UT Southwestern researchers identify risk factors for unsuccessful bunion surgery
Findings could help surgeons counsel patients on common elective procedure
DALLAS – Jan. 31, 2023 – A study by UT Southwestern researchers has identified three factors that increase the risk that bunion surgery will fail to fix this painful foot condition. The findings, published in The Journal of Foot and Ankle Surgery, provide information that surgeons can use to counsel patients considering this elective procedure.

“If we know the factors that lead to nonunion, when the bones don’t fuse successfully, we can educate patients who may have higher risk of an unsuccessful outcome for this operation,” said study leader Matthew J. Johnson, D.P.M., Assistant Professor of Orthopaedic Surgery at UT Southwestern.
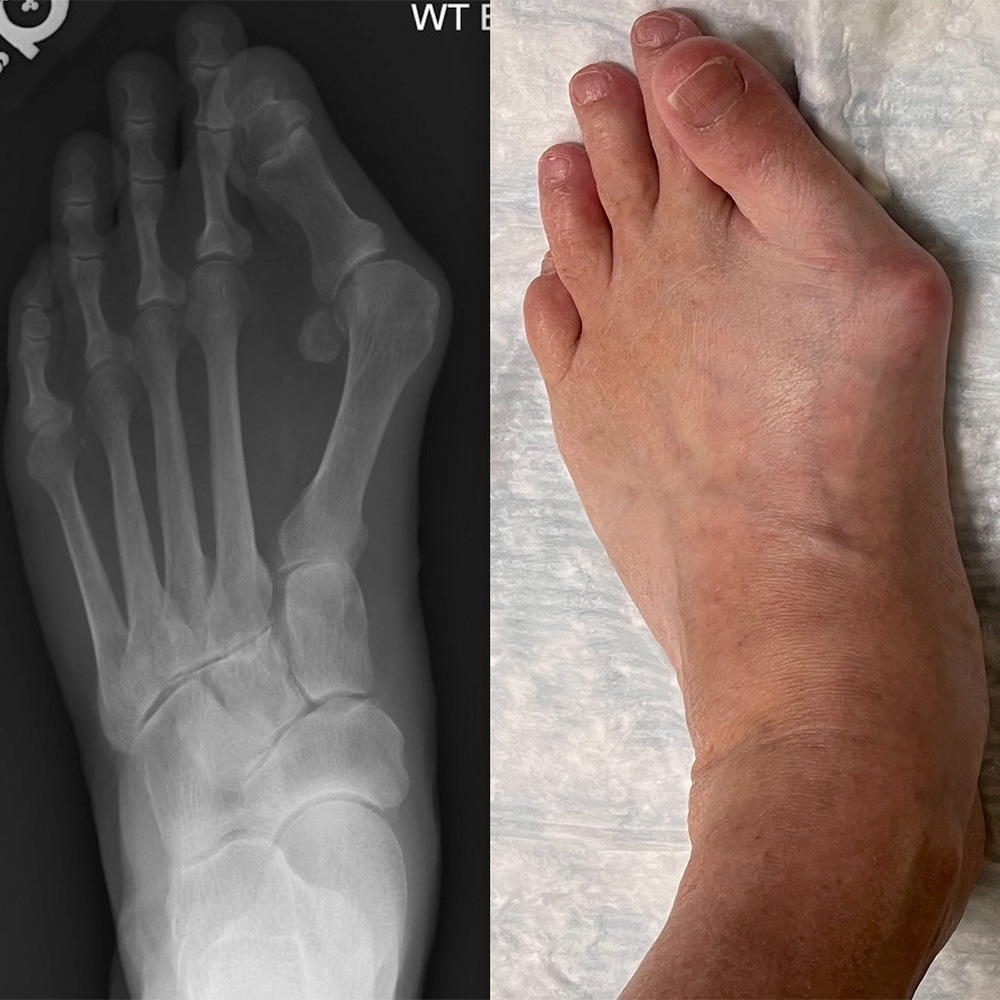
Up to one-third of American adults have bunions, a painful bump that forms on the base of the big toe when the long metatarsal bone shifts toward the inside of the foot and the phalanx bones of the big toe angle toward the second toe. The cause of this common chronic deformity has been linked to ill-fitting shoe wear, genetics, and the biomechanics of the foot. Bunions can be extremely painful, Dr. Johnson explained, because they cause the foot’s soft tissue to rub against shoes, making walking difficult. Although there are nonsurgical treatments such as shoes with a wider toe box or padding for the bunion, these rarely relieve pain significantly, necessitating surgery for many patients.
At UT Southwestern and many other U.S. hospitals, bunions can be corrected through a method called the modified Lapidus procedure, in which surgeons straighten and fuse the misaligned bones making up the first tarsometatarsal joint. However, in about 10% of these surgeries, the bones don’t permanently fuse. It’s called a nonunion. When a nonunion results, the patient may experience continued pain and dysfunction, and surgical revision may be needed.
To better understand which patients are at risk for nonunion, Dr. Johnson and his colleagues examined the medical records of 222 patients from UTSW and Parkland Health who received a modified Lapidus procedure to correct their bunions. They collected data on a variety of patient characteristics, including age, sex, body mass index, prior bunion surgery, history of tobacco use, any diagnosis of diabetes mellitus or hypothyroidism, and the particulars of their fusion procedure, such as the number of screws or plates used.
Their findings showed that the risk of nonunion significantly increased with prior bunion surgery, higher body mass index, and a bigger preoperative angle of their bunions (a marker of the deformity’s severity). Dr. Johnson said that although previous studies have suggested that smoking could affect bunion surgery success, tobacco use had no significant effect on nonunion risk in their study. The number of screws or plates used also had no bearing on union success.
“Understanding these factors that may hinder achieving optimal results for bunion surgery can help us address them for more successful outcomes in the future,” Dr. Johnson said.
Other UTSW researchers who contributed to this study include Benjamin Wang, Kshitij Manchanda, Trapper Lalli, Dane K. Wukich, George Tye Liu, Katherine Raspovic, Michael VanPelt, and Paul A. Nakonezny.
Dr. Wukich holds the Dr. Charles F. Gregory Distinguished Chair in Orthopaedic Surgery.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
About Parkland Health
Parkland Health is one of the largest public hospital systems in the country. Premier services at the state-of-the-art Parkland Memorial Hospital include the Level I Rees-Jones Trauma Center, the only burn center in North Texas verified by the American Burn Association for adult and pediatric patients, and a Level III Neonatal Intensive Care Unit. The system also includes two on-campus outpatient clinics – the Ron J. Anderson, MD Clinic and the Moody Outpatient Center, as well as more than 30 community-based clinics and numerous outreach and education programs. By cultivating its diversity, inclusion, and health equity efforts, Parkland enriches the health and wellness of the communities it serves. For more information, visit parklandhealth.org.
