few decades, from a historical peak in 1965 when 43% of U.S. adults reported smoking to about 12% in 2025, according to the Centers for Disease Control and Prevention. However, since e-cigarettes, or “vapes,” were introduced in the U.S. in 2006, their use has steadily grown: Nearly 7% of U.S. adults reported using these devices in 2025.

According to physicians, e-cigarettes are generally thought to be less harmful than conventional cigarettes, which are known to cause cardiovascular disease, pulmonary disease, and several forms of cancer, Dr. Thomas explained. However, a growing awareness of e-cigarettes’ hazards – including exposure to high levels of addictive nicotine and toxic chemicals as well as a propensity to act as a gateway for conventional cigarette smoking – led the Food and Drug Administration to include e-cigarettes in its 2018 anti-smoking campaign aimed at youth called “The Real Cost.” A year later, an outbreak of e-cigarette or vaping product use-associated lung injury (EVALI) occurred, affecting the health of thousands of e-cigarette users.
To learn how these events may have affected public perception of e-cigarettes, Mr. Wu and his colleagues analyzed data from the Health Information Nation Trends Survey (HINTS) from 2012 to 2022. This cross-sectional, nationally representative survey sponsored by the National Cancer Institute collects a variety of health data each year.

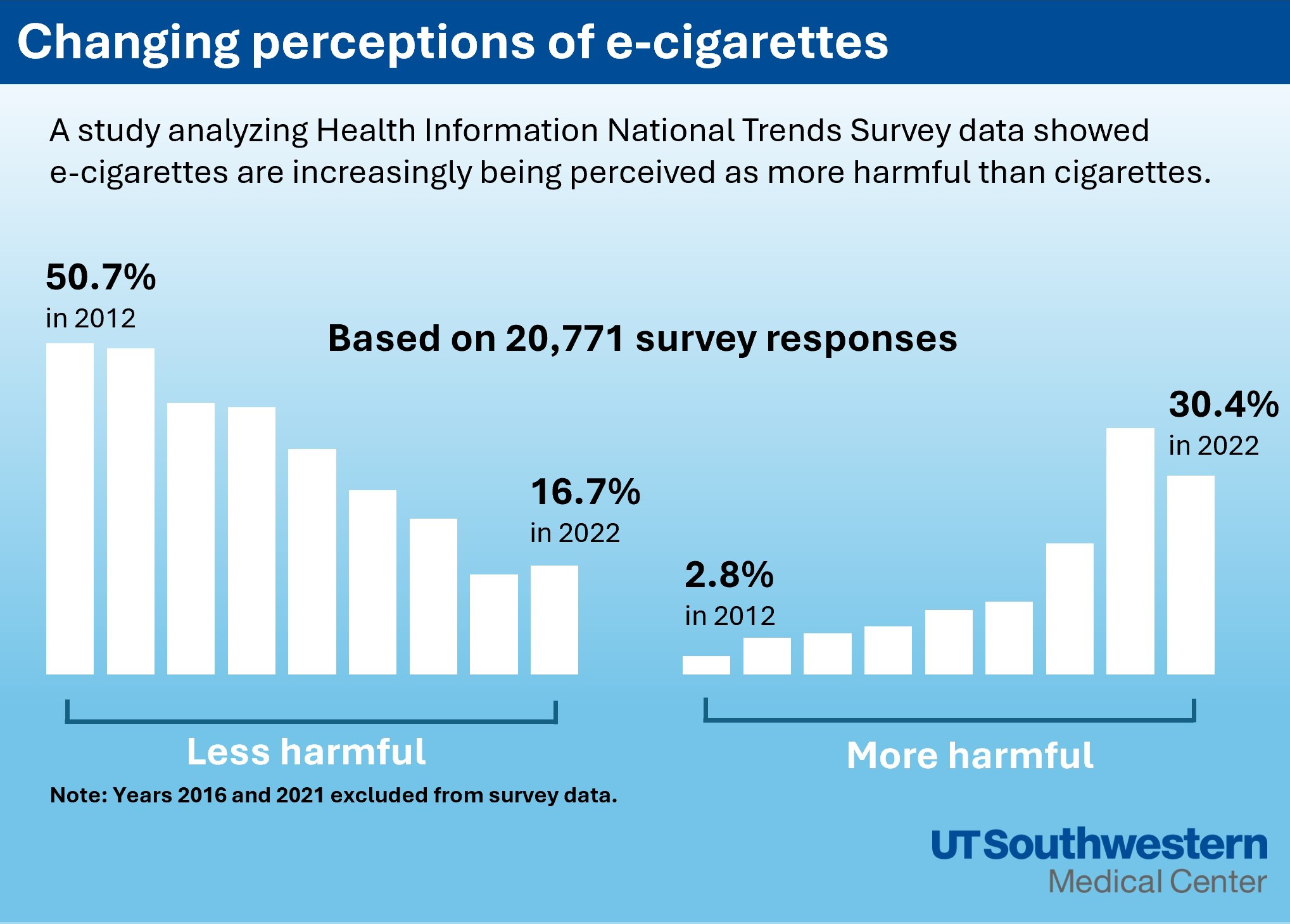
Using answers from 20,771 survey respondents, the researchers found that the proportion perceiving e-cigarettes as more harmful than conventional cigarettes rose from nearly 3% in 2012 to more than 30% in 2022. Similarly, perceptions of e-cigarettes as less harmful decreased from nearly 51% in 2012 to about 17% in 2022. An analysis of data collected before and after “The Real Cost” campaign and the EVALI outbreak suggests that these events negatively affected public perceptions of e-cigarettes, Mr. Wu said.
“Understanding how events like this shape people’s beliefs is key to guiding public health policy and future tobacco control strategies,” Mr. Wu said.
Although e-cigarettes are not harmless, Dr. Gerber added, clinicians widely consider them a less harmful alternative to conventional cigarettes. Research has shown that using e-cigarettes to help quit smoking increases the chances of success compared with other nicotine replacements such as patches, lozenges, and gum when combined with behavioral therapy. Negative public perceptions of e-cigarettes might steer people away from using them as a smoking cessation tool or encourage them to choose conventional cigarettes over e-cigarettes, a topic the team plans to explore in future research.
“Our findings show the need to strike a balance in public health messaging that discourages youths from using either product while also ensuring that adults who do smoke have access to accurate information about product risks and cessation options,” Dr. Thomas said.
Other UTSW researchers who contributed to this study are Sandi L. Pruitt, Ph.D., M.P.H., Professor in the O’Donnell School of Public Health and Associate Director of the Office of Community Outreach and Engagement in the Simmons Cancer Center; Chul Ahn, Ph.D., Professor in the O’Donnell School of Public Health and Director of the Biostatistics Shared Resource Core in the Simmons Cancer Center; David Balis M.D., Professor of Internal Medicine; John D. Minna, M.D., Director of the Hamon Center for Therapeutic Oncology Research, Professor of Internal Medicine and Pharmacology, and co-leader of the Experimental Therapeutics Research Program in the Simmons Cancer Center; and Sumin Son, B.A., and Matthew Lee, B.S., medical students.
Dr. Gerber holds the David Bruton, Jr. Professorship in Clinical Cancer Research.
This study was supported in part by the Harold C. Simmons Comprehensive Cancer Center Biostatistics Shared Resource (5P30 CA142543).
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
