Neurological Surgery Chair envisions building on UTSW’s clinical, research strengths to advance treatment

The opportunity to draw upon UT Southwestern’s dual strengths in outstanding clinical care and translational research to develop new treatment options attracted Dr. Nader Pouratian, a neurosurgeon known for innovative surgical care for depression, blindness, and movement disorders, to the role of Chair of Neurological Surgery. UT Southwestern is ranked No. 17 in the nation by U.S. News & World Report in neurology and neurosurgery.
Additionally, the powerful potential of the Medical Center’s Peter O’Donnell Jr. Brain Institute and the chance help build the young brain research and treatment center caught his attention.
Dr. Pouratian, who joined UTSW April 1, holds an M.D. and a Ph.D. in neuroscience and was previously a Vice Chair at UCLA’s David Geffen School of Medicine. He succeeds Dr. Hunt Batjer, who retired in December after serving as Chair of Neurological Surgery since 2012, and Dr. Carlos Bagley, Associate Professor of Neurological Surgery and Orthopaedic Surgery, who served as Interim Chair.
At UCLA, Dr. Pouratian was Professor and Vice Chair of Academic Affairs in the Department of Neurosurgery, with additional appointments and affiliations in Neuroscience, Bioengineering, and Radiation Oncology.
In his clinical practice, Dr. Pouratian focuses on surgical treatments for movement disorders, psychiatric disease, facial pain, and chronic pain syndromes, using modern techniques such as brain and spinal cord stimulation, radiosurgery, microsurgery, and targeted ablation. He is also a clinical researcher and prolific author of peer-reviewed scientific publications and a passionate educator and mentor.
Dr. Pouratian is currently involved in clinical trials testing surgically implanted stimulators in the brain to remedy blindness and treatment-resistant depression. He said he hopes to use advances in technology to develop new procedures to treat stroke, brain injuries, and neurological and psychiatric diseases.
Dr. Pouratian received his undergraduate degree in neuroscience from UCLA, then earned a combined medical degree and Ph.D. from the David Geffen School of Medicine, followed by a neurosurgical residency and functional neurosurgery fellowship at the University of Virginia.
“Dr. Pouratian’s expertise will allow him to work closely with researchers and clinicians to improve treatment options for brain diseases and injuries and to discover ways to prevent such illnesses,” said Dr. W. P. Andrew Lee, Executive Vice President for Academic Affairs, Provost, and Dean of UT Southwestern Medical School. “This strategic cooperation between the Department of Neurological Surgery and the O’Donnell Brain Institute will further elevate UT Southwestern as a national hub for excellence in neuroscience discovery and clinical care.”
Indeed, the potential for such synergies is one of the reasons Dr. Pouratian listed for his decision to join UT Southwestern. In an interview during his first month here, he shared his vision for the Department.
Why did you decide to join UT Southwestern?
Most of all it was the vision of UT Southwestern and its leadership to continue to transform and evolve as a leader in academic medicine.
The primary reason I decided to become an academic neurosurgeon was, first and foremost, the opportunity to take care of patients with diseases of the brain. But I was almost equally intrigued by the unique opportunity neurosurgery provides to study and learn about how the brain works. To do this kind of human neuroscientific discovery takes a collaborative environment with clinician-scientists like myself and translational neuroscientists who want to work together and maximize the opportunity.
At the O’Donnell Brain Institute, under Director Dr. William Dauer, human neuroscience is a high priority and a major area of investment. Building bridges between basic sciences and human neuroscience is a big part of the vision, which was attractive to me.
What are some areas of special interest for you?
Personally, my passion has been at the intersection of neurological care, engineering, and technology, with a focus on developing new therapies – including for patients whom we have not traditionally cared for with neurosurgical therapies, like patients with psychiatric disease or patients with blindness.
I am currently involved in a clinical trial treating a small number of patients with complete blindness using a specially designed device that is implanted in the patient’s brain. Together with a California company that I also consult for, Second Sight Medical Products Inc., we received National Institutes of Health funding to develop and test the device. Our preliminary investigations have revealed positive results, allowing people with complete blindness to see patterns of flashing lights that they are learning to interpret and decode. This trial began when I was at UCLA and I am hoping to continue this clinical research soon at UT Southwestern as well.
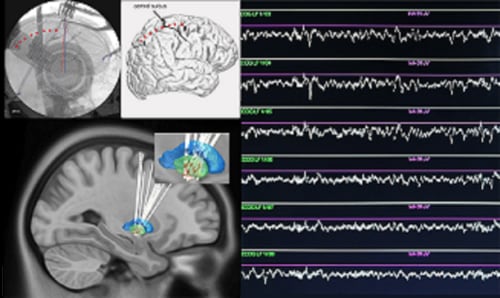
Another area of particular interest is the treatment of patients with treatment-resistant major depression. Just like other diseases that we treat with brain stimulation – like Parkinson’s disease – depression affects the brain and results in abnormal brain activity. We have a fairly good but incomplete understanding of the parts of the brain and the networks in the brain that are involved in depression. Our approach is to put stimulators in these precise areas of the brain, using advanced neurosurgical techniques with cutting edge imaging. By stimulating those areas of the brain that are critically related to depression, we aim to make those brain networks function more normally and help people with depression. We are looking forward to launching two separate clinical trials here in this area in collaboration with our outstanding colleagues in psychiatry.
What areas do you want to focus on as the new Chair?
UT Southwestern Neurosurgery is known for its innovation. I hope to continue to promote and build on that spirit of innovation. One of the newest and most innovative technologies we have at UT Southwestern as part of the O’Donnell Brain Institute is focused ultrasound. This technology uses precisely targeted ultrasonic energy to treat or destroy tissue inside the body without the need to make an incision. The FDA has approved this technology for treating essential tremor and tremor-dominant Parkinson’s disease.
Beyond treating movement disorders, we are excited to collaborate with our partners in radiology to explore even more innovative applications. For example, we are looking forward to launching a novel study to open the blood-brain barrier to better deliver targeted therapies to the brain, treating epilepsy as well as potentially treating tumors and chronic pain. This is a just one example of helping to invent the future of our field, in collaboration with our outstanding clinical and scientific partners at UTSW.
Dr. Dauer holds the Lois C.A. and Darwin E. Smith Distinguished Chair in Neurological Mobility Research.
Dr. Lee holds the Atticus James Gill, M.D. Chair in Medical Science.
Dr. Pouratian holds the Lois C.A. and Darwin E. Smith Distinguished Chair in Neurological Surgery.


