How the pandemic changed life for four first-year residents
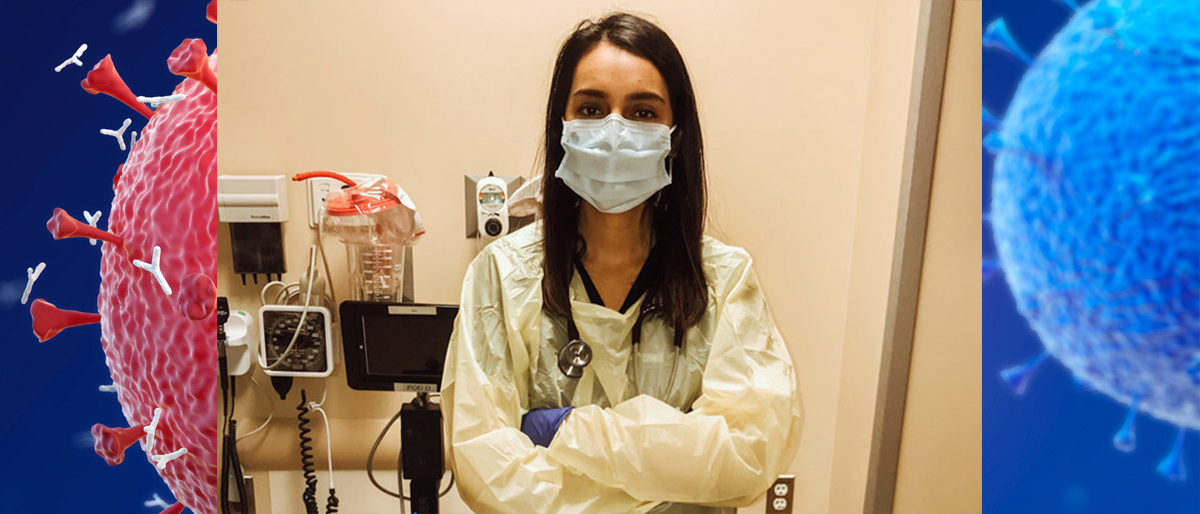
Drs. Iqra Zakaria, Jonathan Brewer, Danielle Rucker, and Deven Bhatia were more than halfway through their first year of residency at UT Southwestern when the COVID-19 pandemic added a heightened sense of urgency to their on-the-job training.
Like other health care workers, the emergency medicine doctors would quickly adjust to a new environment: learning how to correctly handle personal protective equipment (PPE), discovering new ways to care for patients while minimizing the risk of exposure, and juggling caring for themselves and their families while serving on the front lines of the health emergency.

As part of the Emergency Medicine program, the residents rotate through different ICU areas such as Pediatrics, Surgery, Burn Unit, and Toxicology as well as among three hospitals: William P. Clements Jr. University Hospital, Children’s Medical Center Dallas, and Parkland Memorial Hospital.
They all knew residency would be a time of long hours and stressful experiences, but none expected a global pandemic to strike in their first year as doctors. Recently, they shared a window into their hectic lives and how the experience has strengthened their resolve to help patients.
“This is why we are doing this. We want to be the people who others come to for help in any situation,” said Dr. Bhatia.
Shift changes
Before the pandemic broke out, Dr. Rucker made it a practice to make a personal connection with her patients. She would enter a hospital room and pull a chair up to the bed so she could get to know each patient face to face.
Now, most check-ins are made from the door. Patients are wearing masks too, obscuring part of their expressions. Safety comes first. COVID-19 has changed the nature of doctor-patient relationships.
“As more data comes out, we’re learning that some restrictions may be in place for a year or more. It’s a tough pill to swallow,” said Dr. Rucker, without irony.
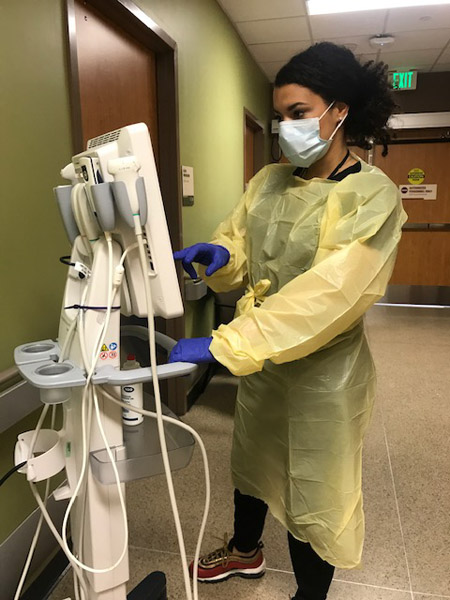
Some common routines are now different. When Dr. Zakaria arrives at Parkland each day, she goes to a specific entrance for a temperature check before entering the building. She no longer takes food, a backpack, or anything else with her to work, out of concern that she could inadvertently carry the virus back to her Uptown apartment. She doesn’t eat during her shift out of safety concerns, and she keeps her mask on at all times. “I have to remind myself to drink water during my shift,” she said.
After reporting to her station to gown up, Dr. Zakaria reviews the patient situation with departing night staff. The landscape changes during the shift, with new patients arriving and others leaving.
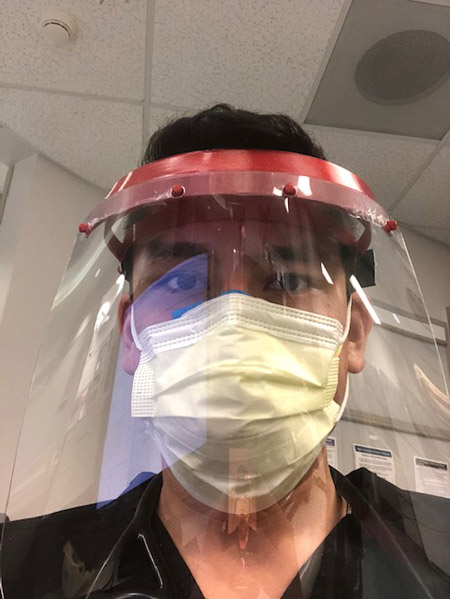
The emergency department residents have become familiar with “donning and doffing,” the process of putting on and taking off PPE: bouffant, N-95 mask, surgical mask, face shield, gown, and gloves. The gown and gloves are changed between visits to different patient rooms. The goal is to not infect anyone, at the hospital or outside. Multiple times each day, they sanitize their stethoscopes and hard surfaces where they work.
Even as the pandemic unfolded, other health care emergencies still occurred. Dr. Bhatia recently worked in the Burn Unit.
“Burn patients are very susceptible to infections because they’ve lost their protective skin barrier,” he pointed out. He notes that people are sometimes at higher risk for burns now that they are cooking more at home and completing more home projects.
‘A different energy’
The stations in Parkland’s emergency department, called pods, are for both COVID and non-COVID patients. There may be up to a dozen patients under the care of one person at times. Most residents keep moving during the entire 12-hour shift. While that’s not unusual, they’ve noticed that the energy in their department has changed.

“There’s a different vibe in the hospital now,” said Dr. Zakaria. “There’s a baseline anxiety and uncertainty bubbling under the surface at all times, like an unnerving current.”
The residents – and all the medical staff – rely on each other for support. They have seen the best and the worst of human behavior. “You can feel every single emotion on one shift,” said Dr. Brewer. “You get that one victory and it carries you through the whole day.”
What is a victory? When a COVID-19 patient is removed from a ventilator or someone has recovered from the virus and leaves the hospital. Each one is celebrated.
After cleaning up equipment and surfaces, conferring with the personnel taking over their shift, and doffing PPE, the residents walk through the hospital to the parking garage with their masks on.
Following each shift, Dr. Rucker still faces the one-hour drive home to Fort Worth, where she knows her 5-year-old son, Maddox, will already be asleep. Worried that she could potentially bring the infection home with her, she admitted, “I’m not completely confident that it couldn’t happen. We take every possible precaution, but there is always a fear.”
Dr. Brewer will de-stress after a shift by playing some guitar, having dinner with his fiancée, and chatting on FaceTime with his parents. “I told my parents when this started that I would no longer be able to see them as much as I would like to,” he said.
What they’ve learned
As the weeks turn into months in this pandemic, it can be hard to stay focused and positive, especially if residents face a combination of stressors at work and at home. UT Southwestern offers a variety of resources to help residents and other learners in this challenging time.
“At UT Southwestern, we have worked closely with our on-campus Wellness Center to provide assistance to residents who need emotional support; with the Office of Institutional Equity & Access to offer education; and to provide child care options for residents and fellows,” explained Dr. Larissa Velez, Associate Dean for Graduate Medical Education, Professor and Vice Chair for Education in the Department of Emergency Medicine, and a Distinguished Teaching Professor. “It has also been wonderful to see how the community at large has contributed to our well-being.”
As the residents prepared to enter their second year as doctors in July, they took a few minutes to reflect on lessons learned and what they want to share with the incoming class of residents.
“It’s an honor and a privilege every day that you come to work,” said Dr. Rucker. “In order to add value to your profession, you have to be well. Find ways to de-stress. Make sure you’re well protected from infection.”
Dr. Zakaria advised the next class of residents to take full advantage of the group support that is available. “These are unprecedented times with much uncertainty, but know that we are all here for you. Don’t be afraid to rely on your colleagues, the upper levels, and the faculty. Trust all the education that has gotten you to this point.”
They all expressed gratitude that their class bonded earlier in the year, and that first-, second-, and third-year medical residents interact a great deal in UT Southwestern’s program. They call their group a “work family” and check in on each other during shifts.
“Burnout is a very real issue in medicine,” said Dr. Brewer. “Medicine as a whole is experiencing a newfound resiliency. Everyone is staying strong and it’s very humbling to watch.”
Dr. Bhatia added a heartfelt thanks to paramedics and firefighters, nurses, ED technicians, radiology technicians, housekeeping crews, grocery store workers, and other essential workers who are also putting themselves at risk during the pandemic. He also expressed a broader word of encouragement that may help everyone:
“Everything else can shut down, but the ED will always remain open,” he said. “We will be here for you.”
Dr. Velez holds the Michael P. Wainscott, M.D. Professorship in Emergency Medicine.


