Radiofrequency ablation offers a nonsurgical treatment for thyroid nodules

DALLAS – May 23, 2022 – When Vickie Bell-Percival was offered the opportunity to have a nodule on her thyroid treated with a new nonsurgical technique called radiofrequency ablation (RFA), she didn’t hesitate.
“The options were surgery or RFA. My concerns were how invasive the treatment would be and how much time it would take to heal. I also wanted it done quickly. My doctor said she could schedule the ablation for Friday and – boom shakalaka! – it was done,” said Mrs. Bell-Percival.
Earlier this year, Mrs. Bell-Percival became the first patient at UT Southwestern to undergo RFA for her thyroid nodule. Although being the first made her experience special, Mrs. Bell-Percival, 68, a busy IT worker and matriarch of a large family, is typical of patients who will opt for this treatment over surgery.
At her May checkup, the nodule had shrunk 60% since the procedure eight weeks earlier.
Thyroid nodules – lumps that occur in the butterfly-shaped gland at the base of the neck – are so common that nearly half the population will develop one by age 60. They are more common in women than men and more likely to occur as people age.
Most thyroid nodules are noncancerous, but even benign nodules can cause health problems, including persistent coughing, difficulty breathing, difficulty swallowing, and hoarseness. Large nodules can be disfiguring as well.

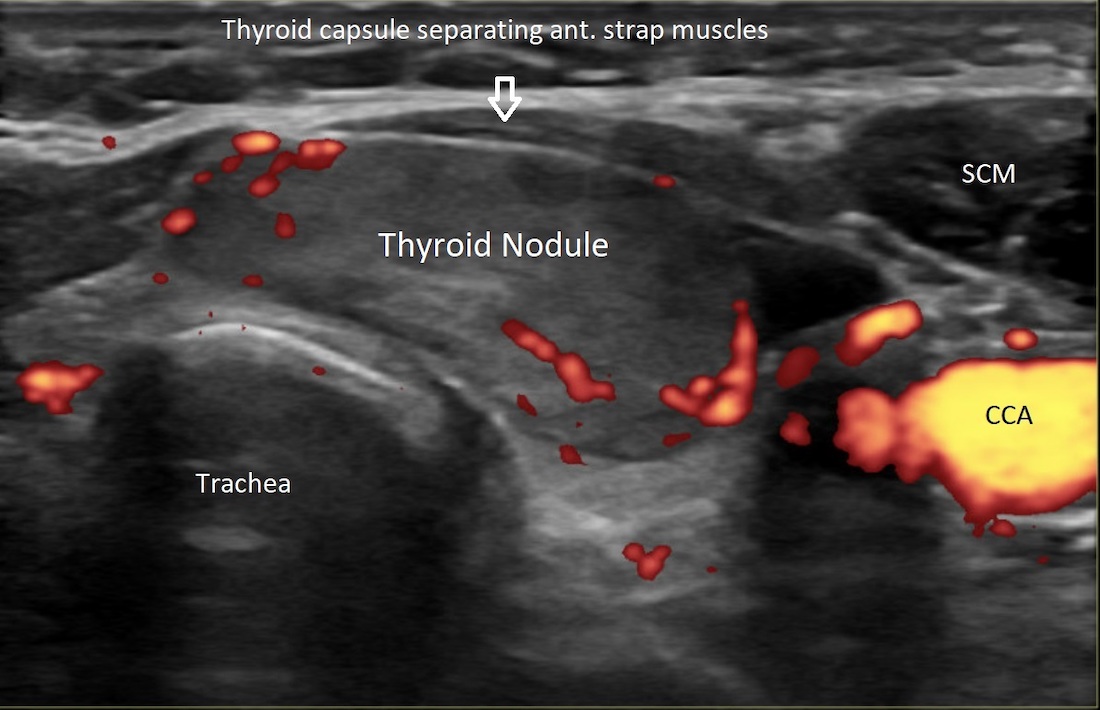
RFA uses an electrode with high-frequency current to generate heat to burn the tissue, leading to cell death and shrinking of the treated part over time, explained endocrinologist Iram Hussain, M.D., Assistant Professor of Internal Medicine at UT Southwestern, who was Mrs. Bell-Percival’s treating physician. Dr. Hussain is a member of the Harold C. Simmons Comprehensive Cancer Center who specializes in treating thyroid nodules.
“We use ultrasound-guidance with a parallel approach throughout the procedure so we can see the entire needle in real time, reducing the risk of complications,” Dr. Hussain said. “RFA has several advantages over surgery. The patient won’t need general anesthesia, won’t have an incision or scarring, won’t need thyroid medicine, and will be able to resume their normal routines in a shorter time. Generally speaking, any patient with a benign solid nodule who is a candidate for surgery could consider RFA.”
RFA has long been used to treat liver tumors, varicose veins, and other conditions. Since it received FDA approval in 2018, a handful of medical centers, including UT Southwestern, have begun using the technique to treat benign thyroid nodules as well. UT Southwestern is ranked among the top 25 hospitals in the nation for diabetes and endocrinology care by U.S. News & World Report.
Mrs. Bell-Percival’s nodule, which was without symptoms at first, was discovered by another UT Southwestern physician, G. Sunny Sharma, M.D., Assistant Professor of Physical Medicine and Rehabilitation, who was treating Mrs. Bell-Percival for back and neck pain. “Dr. Sharma did some X-rays and discovered the nodule. I’m so grateful to him for finding the nodule and for then referring me to Dr. Hussain. I love the way UT Southwestern doctors work together,” said Mrs. Bell-Percival.
Dr. Hussain immediately did a fine needle aspiration biopsy and was able to reassure Mrs. Bell-Percival that the nodule was not cancerous. Since she had no symptoms, no treatment was needed at the time.
But the nodule continued to grow, and six months later Mrs. Bell-Percival was having a bit of trouble with swallowing. By March, she was ready for something to be done, and that’s when Dr. Hussain told her about RFA.
On the day of the procedure, Mrs. Bell-Percival said everything went smoothly.
“They prepped me and used a local anesthetic to deaden the area, but Dr. Hussain wanted me to be awake during the procedure and asked me to speak occasionally so she could be sure there was no damage being done to my vocal cords. She inserted the heated needle and moved it around a bit. I could feel a little vibration, but they’d prepped me on what would happen, so I knew exactly what to expect.
“There wasn’t any pain associated with it, just a little discomfort very briefly. The whole thing took less than 30 minutes. Easy-breezy,” recalled Mrs. Bell-Percival.
“I am grateful to Mrs. Bell-Percival for entrusting me with her care,” said Dr. Hussain.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
