Flexible assemblies of nerve cells key to episodic memory
UTSW study shows phenomenon in human patients for the first time
DALLAS – Dec. 12, 2022 – For the first time, scientists have recorded human nerve cells firing together in flexible assemblies, a process that appears necessary to successfully encode long-term memories, a study led by UT Southwestern researchers reports. The findings, published in Nature Communications, could lead to new ways to slow, prevent, or even improve memory loss caused by Alzheimer’s disease and other types of dementia.

“These assemblies are important because we think this is a fundamental unit of how the brain works, especially for creating new memories,” said Bradley Lega, M.D., Associate Professor of Neurological Surgery, Neurology, and Psychiatry at UTSW, and in the Peter O’Donnell Jr. Brain Institute.
Previous research in rodents has shown that when these animals form memories of a specific event or episode, groups of nerve cells, or neurons, in the brain fire together within a narrow time window of around 25 milliseconds (.025 seconds). This time window is set by key brain waves involved in memory, termed gamma oscillations.
By firing so close together in time, the brain waves can organize the timing of when assembly neurons fire and promote connections between them. Although these assemblies have been well established in lab models, they had never been seen in humans, and it was unknown if this same basic mechanism applied to human brain activity.
To search for their existence, Dr. Lega, his frequent UTSW collaborator Brad Pfeiffer, Ph.D., an Assistant Professor of Neuroscience and a Southwestern Medical Foundation Scholar in Biomedical Research, and a colleague at Columbia University worked with patients at UTSW’s Epilepsy Monitoring Unit, where epilepsy patients stay for several days before undergoing surgery to remove the damaged parts of their brains that spark seizures. Electrodes implanted in their brains not only help surgeons precisely identify the seizure foci, Dr. Lega said, but also provide valuable information on the brain’s inner workings.
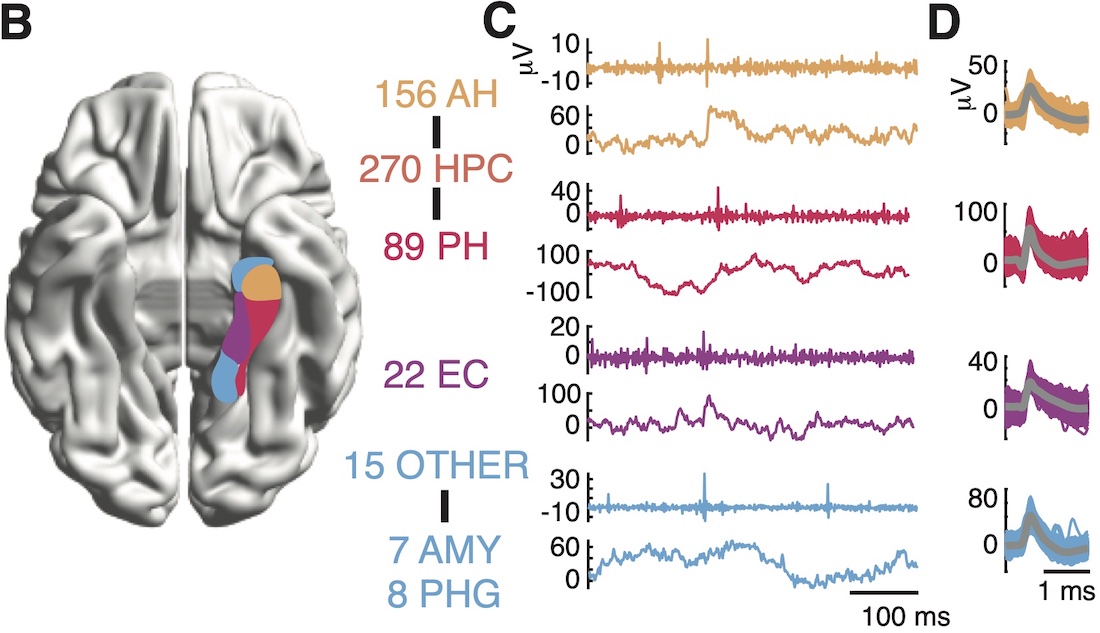
The researchers recorded activity from electrodes placed in the mesial temporal lobes (MTLs), an area key to forming memories. While the researchers recorded activity at single-neuron resolution, the patients performed memory tasks in which they tried to memorize lists of several words, then recall as many as they could.
Analysis of these recordings revealed these brains exhibited the same phenomenon as in rodents, with groups of neurons firing together on time scales of about every 25 milliseconds. Rather than being nearest neighbors, these neurons were often scattered across the patients’ MTLs.
However, Drs. Lega and Pfeiffer and their colleagues noticed a key difference compared to the findings in rodents. Rather than these assemblies being permanently fixed, they were typically flexible, with neural members joining and dropping out over 20 to 30 minutes. In fact, Dr. Lega said, the more flexible a patient’s assemblies behaved, the better he or she performed on the memory task.
“These neural assemblies act more like a group of musicians who jam together for a couple of gigs and then go off and join other bands,” Dr. Lega explained. “Gamma oscillations act like the conductor, organizing when individual neurons play their notes.”
Because this flexibility appears to be key to successful episodic memory, he added, it could be a useful biomarker for interventions in development by Dr. Lega’s lab and others that aim to help people with memory loss.
Gray Umbach, M.D., a former UTSW medical student who is now a neurosurgical resident at the University of California, San Francisco, was lead author on the study. UTSW researcher Ryan Tan also contributed.
This research was funded by grants from the National Institutes of Health (R01NS107357, R01NS125250, and R01MH104606) and the Southwestern Medical Foundation.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
