Plant-rich diet protects mice against foodborne infection, UTSW researchers find
DALLAS – Dec. 25, 2019 – Mice fed a plant-rich diet are less susceptible to gastrointestinal (GI) infection from a pathogen such as the one currently under investigation for a widespread E. coli outbreak tied to romaine lettuce, UT Southwestern researchers report. A strain of E. coli known as EHEC, which causes debilitating and potentially deadly inflammation in the colon with symptoms such as bloody diarrhea and vomiting, is implicated in several foodborne outbreaks worldwide each year.
“There has been a lot of hearsay about whether a plant-based diet is better for intestinal health than a typical Western diet, which is higher in oils and protein but relatively low in fruits and vegetables,” says Vanessa Sperandio, Ph.D., professor of microbiology and biochemistry at UT Southwestern. “So we decided to test it.”
Her study on a mouse model of EHEC is published this week in Nature Microbiology.
“Plant-rich diets are high in pectin, a gel-like substance found in many fruits and vegetables. Pectin is digested by the gut microbiota into galacturonic acid, which we find can inhibit the virulence of EHEC,” she adds.
“This is relevant to public health because EHEC outbreaks lead to hemorrhagic colitis, which is debilitating and sometimes causes death, particularly in the very young and the elderly,” she says.
Intestinal pathogens like EHEC sense the complex chemistry inside the GI tract to compete with the gut’s resident microbiota to establish a foothold, Sperandio says. Over centuries, the pathogens have developed different strategies to compete against the so-called good, or commensal, microbes that normally line the gut.
Those commensals include harmless strains of E. coli living in the colons of humans and other mammals, where they help the host’s normal digestion process, she adds. The word commensal means “eating at the same table” and that is what the symbiotic bacteria that make up the gut’s microbiota do.
The commensals that line the gut present a significant barrier to intestinal pathogens, Sperandio explains. EHEC and similar gram-negative bugs overcome that barrier by deploying a secretion system called T3SS.
T3SSs act like molecular syringes to inject a mix of virulence proteins into the cells lining the host’s colon, setting off inflammation and symptoms of infection. Because mice are unaffected by EHEC, researchers use a similar pathogen, Citrobacter rodentium, in mouse studies, Sperandio explains.
“Our study finds first that the good E. coli and the pathogenic ones like EHEC use different sugars as nutrients,” she says, adding that the two types of E. coli may have evolved to avoid competing for the same energy sources. “Second, we find that dietary pectin protects against the pathway the pathogenic EHEC uses to become more virulent.”
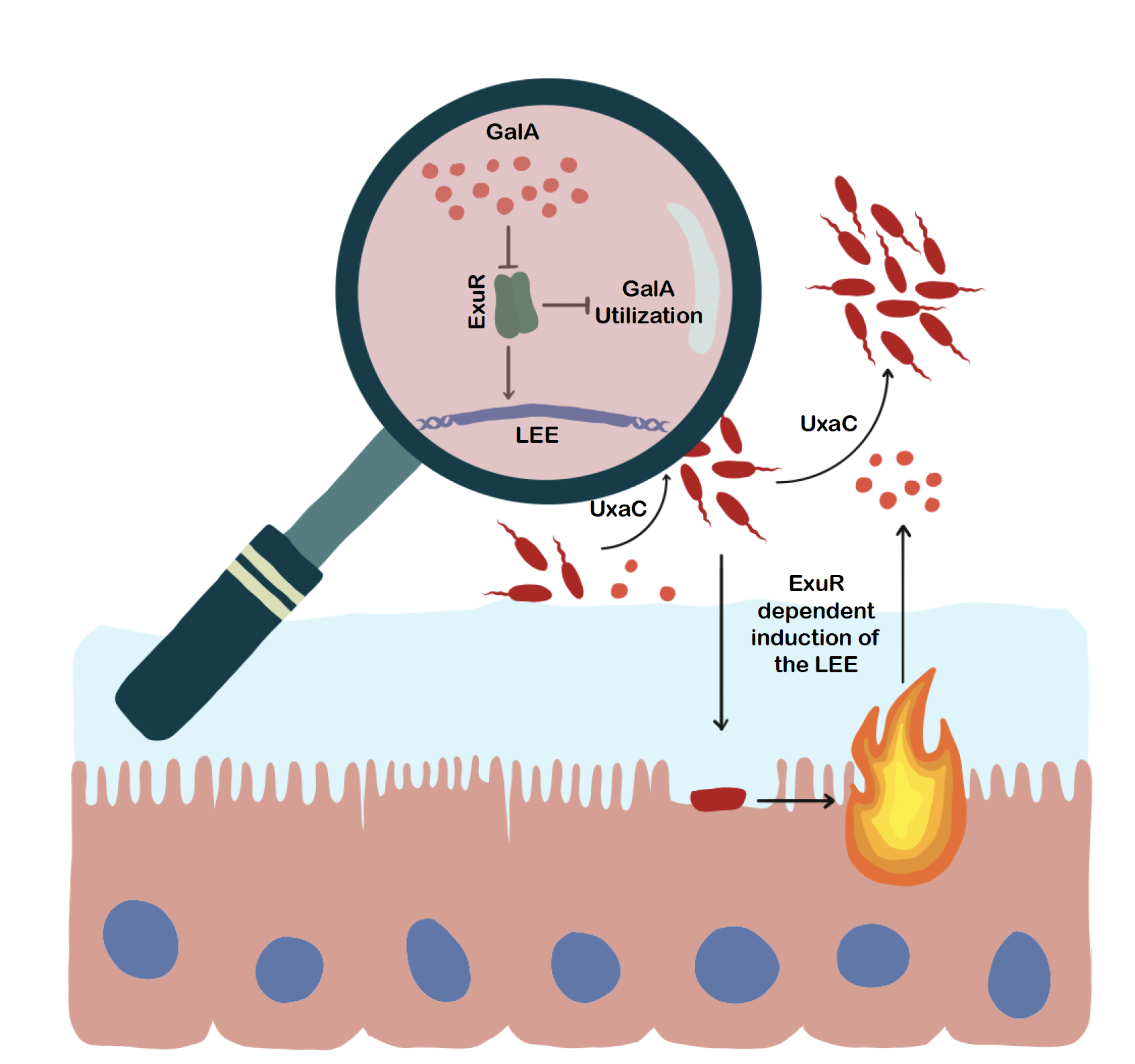
Another type of commensal gut bacteria breaks down dietary pectin from fruit and vegetables, creating galacturonic acid, a sugar acid that the EHEC and C. rodentium use in two ways. Initially, the pathogen uses that sugar acid as an energy source to expand in the gut, Sperandio says.
“Once the sugar acid becomes depleted, the pathogen changes its survival strategy, almost like flipping a switch,” she says. Instead of using the galacturonic acid for nourishment, the infectious bacteria employs it in a signaling pathway that increases the EHEC’s and similar bacteria’s virulence using the syringe-like T3SS.
In the study, mice fed pectin for about a week withstood infection. Comparing the colons of six mice fed a chow diet with 5 percent extra pectin from citrus peel with four mice on a typical diet, the researchers found a much lower rate of infection in the pectin-eating mice, Sperandio says.
The amount of bacteria in the mouse gut was measured by daily stool checks and by analysis of the amount of bacteria in a pouch at the juncture of the small and large intestines, called the cecum, at the experiment’s end.
The researchers found that mice on the pectin-enriched chow had about 10,000 bacteria in the cecum compared to 1 million bacteria in mice on the typical diet. The pectin group also had fewer symptoms, she says, adding that a pectin level of 5 percent appears to prevent the pathogen from activating its virulence repertoire.
She stresses that the research is one step in a journey to define the molecular mechanisms that govern how the commensal species in the gut impact the virulence of intestinal pathogens.

“This is not translatable to humans yet. We hope a better understanding of how intestinal disease develops will lead to strategies to reduce the incidence or, at least, the symptoms caused by these gram-negative pathogens, possibly through new vaccines or drugs,” she says.
Additional study authors are lead author Angel Jimenez López and Melissa Ellerman, both of UT Southwestern, and Wade Abbott, of the Lethbridge Research and Development Centre, Agriculture and Agri-Food Canada.
The authors report no competing interests.
The study received funding from the National Institutes of Health (grants AI053067, AI05135, AI077613, AI114511, and training grant 5 T32 AI7520).
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty has received six Nobel Prizes, and includes 22 members of the National Academy of Sciences, 17 members of the National Academy of Medicine, and 15 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 2,500 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in about 80 specialties to more than 105,000 hospitalized patients, nearly 370,000 emergency room cases, and oversee approximately 3 million outpatient visits a year.
