Endoscopic nasal polyp procedure provides lasting relief
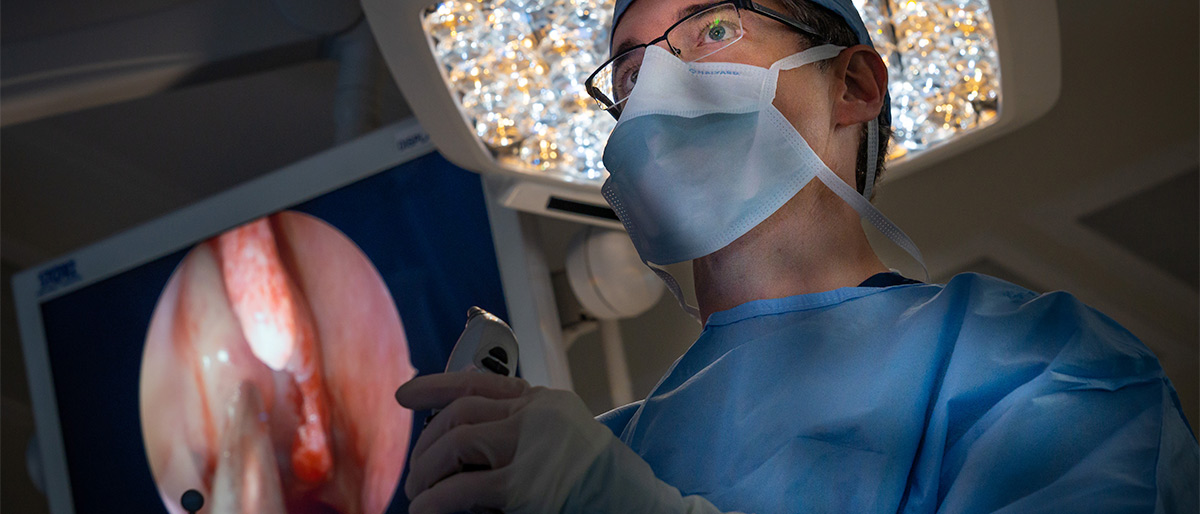
For those with nasal polyps, advances in technology promise to make breathing easier, including a minimally invasive procedure called functional endoscopic sinus surgery (FESS) performed at UT Southwestern that removes polyps and is more effective than other procedures such as balloon sinus dilatation.
For the 4% of adults who have nasal polyps, the surgery offers relief from congestion and nasal obstruction, may restore the sense of smell, and reduces snoring and other symptoms, said Matthew Ryan, M.D., Professor of Otolaryngology – Head and Neck Surgery, who with his colleagues performs more than 700 advanced sinus surgeries a year.

“Historically, sinus surgery has been an ordeal for patients,” Dr. Ryan said. “Outdated techniques such as minimal polyp removal and sinus stripping with placement of nasal packing after surgery produced only short-term results, if any, and often required weeks of painful recovery. Some techniques highly promoted in the media like balloon sinus dilatation accomplish almost nothing for the treatment of nasal polyps.”
By comparison, today’s advanced sinus surgery is vastly different. Real-time stereotactic computer-aided navigation permits safe, complete surgery. Patients are asleep under general anesthesia and the surgeon uses an endoscope – a thin tube with a camera – and specialized small tools inserted via the nostrils. There is no swelling, bruising, or other external sign that surgery has been performed.
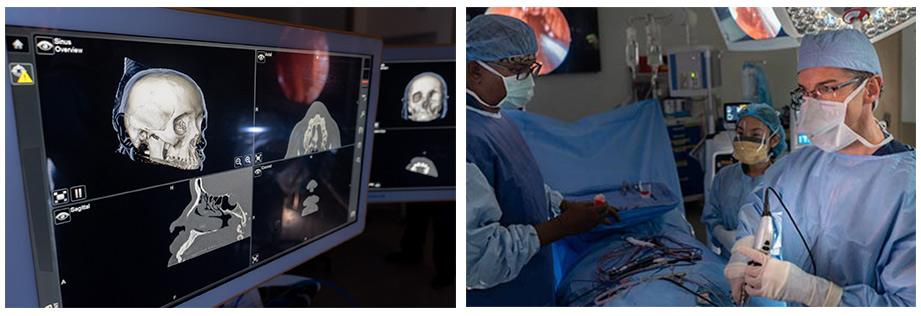
“We pair sophisticated computer guidance with our surgical expertise to navigate more precisely within the sinuses and remove polyps,” Dr. Ryan said. “The technology adds an additional layer of safety to the surgery, making patients and surgeons more confident in getting positive results.”
Patients usually go home the same day. Most do not feel much pain, he said, but might have some discomfort, congestion, or spotty nose bleeds for a few days.
Although nasal polyps can occur in anyone, about 25% of patients with chronic rhinosinusitis develop them, Dr. Ryan said. Small nasal polyps might not cause any symptoms, but if they grow large enough that they block the nasal passages, they can make breathing difficult and take away the sense of smell, he added.
“Polyps are the result of chronic inflammation, though we don’t yet understand what triggers their development in some people and not others,” Dr. Ryan said. “Certain conditions such as allergies, cystic fibrosis, aspirin sensitivity, and frequent sinus infection have been shown to increase the risk of developing nasal polyps. But in most instances, there is no single treatment that constitutes a ‘cure’ for the disease.”
While polyps can be removed, there is a chance they can return. For patients suffering now, surgery can make a significant difference, he said.
“They can breathe easier and sleep better, which means they can get back to enjoying their lives – and we are honored to be a part of making happen,” Dr. Ryan said.


