Making Waves with HIFU
MRI-guided high-intensity focused ultrasound opens new paths to noninvasive treatment of brain disease
For years, brain surgery has involved anesthesia, scalpels, drills, and sometimes wires implanted into the brain. Today, some cutting-edge treatments involve no cutting at all.
One of the latest methods uses high-intensity focused ultrasound (HIFU) waves to penetrate the brain and remove unhealthy tissue. It’s similar to how children use a magnifying glass to focus the sun’s rays and burn a scrap of paper – only instead of sunlight, you’re using ultrasound.
Now technological advances are taking this treatment to the next level. Guided by MRI, physicians can precisely target specific parts of the brain, locating groups of cells and aiming the ultrasound waves with far greater precision. This noninvasive method can be used to treat tumors and other diseases typically treated with radiation or surgery. The combined technologies have an unwieldy acronym: MRgHIFU. It’s short for magnetic resonance-guided high-intensity focused ultrasound.

“MRgHIFU technology can potentially eliminate the need for invasive surgery,” said Dr. Bhavya R. Shah, Assistant Professor in the Division of Neuroradiology at the Peter O’Donnell Jr. Brain Institute, who is the pioneering researcher at the forefront of this innovative treatment. “High-intensity focused waves can be focused across the skull under real-time MRI guidance to ablate or burn away diseased tissue without the necessity of opening up the skull.”
Finding innovative ways to make a difference in people’s lives with technology is central to Dr. Shah’s work as Director of the Neuro Focused Ultrasound Program. As a child, he gained a love of working with devices from his father, an ophthalmologist who developed new ways to use laser technology for cataract surgery.

Dr. Shah uses MRgHIFU to treat patients with movement disorders such as essential tremor or Parkinson’s disease. The Food and Drug Administration has approved it as an effective tremor treatment for both.
“With today’s technology, a patient wears a helmet that focuses ultrasound beams onto a precise point in the brain,” he said. “There is no implantable hardware, no general anesthesia, and no incisions at all.”
The technology is also used to treat cancers. Prostate cancer was one of the earliest forms treated using MRgHIFU, but the technique might also be applied to breast or bone cancer.
“Pairing HIFU with our advanced imaging methods ensures you locate the appropriate targets in each patient and avoid damaging other structures,” Dr. Shah said.
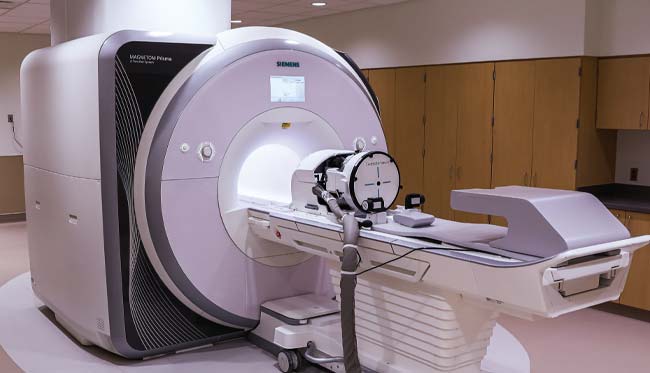
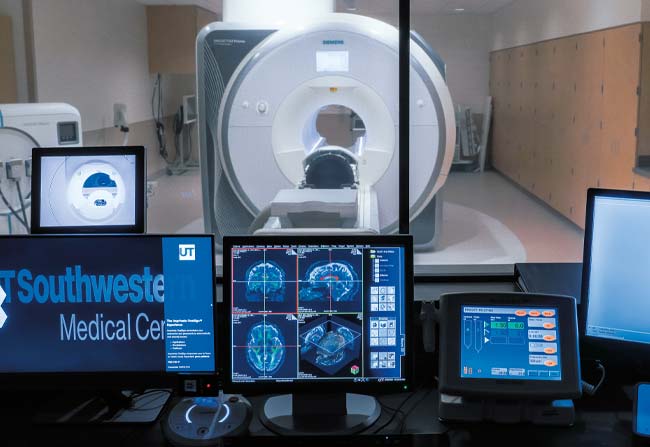
A first for Texas
The technology’s impact on the way physicians treat brain diseases could be seismic.
The National Institutes of Health estimates that essential tremor impacts as many as 10 million Americans. Parkinson’s disease affects a million more.
Fewer than two dozen hospitals in the U.S. offer treatment using MRgHIFU. Its steep price tag has limited widespread adoption.
UT Southwestern is the first hospital in Texas with the capability, thanks to an anonymous donor’s $5 million gift to the O’Donnell Brain Institute. The equipment is housed in the newly opened third tower of William P. Clements Jr. University Hospital, which has specialty care units for patients with brain diseases and is the clinical home of the O’Donnell Brain Institute.
The first patient procedure using the equipment took place in early March.
Jimmy Hiner, age 73, had suffered from debilitating involuntary tremors for decades before undergoing treatment at UT Southwestern. The retired long-haul truck driver and avid photographer first noticed the condition at age 17.

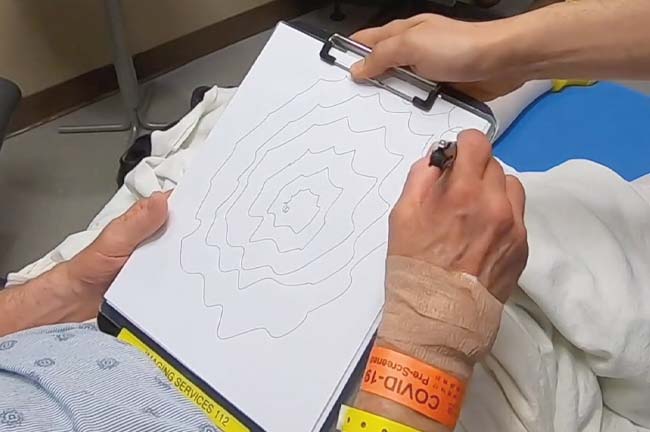
“Over the years, there were so many little things you just couldn’t do anymore because of the tremors. It got so bad I couldn’t write anymore. I couldn’t hold a camera steady to take a picture,” he said.
Dr. Shah treated Mr. Hiner using MRgHIFU. Immediately after, Mr. Hiner showed noticeable improvement. “Today, it’s slicker than a whistle,” he said. “The shaking is gone. It is just amazing the difference that it has made and how fast it happened. It’s just like they flipped the switch and it went away.”
The successful procedure marks a significant moment, even for an institution accustomed to being on the leading edge. Tremor and Parkinson’s patients from as far away as the Middle East and Europe have expressed interest in traveling to Dallas for the procedure.
“We are at the forefront of brain science because of the visionary generosity of our supporters, innovation of our scientists, and outstanding care provided by our clinicians,” said Dr. Daniel K. Podolsky, President of UT Southwestern. “This gift enables us to bring a technology with great promise to Texas and surrounding states, expanding our capacity to pursue groundbreaking research and opening up new treatment possibilities for patients in Texas and beyond.”
An extensive team of UT Southwestern leaders collaborated across brain research, radiology, and neuroradiology to bring this project to fruition. The Neuro Focused Ultrasound Program works with physicians in Neurology, who initially evaluate patients. Since the new procedure is not appropriate for everyone, Dr. Shah consults with colleagues in Neurology and Neurosurgery to decide on the best candidates. MRgHIFU is one of several types of next-generation “neuromodulation” therapies being advanced in the O’Donnell Brain Institute.
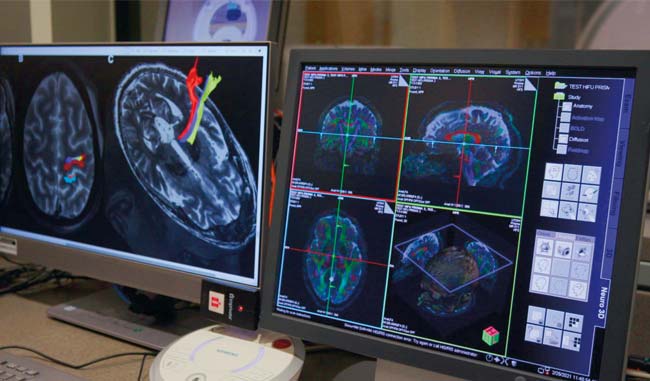

Bypassing the blood-brain barrier
In addition to removing tissue, Dr. Shah is currently leading clinical trials at UT Southwestern to determine whether MRI-guided focused ultrasound is effective for delivering drug therapies and diagnostic agents into the brain – past the blood-brain barrier.
Acting as part of the body’s defenses against toxins and diseases, the blood-brain barrier is a type of wall that separates the brain from the bloodstream. Essential nutrients delivered by the blood can pass through the barrier, but larger particles, such as bacteria or viruses, cannot.
The shield works so well it’s hard for physicians to deliver therapies to the brain.
Injecting drugs directly into the bloodstream is not effective for treating the brain because the blood-brain barrier stops them. Alternatively, when injected directly into the brain, drugs do not extend very far beyond the injection site. And as Dr. Shah pointed out, “Anytime you put a needle close to the brain there is always the chance of injury.”
Those risks aren’t a factor with MRI-guided focused ultrasound.
One of the best ways to penetrate the blood-brain barrier is to inject a series of small gas-filled bubbles into a vein. When they reach the brain, they can be targeted with focused ultrasound. Instead of using higher intensity waves that can destroy cells, this technique substantially reduces the intensity of the waves. When the ultrasound waves interact with the bubbles, the bubbles gently vibrate and push open the blood-brain barrier. Diagnostic agents and other therapies can be delivered through the opening, directly to the brain.
“What we’re now doing is turning the ultrasound wave energy level way down … to not destroy any tissue but rather to interact with microbubbles to open the blood-brain barrier,” he said. “This process can then deliver drugs or diagnostic agents to a specific target in the brain.”
Through his clinical trials, Dr. Shah sees potential to use focused ultrasound to deliver therapies to targeted parts of the brain in patients suffering from Alzheimer’s and brain tumors. He also anticipates using the technique to deliver immunotherapy and gene therapies in patients with neurodegenerative diseases, movement disorders, and genetic diseases. “The future of personalized medicine is in using MRI-guided focused ultrasound to deliver gene therapy, chemotherapy, and immunotherapy to specific regions of the brain instead of destroying brain tissue. These noninvasive procedures could be a game-changing, clinical breakthrough.”
Dr. Podolsky holds the Philip O’Bryan Montgomery, Jr., M.D. Distinguished Presidential Chair in Academic Administration, and the Doris and Bryan Wildenthal Distinguished Chair in Medical Science.

