Neuro-Oncology
Leadership

Justin Jordan, M.D., M.P.H, FAAN
Section Head
Contact
Maureen Edwards
Academic Administrator
maureen.edwards@utsouthwestern.edu
Patient Appointments
214-645-8800
Book Online
The Neuro-Oncology section embodies the core missions of the Department of Neurology, including excellence in patient care, promoting education, and advancing research in tumors of the nervous system and cancer-related neurological disorders. Our faculty are recognized nationally and internationally for their academic contributions to the field of neuro-oncology.
The Harold C. Simmons Comprehensive Cancer Center, home to the neuro-oncology clinic, is the only National Cancer Institute (NCI)-designated comprehensive cancer center in North Texas. The faculty employ a patient-centric approach, blending innovative cancer research with conventional cancer care.
Faculty
We have six outstanding neuro-oncology faculty members, committed to advancing research, education, and clinical care. Four of those faculty lead extramurally funded research laboratories and are accelerating science through discoveries of novel therapeutic strategies for glioblastoma, engineering nanoparticles to overcome blood-brain barrier limitations of drug delivery, and identifying novel methods of targeting metabolic vulnerabilities in IDH-mutant gliomas. The neuro-oncology section is also home to one of the largest repositories of clinically annotated patient-derived xenograft (PDX) models, which give insight into how genetic mutations influence tumor phenotypes. The collective knowledge of our faculty contributes significantly to the field of neuro-oncology, and our faculty are widely regarded as leaders in their field.
View all faculty Join Our Team
Neuro-Oncology Highlights
3600+
Patient visits annually
700
Patient operations performed by neurosurgery
1
NCI-designated comprehensive cancer center (only in North Texas)
6
Faculty
4
Faculty with extramural funding
4
Subspecialty Clinics
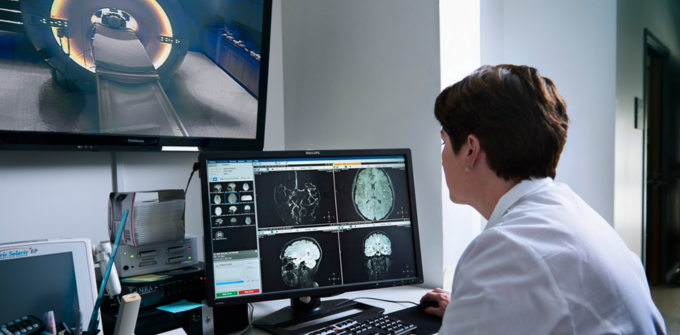
Subspecialty Care
While we pride ourselves on comprehensive care for all patients with neuro-oncologic diagnoses, our faculty lead four specialty clinics: the multidisciplinary glioma clinic, neurofibromatosis and schwannomatosis clinic, cancer prevention and screening clinic, and a procedure clinic.
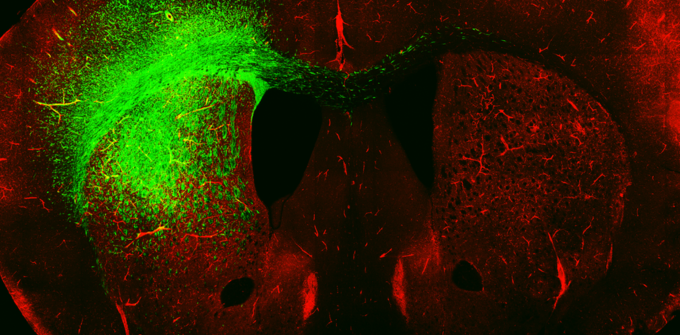
Research
Physicians and scientists within the Neuro-oncology section focus on a range of clinical and basic research topics. Clinical research activities focus on low- and high-grade gliomas, leptomeningeal disease, novel tumor mutations, neurofibromatosis, schwannomatosis, and health disparities. Basic science research investigates the mechanisms of tumor cell biology, including signal transduction pathways involved in cancer pathogenesis and the genetic drivers of oncogenesis, as well as novel strategies to target metabolic vulnerabilities in gliomas. Faculty research on IDH inhibitors and their efficacy in treating IDH mutant gliomas has informed the National Comprehensive Cancer Network guidelines for this disease. Their work in the imaging field has also been instrumental in utilizing non-invasive imaging techniques to identify patients with IDH mutant tumors through the evaluation of 2HG signaling.
Further, the neuro-oncology section has a strong track record of clinical trial enrollment to provide novel therapies to our patients. With >35 patients enrolled in therapeutic clinical trials per year, we strive to bring the most innovative and promising therapies to our patients, while also contributing to the global acceleration of therapeutic discovery.

Our Reach Within the Community
Head for the Cure, an annual spring walk is a well-attended fundraising event. A portion of the funds are directed to our research team to bring novel therapies from bench concepts to the bedside.
National Brain Tumor Society - Fireside Chats occur once every 6 months to 1 year, where clinical trials are discussed offering insight to community members interested in supporting research. The society funds clinical research activities and community engagement activities. They also provide dedicated support group assistance to patients and caregivers.
Grey Matters, is a local neuro-oncology support group for UT Southwestern brain tumor patients and faculty.

