Surviving COVID-19: Beating the virus is just the beginning

What was one of your last pre-pandemic moments?
For 36-year-old Adrian Lynn-Royerth, it was a Saturday night at an indoor concert surrounded by friends and plenty of strangers. At that time, only gatherings of 500 people or more were prohibited in Dallas County. The venue implemented occupancy limits to further put space between people as an extra precaution. He said it felt safe.
Four days later, on March 18, Mr. Lynn-Royerth began experiencing some of the common symptoms associated with COVID-19 – coughing, fever, and nausea. Others within his network, including those who attended the concert, also exhibited symptoms such as loss of taste and smell. Their illnesses remained mild while Mr. Lynn-Royerth’s condition worsened with each passing day. His first ER visit to William P. Clements Jr. University Hospital resulted in a viral pneumonia diagnosis, a coronavirus-related complication. And on the morning of March 21, he received a call that he had tested positive for COVID-19.
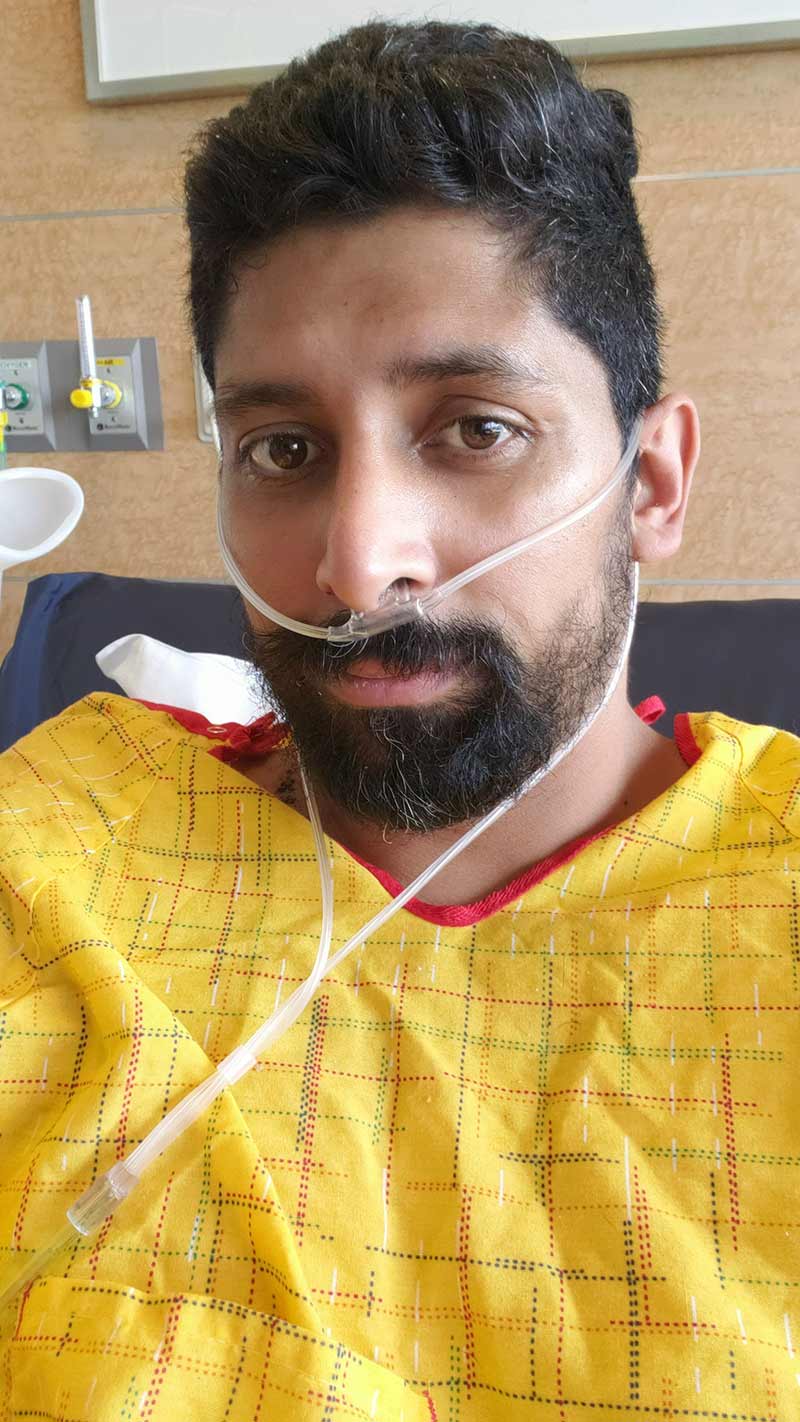
He soon developed shortness of breath and was rushed back to Clements University Hospital. “I felt different that morning and my chest was a little bit tighter,” Mr. Lynn-Royerth said. “My fever spiked to 103 degrees and all of a sudden I had a hard time just catching my breath.” In the two weeks following the concert, his health had rapidly deteriorated. Within a few hours of arriving at Clements, he was calling family members and close friends in tears before being intubated by medical staff.
Mr. Lynn-Royerth has hazy memories of the intubation but knew he was in good hands. “UT Southwestern has great facilities and you can see that the doctors and nurses genuinely care,” he said.
Inside the walls of the ICU, UT Southwestern’s health care heroes are delivering compassionate care while donning head-to-toe personal protective equipment. When Mr. Lynn-Royerth had energy, staff members helped him check messages on his phone to communicate with loved ones, including family members in Colombia.
“One of the main nurses that took care of me was so invested and she really stood by my side,” he added. “I wouldn’t be here without the help of all of the people that participated in my care.”
The unpredictability of COVID-19
The coronavirus manifests differently from person to person. Symptoms can vary drastically, depending on factors such as age or existing comorbidities. For some young, otherwise healthy individuals, the fierce attack on their body feels more random.
“You don’t know how it will affect you,” Mr. Lynn-Royerth said. “Other members of your own family could contract COVID-19 and not need to be hospitalized, but you may be the one who is hit hardest.” For those patients hospitalized with severe cases, health problems may linger long after they recover from the disease.
Dr. Corey Kershaw, a pulmonologist and Medical Director of the Medical Intensive Care Unit at Clements, and Dr. Kristina Goff, an anesthesiologist with specialty training in critical care who serves as Co-Medical Director of the Clements Surgical ICU, have teamed up to oversee management of a separate team and ICU for COVID-19 patients. “We predominantly see patients who are over the age of 50 in the COVID unit, but we certainly have had patients in their 20s and 30s,” said Dr. Goff, also Assistant Professor of Anesthesiology and Pain Management. “I think part of that is because Clements has such a large population of subspecialty patients like transplant patients and other patients with immunosuppression.”
Not only did Mr. Lynn-Royerth become infected at a time when experts had less understanding about the novel coronavirus, he did not check the boxes for one considered at high risk. Dr. Kershaw said age was not the most surprising factor in his case – it was that he had been in generally good health beforehand.
The road to recovery
Those who survive a long period on a ventilator are prone to muscle atrophy, weakness, and a host of residual health issues, said Dr. Kershaw, also Associate Professor of Internal Medicine. Mr. Lynn-Royerth, no exception, still carries the burden of medical complications more than half a year later.
After spending two weeks on a ventilator at Clements with his survival uncertain, Mr. Lynn-Royerth’s health turned a corner. When he woke up after his extubation on April 7, he did not recognize his body. He had lost more than 25 pounds in a short period of time and became winded just trying to stand up. “It was a shock seeing my body so ravaged,” he said. “It was a struggle and there is definitely a mental disconnect for a 36-year-old, who just a few months ago was running and jumping around on a volleyball court, when that physical ability just disappears. You feel a little bit helpless and you feel a lot of frustration.”

In addition to physical limitations, Mr. Lynn-Royerth has dealt with a racing heartbeat, nerve damage in his left foot, hair loss, reduced lung capacity, pulmonary scarring, sleep problems, blood clots, memory and recall issues, and more.
Dr. Kershaw said a lengthy recovery time after a prolonged, severe lung injury is to be expected, and in some cases damage is permanent. “I worry there is a misconception about survivorship,” he said. “People should realize that the COVID-19 survival rate does not reflect the complexities of recovery. A significant proportion of people could have leftover disability from the virus; the battle is not always over once you overcome the illness.”

Returning home was an emotion-filled day for Mr. Lynn-Royerth. He was reunited with his partner, Jeff Updike, his two Wire Fox Terriers, and his Jack Russell Chihuahua mix on April 14. “This overwhelming feeling washed over me,” he said, “I hit this milestone and thought things are going to be OK.”
By mid-August, Mr. Lynn-Royerth showed signs of progress. He could go on walks and bike rides around his neighborhood, which helped him increase lung capacity and improve exercise tolerance. But he does have to be mindful of air quality, because stepping outside when pollen is high or when the Saharan dust storm moved through Dallas-Fort Worth in July could have caused him to experience breathing difficulties. Blood clots are no longer an issue, but other things like his nerve injury could take up to a year to recuperate, with no promise of full functionality returning to his foot. In July, it was confirmed that he had lung scarring, which will require long-term monitoring. He takes his recovery one day at a time, grateful to still be alive.
Rising to the challenge
Early data from New York gave many the sense that the coronavirus would be a death sentence for those who ended up on a ventilator, but as seen at UT Southwestern, having proper resources and staffing available can be a game changer.

The pandemic has brought people together in new ways – and collaboration is thriving among caregivers dedicated to fighting the virus. “The collaboration between the anesthesia and the pulmonary critical care groups has been integral to our success,” Dr. Goff said. “This blended team has utilized the strengths of each group and allowed us to really be innovative in the way that we care for these patients.”
The coronavirus has presented health care workers with one of the greatest intellectual and psychological challenges of their careers. As the nation continues to grapple with the spread of the virus, experts hammer down on the importance of maintaining appropriate physical distancing and wearing masks to ensure the health care system never reaches a breaking point.
In September, UTSW President Dr. Daniel K. Podolsky told employees that what the future brings will depend on the degree to which we collectively continue to maintain vigilance in adhering to nonpharmacologic interventions. By October, COVID-19 cases and hospitalizations were on the rise again as variables such as expanded return-to-school policies for students overlapping with the start of the flu season swung the pendulum back.
“We’re staying fully prepared for this to be around indefinitely,” Dr. Kershaw said. “Our hope is that it remains a slow burn and we don’t have these big surges of cases. We all want to return to a sense of normalcy, but that all goes back to the community.”
Dr. Podolsky holds the Philip O’Bryan Montgomery, Jr., M.D. Distinguished Presidential Chair in Academic Administration, and the Doris and Bryan Wildenthal Distinguished Chair in Medical Science.


