Quality Improvement Distinction program teaches medical students how to advance patient care

As a primary care physician, second-year internal medicine resident Dr. Taylor Roberts became aware of a problem some of her patients encountered. Upon hospital discharge, they received multiple sets of medication lists with discrepancies.
Routinely, a patient’s chart contains several documents that detail their prescribed medications, including the discharge summary, clinician instructions, and a computer-generated medication list.
“These three major lists can be discrepant with each other – and that can lead to patients having misunderstandings about what medications they should take or a clinician misunderstanding what the patient took,” said Dr. Roberts.
This led Dr. Roberts and other residents to develop a quality improvement project on this issue for practices at William P. Clements Jr. University Hospital and Parkland Memorial Hospital. The solution: Simplify the medication information provided at discharge by deactivating older, outdated medication lists.
Dr. Roberts learned how to tackle patient care improvement projects as a medical student at UT Southwestern through the M.D. with Distinction in Quality Improvement and Patient Safety (MDD) program. It’s one of five Distinction tracks available for medical students to earn with their degree at UTSW.
“We’re all responsible for improving patient care,” Dr. Roberts said. “Broadly, the goal of quality improvement in medicine is to improve the way physicians deliver care to patients so that every patient receives the best care possible every time, and that we as medical providers are doing everything in our power to ensure patients are safe.”
In-depth training
The MDD in Quality Improvement and Patient Safety track provides medical students with 24 additional weeks of extensive quality improvement training. Besides improving care and clinic and hospital policies, another goal is to pique students’ interest in careers focused on quality improvement.
“Every school teaches medical students the basic methodologies of how to improve factors such as infection rates, patient satisfaction, or how to decrease care costs,” said Dr. Gary Reed, Associate Dean for Quality, Safety, and Outcomes Education. “UT Southwestern also teaches all of our medical students the basics of quality improvement, plus we wanted to provide interested students an in-depth QI experience with academic recognition.”
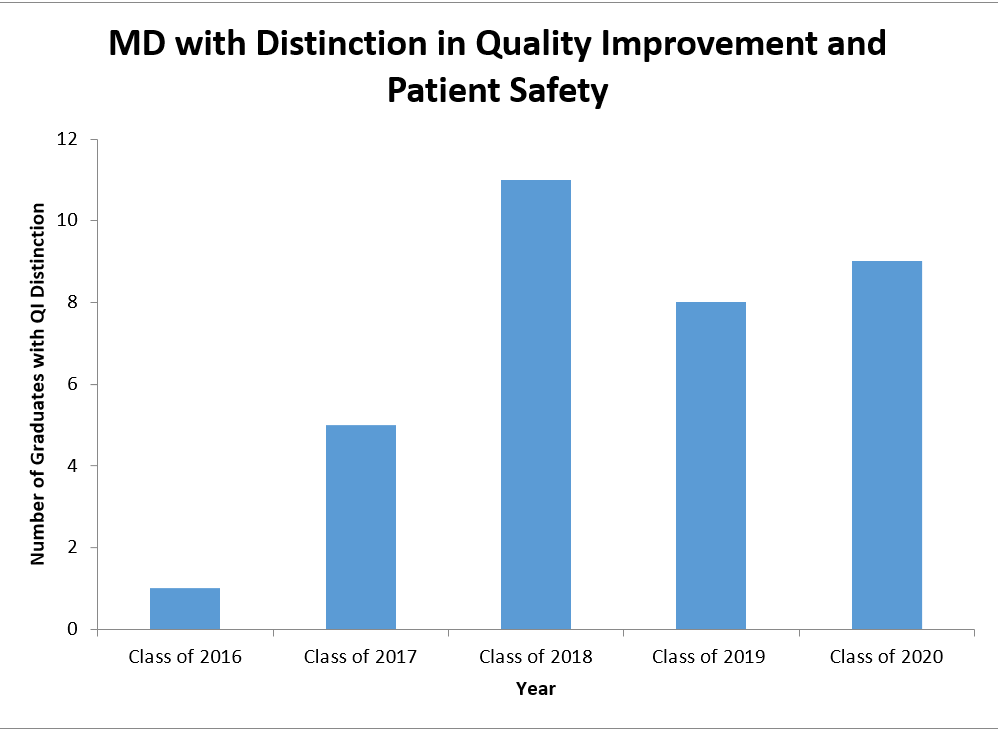
Since the start of the track in 2015, 34 UTSW medical students have graduated with this Distinction. An additional 20 students are in the pipeline to graduate with this Distinction in 2021 and 2022.
The curriculum includes a weeklong Quality Improvement boot camp centered on interdisciplinary training at which students work with nursing and industrial engineering students from UT Arlington. Students are assigned to groups of up to six and tasked with solving clinical quality problems in an interprofessional setting.
“Although doctors are frequently medical team leaders, physicians should learn to use the strengths of all the members of their team to solve medical problems because the collective knowledge of a team of a doctor, nurse, and engineer is stronger than a team of three doctors,” Dr. Reed said.
Additionally, students complete a seven-week summer program that pairs them with clinical faculty members working on QI projects.
Applying QI skills
As a student, Dr. Roberts worked under Dr. Jennifer Rabaglia, Associate Chief Medical Officer and Chief Quality and Safety Officer for Parkland, on a QI project to enhance recovery of elective colorectal surgery patients. The goal was to standardize evidence-based best practices in care before, during, and after the operation to decrease complication rates and hospitalization time.
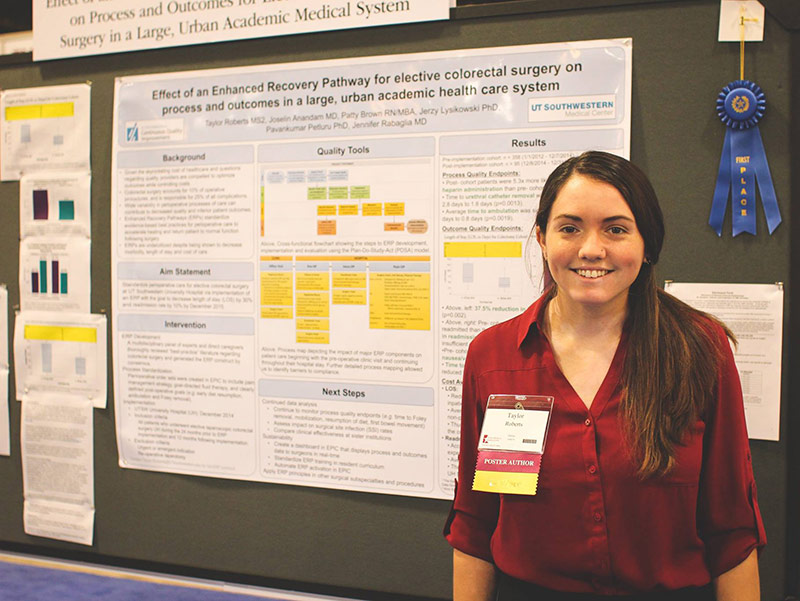
The project was presented at several conferences and Dr. Roberts’ first-author paper, “Enhanced Recovery Pathway Improves Colorectal Surgery Outcomes in Private and Safety-Net Settings,” was published in the Journal of Surgical Research in 2019.
“I think the QI track does an amazing job in teaching fundamental methodology skills that enable you to take a leadership role in whatever project you decide to work on,” Dr. Roberts said.
For her more recent project to address discrepancies in medication lists, Dr. Roberts and other residents reviewed hundreds of patient records.
The residents found that 21 percent of Parkland’s discharge summaries had discrepancies in them, as well as 12 percent of the discharge instructions. Similarly, at Clements University Hospital, the results revealed that 17 percent of discharge summaries and 8 percent of discharge instructions contained discrepancies.
“It’s actually a pretty prevalent problem,” Dr. Roberts said, adding that discrepancies in medication lists is a hospital issue not unique to Parkland or Clements.
Residents presented their findings to the committees that oversee electronic medical functions at the two hospitals. The solution was to deactivate Smartlinks, the electronic functions that autopopulate a list of medications into the discharge instructions. Residents discovered that these lists were not getting updated appropriately, in part leading to discrepancies between discharge documents.
Showing your work
Physicians in every specialty are required to participate in QI projects during residency as part of a requirement by the Accreditation Council for Graduate Medical Education, therefore the MDD track sets students up for success in many ways after medical school. Dr. Aishwarya Vishwanath, a 2020 Medical School graduate, earned the MDD Distinction in May. In July, she’ll begin her internal medicine residency at Rhode Island Hospital – Brown University.

As a student, she was assigned to a QI project called “Using Audit and Feedback to Reduce Avoidable Transfusions in Cardiovascular and Thoracic Surgery” under the direction of Dr. Philip Greilich, Professor of Anesthesiology and Pain Management. The project aimed to better inform physicians about the transfusion process and reduce the need for the procedure during cardiac surgery.
In March, she presented the project as her thesis. All Distinction-seeking students are required to write a 30-page thesis and give an oral presentation, publish at least one peer-reviewed abstract or article, and present their project at a regional or national conference.
“The skills I learned in medical school through this program definitely give me a leg up going forward in my career,” Dr. Vishwanath said. “That includes learning how to work with different medical specialties and multidisciplinary teams, such as nursing staff, data analysts, and information technology.”
Dr. Reed holds the S.T. Harris Family Distinguished Chair in Internal Medicine, in Honor of Gary Reed, M.D., and the Eva A. Rosenthal Professorship in Internal Medicine, in Honor of Gary Reed, M.D.


