UTSW team leads change to safer respiratory support strategy for preterm infants
Reduced use of mechanical ventilation in favor of less invasive CPAP approach decreases risks

A UT Southwestern team of neonatologists, nurses, and respiratory therapists is sharing its strategy for reducing the use of mechanical ventilation in preterm infants with health care professionals nationwide.
During a workshop at the Pediatric Academic Societies meeting in April, the team taught more than 60 health care professionals ways to optimize noninvasive respiratory support for newborns. The workshop gave participants a hands-on experience that they can take back to their medical centers, said Venkat Kakkilaya, M.D., Associate Professor of Pediatrics in the Division of Neonatal-Perinatal Medicine. The approach was detailed in 2019 and 2021 studies in Pediatrics that Dr. Kakkilaya authored.

“We hope that this strategy will be adopted across the country,” said Dr. Kakkilaya, also a neonatologist at Children’s Health. “Our reports showing improved outcomes after decreasing exposure to mechanical ventilation are now being noticed around the world. This is a moment of pride for our Division, UT Southwestern, and Parkland Memorial Hospital.”
UTSW was selected to present the workshop at the largest gathering of pediatricians worldwide. The UT Southwestern team collaborated with Cohen Children’s Medical Center in New York to provide participants with the tools needed to implement the strategy and stop using mechanical ventilation on newborns.
Premature babies who are born with immature lungs and are surfactant-deficient can develop respiratory distress syndrome, requiring mechanical ventilation and surfactant therapy. Mechanical ventilation involves attaching a breathing tube in the windpipe of a premature baby. Despite the lifesaving benefits of mechanical ventilation, premature infants are vulnerable to its harmful effects. Even brief exposure to mechanical ventilation, Dr. Kakkilaya said, can lead to bronchopulmonary dysplasia, a form of chronic lung disease.
With early use instead of continuous positive airway pressure, or CPAP, the risks from mechanical ventilation decrease, he said. Nationwide, 80% of premature infants receive mechanical ventilation during their neonatal intensive care unit (NICU) stay, Dr. Kakkilaya said.
“But we can reduce the need for mechanical ventilation at birth and in the NICU,” he said. “If other centers start following our strategy, it could have a huge impact across the country. Our 2019 study showed that effective face-mask breaths can help decrease the need for mechanical ventilation at birth and instead transition to CPAP, which is provided via nasal prongs.”
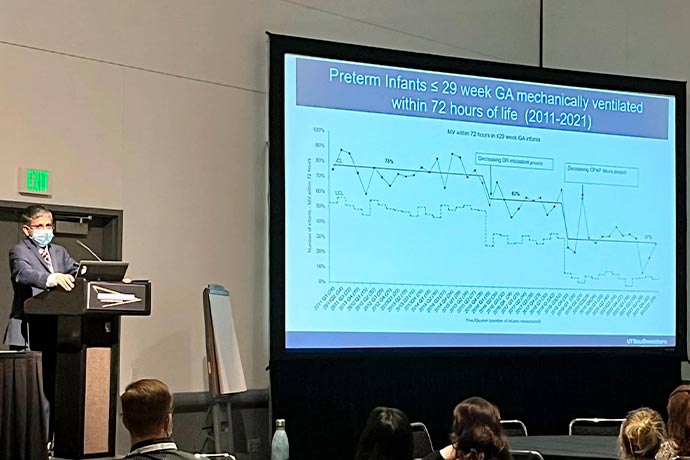
In 2015, respiratory support for nearly 60% of premature babies involved mechanical ventilation in the delivery room. “Since we implemented steps to improve a noninvasive respiratory support strategy in the delivery room, the need for mechanical ventilation dropped to less than 30%,” Dr. Kakkilaya said.
Surfactant therapy is a well-established lifesaving treatment for preterm infants with respiratory distress syndrome. Traditionally, surfactant was administered via the breathing tube in conjunction with mechanical ventilation. Over the last decade, use of a less invasive surfactant administration method (LISA) involving a thin catheter decreased the need for mechanical ventilation and improved outcomes of infants who were admitted to a NICU on CPAP.
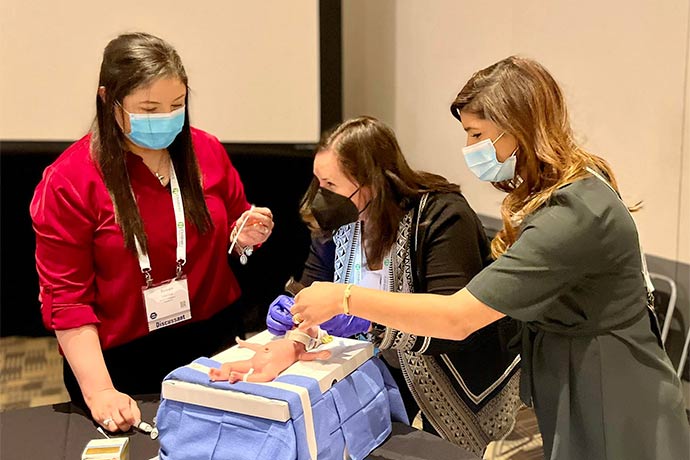
The LISA method is widely adopted in NICUs in Europe. A survey co-authored by Dr. Kakkilaya in the Journal of Perinatology showed that U.S. neonatologists are mainly using breathing tubes for surfactant administration. After conducting research reported also in the Journal of Perinatology and presenting the results to UTSW faculty, a multidisciplinary team including Dr. Kakkilaya developed the guidelines in 2018 for incorporating LISA with CPAP.
After adopting the change, the need for mechanical ventilation at Parkland dramatically decreased from 45% to 11%, Dr. Kakkilaya said.
UT Southwestern is the first major academic center in the U.S. to use the LISA/CPAP approach as its standard of care, he added.


