Neurocritical Care
Leadership

Venkatesh Aiyagari, M.D.
Division Chief
Contact
Misti Marshall
Section Administrator
misti.marshall@utsouthwestern.edu
The Division of Neurocritical Care is the largest in North Texas and brings together faculty from diverse disciplines including neurology, anesthesia, internal medicine, and radiology. The division embodies the core missions of the Department of Neurology, including excellence in patient care, promoting education, and advancing our understanding of acute neurological care through research.
Our faculty have established a nationally and internationally recognized dataset, "Establishing Normative Data for Pupillometer Assessments in Neuroscience Intensive Care" (END-PANIC). The section is a site for the NIH-funded "Transforming Research and Clinical Knowledge in Traumatic Brain Injury (TRACK-TBI)," a precision medicine dataset, advancing the understanding and treatment of TBI. We are home to two Level I trauma centers and are recognized nationally as one of only four Neurointensive Care Units in the country with a Gold Beacon Award for Excellence awarded by the American Association of Critical-Care Nurses.
Faculty
The Neurocritical Care faculty comprises fourteen physicians and thirteen APPs who form a cohesive unit dedicated to advancing research, education, and clinical care. Our faculty have received extramural funding for research encompassing several targeted areas including stroke, traumatic brain injury, coma, and neuromonitoring.
The diverse background of our faculty allows us to provide subspecialty expertise in various disciplines such as neuroanesthesia, interventional neuroradiology, and pulmonary medicine in addition to clinical neurosciences. This expertise extends to not only clinical care but also to the education of residents and fellows from various training specialties.
View all faculty View APPs Join Our Team
Neurocritical Care Lecture Series (CME)
Neurocritical Care Highlights
3
Neurointensive Care Units
3
Comprehensive Stroke Centers
2
Level-1 Trauma Centers
2000+
Days of continuous EEG performed annually
1
Multinational Registry, "END-PANIC"
1
Neuroscience Nursing Research Center
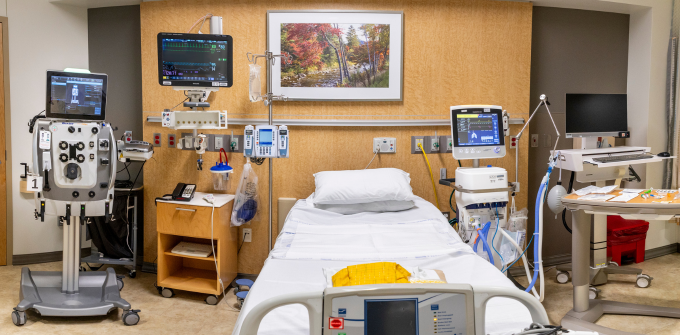
Intensive Care Units
We provide clinical services in three modern, well-equipped neurointensive care units across the Dallas Metroplex area. In addition, we also provide consultation services to patients in medical, surgical, cardiothoracic, cardiovascular, and burn ICUs at Parkland Health.
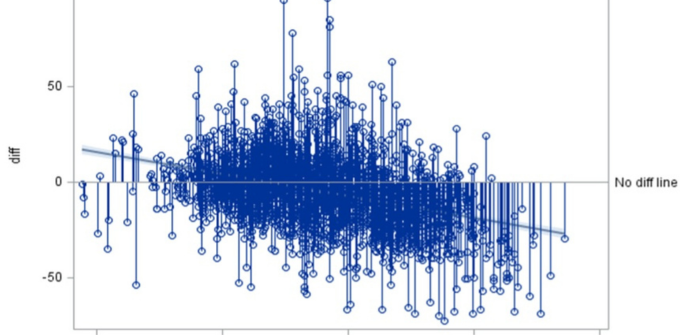
Research
Physicians and scientists within the Neurocritical Care Division center their discoveries on a range of clinical and basic science topics pertinent to the intensive care of patients with neurological and neurosurgical disorders. Clinical research activities span across clinical trials and neuromonitoring studies, including traumatic brain injury, ischemic and hemorrhagic stroke, coma, neuromuscular respiratory failure, and status epilepticus. We lead an international pupillometry research database that contains data on pupillary reactivity from multiple institutions across the U.S., Japan, and Germany. Our Division also hosts the Neuroscience Nursing Research Center whose mission is to promote active clinical research participation of nurses to improve outcomes for neuroscience patients.
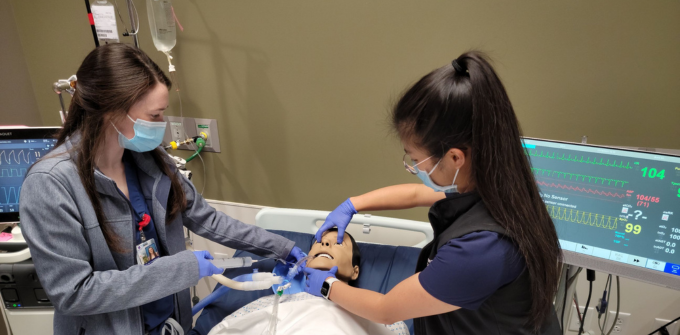
Education & Training
We train medical students and residents from a variety of specialties such as neurology, neurosurgery, anesthesia, emergency medicine, and physical medicine & rehabilitation. We also work with fellows from various disciplines including vascular neurology, and medical & surgical critical care. Our two-year neurocritical care fellowship offers trainees the opportunity to manage the full spectrum of acute neurological and neurosurgical critical care. The faculty foster nuanced critical thinking and reasoning skills, all of which are vital in the intensive care unit setting. We utilize the UTSW Simulation Center, one of the largest state-of-the-art simulation facilities in the nation, to provide fellows with a rich experience in various ICU procedures. This provides experiential learning in real-world scenarios to help them confidently navigate through neurological and critical care emergencies. The program aims to engage trainees in scholarly projects, develop an educational portfolio, and bolster individual career growth.

Stroke Education for Providers and Nurses
Physicians, Faculty, and APPs from several sections have created a self-study lecture series. Through these, participants learn about best practices in stroke care and earn CME Credits. These lecture series are open to everyone, both within and outside of UT Southwestern
Topics Include:
- Acute Stroke Care
- Cerebral Venous Sinus Thrombosis
- Cognitive Function & Communication
- Pain Management & Palliative Care
- Prehospital Care
- Social Determinants
- and more

Our Reach Within the Community
The Curing Coma Campaign® is an initiative launched by the Neurocritical Care Society® in 2019. It is the first global public health initiative to tackle the unifying concept of coma as a treatable medical entity. The campaign is organized into various scientific and administrative working groups tasked with addressing this challenge. Our division actively participates in this campaign, and Dr. DaiWai Olson is a co-chair of this campaign.

