Simple blood test may predict abnormal bone growth early
UT Southwestern researchers helped develop method to detect heterotopic ossification days after trauma or surgery
DALLAS – March 24, 2026 – Researchers at UT Southwestern Medical Center are part of a team that developed a simple blood test that can detect heterotopic ossification (HO), the abnormal formation of bone in soft tissues after injury or surgery, weeks before it can be identified by traditional imaging. Their findings, published in Nature Communications, could potentially lead to earlier treatment for patients at risk.
HO develops in muscles, tendons, or other soft tissues in a significant proportion of trauma and joint replacement patients when the body’s natural repair response overcorrects or is misdirected. Symptoms can include pain, swelling, joint stiffness, reduced range of motion, and the formation of misplaced bone.
“Heterotopic ossification is a fairly common complication of trauma and some types of surgery,” said co-corresponding author Benjamin Levi, M.D., Professor of Surgery and Chief of the Division of Burn, Trauma, Acute and Critical Care Surgery at UT Southwestern.

“The body is working overtime to repair itself, and if those efforts are short-circuited at the cellular level, it leads to bone growth where there shouldn’t be any. Rather than waiting six to eight weeks for bone to appear on a CT scan or X-ray as we do today, our findings suggest that clinicians could identify molecular changes that lead to HO within hours to days after injury or surgery,” said Dr. Levi, who also serves as Director of UTSW’s Center for Organogenesis, Regeneration, and Trauma.
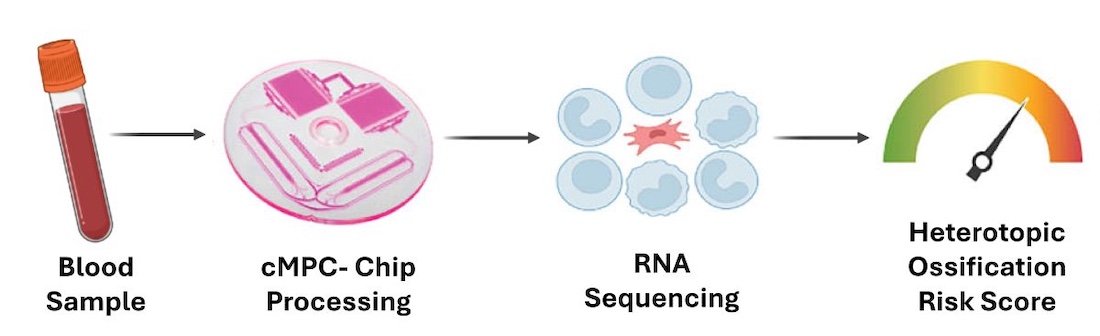
UTSW researchers and colleagues at Massachusetts General Hospital in Boston focused on rare cells in the blood – known as circulating mesenchymal progenitor cells (cMPCs) – that are involved in abnormal bone formation. Using blood samples from trauma-induced mouse models and UT Southwestern patients who had undergone hip replacement surgery, the researchers isolated these cells using a microfluidic device called an iChip. They then analyzed the cells’ gene expression to build a risk prediction model that was 90% successful in identifying HO formation.
The test also could be used to monitor treatment response by detecting reductions in HO risk after clinical intervention – usually physical therapy, radiation, pain medication, or surgery.
“Currently, up to 80% of patients who don’t have HO receive unnecessary preventive treatment such as radiation or nonsteroidal anti-inflammatory drugs after trauma or surgery because of the delay in identifying HO via traditional imaging,” said Johanna Nunez, M.D., UTSW Burn Surgery and Critical Care fellow, previous Sons of the Flag fellow, and the study’s first author. “A blood-based ‘liquid biopsy’ tool like this could allow early identification, reducing complications, costs, overtreatment, and associated risks while improving precision, monitoring, and safety.”

The study is an extension of previous research the Levi Lab has conducted on the pathology and treatment of heterotopic ossification. The new diagnostic test, which has a patent pending, will undergo additional research to further evaluate its effectiveness.
“While this study focused on HO after trauma, burns, or joint replacements, it’s possible that the blood test platform could be used with other disorders involving abnormal tissue repair, such as osteoarthritis and fibrosis-related conditions,” said Dr. Levi, who holds secondary appointments in the Charles and Jane Pak Center for Mineral Metabolism and Clinical Research, Children’s Medical Center Research Institute at UT Southwestern (CRI), and Plastic Surgery.
Other UTSW researchers who contributed to this study are Antonia Chen, M.D., M.B.A., Chair and Professor of Orthopaedic Surgery; Alexandra Callan, M.D., Associate Professor of Orthopaedic Surgery; Robert Tower, Ph.D., Assistant Professor of Surgery and in the Charles and Jane Pak Center for Mineral Metabolism and Clinical Research and the Eugene McDermott Center for Human Growth and Development; Heeseog Kang, Ph.D., Assistant Professor of Surgery; Elise Jeffery, Ph.D., Research Scientist in the Morrison Lab and CRI; and Sneha Korlakunta, B.A., Data Scientist; Chase Pagani, Research Assistant and M.D./Ph.D. student; and Achira Shah, M.S., Research Assistant II, all from Surgery and the Center for Organogenesis, Regeneration, and Trauma.
Dr. Levi holds the Dr. Lee Hudson-Robert R. Penn Chair in Surgery.
This research received funding from Shriners Hospitals for Children, MGH ECOR, Orphan Disease Center, and the National Institutes of Health (R61AR078072/R33AR078072 and R01AR078324).
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
