UTSW findings could lead to more effective CPR delivery
Improvements to ventilation technique outside of hospital setting can enhance patient survival rates
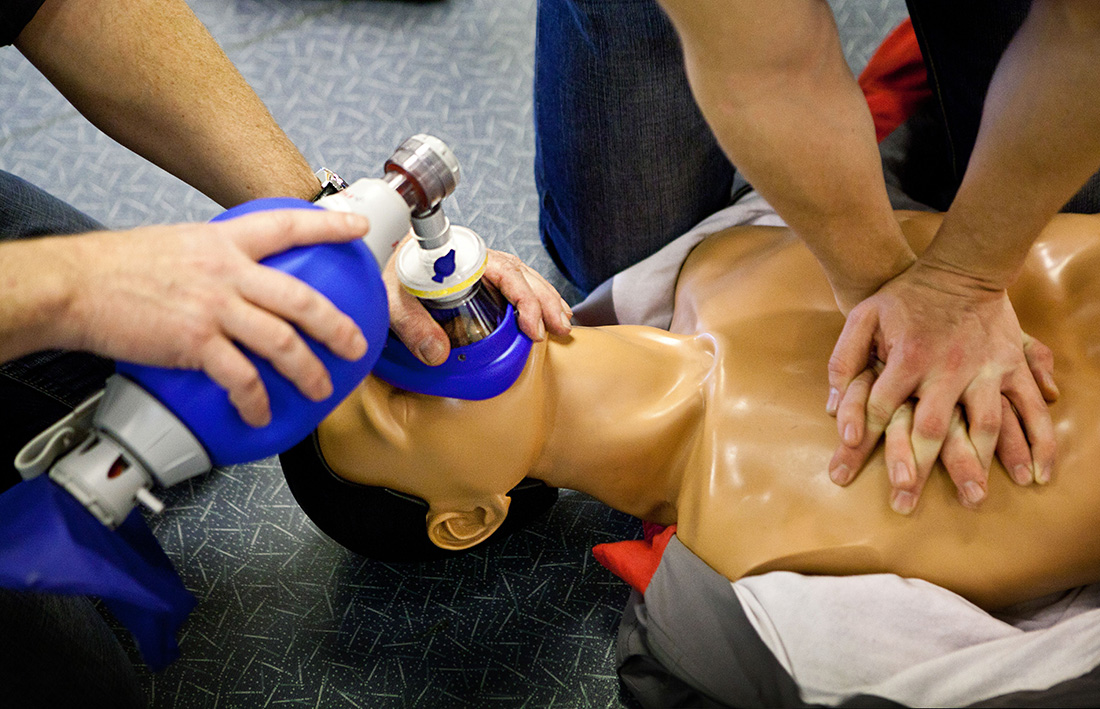
DALLAS – Nov. 13, 2023 – Simple changes in patient ventilation procedures during out-of-hospital cardiopulmonary resuscitation (CPR) could lead to a dramatic improvement in cardiac arrest survival rates, according to a landmark study led by UT Southwestern Medical Center.
The findings, published in Circulation and presented at the American Heart Association’s annual Scientific Sessions conference in Philadelphia, show that bag-valve-mask (BVM) ventilation – a common CPR technique used with chest compressions to ensure patients are getting oxygen – is often performed inconsistently.
When BVM ventilation was effectively delivered, with cardiac arrest patients receiving measurable ventilation in at least half of the pauses during chest compression, the survival rate was up to four times greater compared with those who received ventilation in less than half of the pauses. The discovery could reshape the way CPR is administered in the field, the authors said.

“The role of chest compressions during CPR has been studied at length for more than two decades, but there has been little on ventilation until our research,” said study leader Ahamed Idris, M.D., Professor of Emergency Medicine and Internal Medicine and Director of Emergency Medicine Research at UT Southwestern. “The assumption was that ventilation with the bag and mask took place whenever the ventilation bag was squeezed. But our study found that in actual out-of-hospital conditions, BVM has significant shortcomings – primarily because it is difficult for emergency personnel to know whether proper lung inflation is occurring during early CPR.”
To better understand the limitations of out-of-hospital ventilation, Dr. Idris’ team developed a novel method of measuring ventilation using the thoracic bioimpedance channel that is recorded by many defibrillators during the early stages of CPR. The technique uses a computer program to identify lung inflation waveforms from those recordings, providing data on the effectiveness of BVM ventilation.
The team used that program to conduct a secondary analysis of clinical and continuous cardiac monitor data from six sites in the U.S. and Canada that participated in the Resuscitation Outcomes Consortium’s clinical trial studying the effectiveness of continuous compressions versus standard CPR. A total of 1,976 records were included in the study from patients who underwent 30:2 CPR (30 chest compressions for every two breaths via BVM ventilation) and had usable recordings.
The investigation showed that detectable ventilation occurred in only 40% of compression pauses overall, suggesting poor ventilation. In patients who had measurable ventilation in at least half of the pauses in 30:2 CPR, there was an associated improvement in return of spontaneous circulation, survival to hospital discharge, and survival with favorable neurological outcome.
Dr. Idris stressed that emergency personnel can improve the odds of success by measuring and monitoring BVM ventilation during CPR using capnography that is available in many defibrillators now in use; ensuring that an oropharyngeal airway device is placed before starting BVM ventilation; and reducing or preventing mask leak by holding the mask in place with both hands while another rescuer squeezes the bag. Using newly developed portable spirometers that can be coupled with defibrillators can be an effective tool for measuring ventilation.
“Adequate ventilation through BVM is a difficult skill to perform properly and must be practiced regularly to maintain proficiency,” Dr. Idris said. “Our hope is that this study spurs EMS medical directors to find solutions that work best for their agencies, ensuring that staff in the field is aware of the limitations of BVM and have been trained in how to overcome them.”
UTSW researchers have been working to measure ventilation during early CPR since 2015, often in collaboration with engineers at the University of the Basque Country, Spain. This study builds upon those earlier efforts and was supported by the National Institutes of Health and the National Heart, Lung, and Blood Institute.
Other UTSW researchers from Emergency Medicine who contributed to this study are Mary P. Chang, M.D., M.P.H., Associate Professor; Betty Y. Yang. M.D., M.S., Assistant Professor; and Sarah Shaver, M.D., Assistant Instructor.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty members have received six Nobel Prizes and include 24 members of the National Academy of Sciences, 25 members of the National Academy of Medicine, and 13 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 3,300 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians in more than 80 specialties care for more than 143,000 hospitalized patients, attend to more than 470,000 emergency room cases, and oversee nearly 5.3 million outpatient visits a year.
