Voice Behavior & Rehabilitation Lab Research: How Everyday Voice Use and Personality Shape Phonotrauma Risk and Recovery
Laura Toles, Ph.D., CCC-SLP
April 16, 2026
Voice injuries such as vocal fold nodules and polyps, often grouped under the term "phonotrauma," are among the most common voice problems seen in clinical settings. These conditions are generally thought to result from how a person uses their voice in daily life.
With support from a K23 award from the NIH's National Institute on Deafness and Other Communication Disorders, the Voice Behavior and Rehabilitation Lab, directed by Laura Toles, Ph.D., is conducting a longitudinal study to better understand how everyday voice use and individual personality characteristics contribute to both the development of phonotrauma and the ability to recover from it. The goal of this work is to support earlier identification of risk, more targeted prevention strategies, and more personalized approaches to voice therapy.
Our study will expand the limited amount of existing research that has followed people over time to understand why some individuals develop voice injuries while others with similar voice demands do not. Even less is known about why some patients find it harder than others to change harmful voice behaviors during treatment, which our research also will explore.
Previous studies have shown people with phonotrauma often speak more loudly, use their voices more throughout the day, and tend to have personality traits associated with being socially assertive or impulsive. Those same traits are associated with similar voice use patterns in people without current voice problems, suggesting that these traits may exist long before injury occurs. We hypothesized these personality traits and communication styles may increase vulnerability to voice injury and influence how patients respond to behavioral recommendations in therapy, but to date, no work has definitively found a causal link.
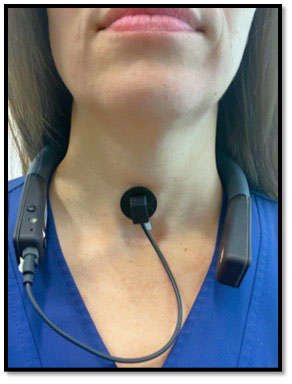
To explore this, our study follows vocally healthy college singers, a high-risk group, over several years, beginning in their freshman year. In addition to completing personality inventories, participants complete ambulatory voice monitoring at each time point by wearing a small sensor that adheres to the neck and measures the voice signal during everyday activities for four days, allowing us to capture real-world voice use outside of the clinic. Participants also undergo detailed imaging of the vocal folds using high-speed video endoscopy, an advanced technique that records vocal fold vibration in thousands of frames per second. By combining real-life voice use measures with high-speed imaging collected repeatedly over time, the study can observe subtle changes in vocal behavior and vocal fold function that may occur well before injury becomes clinically apparent.
In addition to understanding how phonotrauma develops, the study also examines the recovery process. A portion of the research focuses on how personality traits may affect a person's ability to follow voice therapy recommendations and make lasting changes to their voice use in daily life. This aspect of the project recognizes a common clinical experience: Not all patients respond to therapy in the same way, even when given similar guidance.
Findings from this work are expected to help clinicians better identify individuals at higher risk for phonotrauma, understand why some patients struggle with behavioral change, and tailor prevention and treatment approaches to the individual rather than relying on a one-size-fits-all model.
