The Bronze Star combat medic who became a UTSW Professor of Emergency Medicine

Throughout the month of November, which is designated as Veterans Month, Center Times Plus will feature content that showcases our faculty, staff, students, and patients who have served, or are still active, in the United States Armed Forces. Please keep visiting CT Plus for new content throughout the month.
A combat medic in the spring of 1969, Ahamed Idris was clinging to the chopper as it headed into a monsoon over the jungles of Vietnam. He was desperately trying to keep alive an Army crew chief whose arm had almost been severed after a tail rotor clipped his shoulder.
As rain slammed through the open doors of the stripped-down “Huey” gunship on its way to the nearest field hospital, Spc. Idris kept the nearly amputated arm packed with dressing to control bleeding, while he administered the IVs that delivered a steady flow of life-giving fluid.
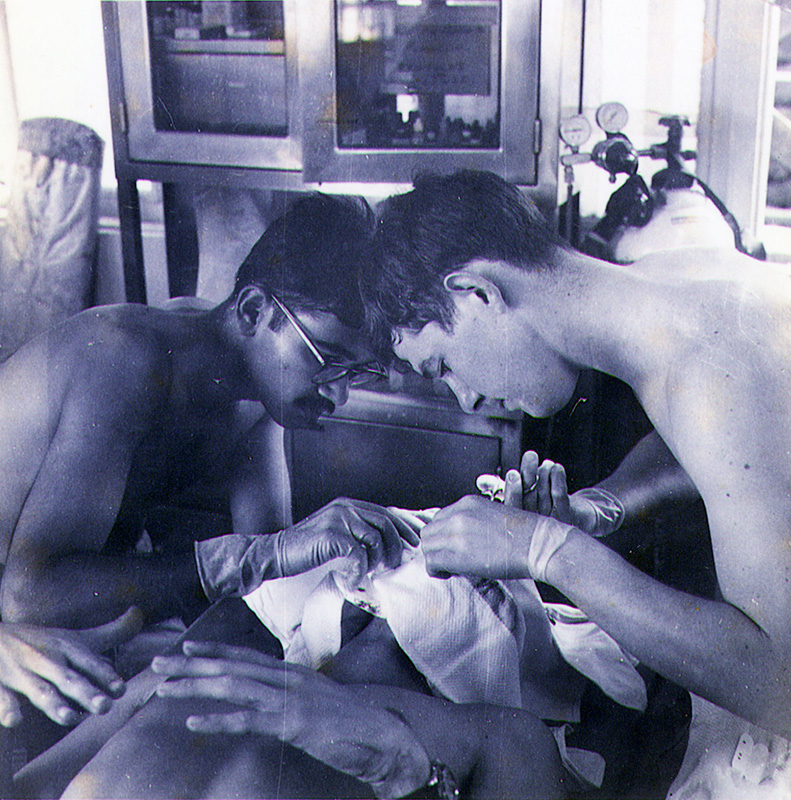
“The next 60 minutes are going to last an eternity,” the future UT Southwestern Professor of Emergency Medicine thought. “That’s if any of us live through this.”
As with many such missions then – and even now with some cases as Director of Emergency Medicine Research at UTSW – the combat medic never knew of the final fate of his patient, though he was told the crew chief survived his wounds.
But his year of heroic action in Vietnam earned Dr. Idris the Bronze Star for meritorious service in a combat zone.
“We used to joke that the red cross painted on the bottom of each medevac copter wasn’t a designation, it served as a target,” Dr. Idris said with a slight grin. “The mortality rate of medics in 1969 actually exceeded the mortality rate of infantrymen in the field. The enemy knew that if they took out a medic, they were taking out the other soldiers you were going to help.”
He had joined the storied 1st Air Cavalry Division, which had been carrying out operations throughout the Mekong Delta since 1965. The famed unit is unique in its designation over the years as a Cavalry Division, an Infantry Division, an Air Assault Division, and most recently as an Armored Division. During the Vietnam era, the division’s new quick-insertion tactics via waves of choppers began with the battle of Ia Drang – described in Lt. Gen. Harold G. “Hal” Moore Jr.’s book We Were Soldiers Once ... And Young and the basis of the 2002 movie We Were Soldiers starring Mel Gibson.
His daily routine was to run the airfield dispensary, but that schedule was often supplanted with de facto duties as a crew member on medevac missions bringing in wounded soldiers from the field. At times, duty required the 5-foot-7, 125-pound medic to hop out of the choppers under the yellow smoke that signaled the enemy was still active in the immediate area.

On that particular stormy night, all flights had been grounded, so Spc. Idris wasn’t sure how the crew chief walked into that tail rotor on the flight line.
“He was really bad off when I got there. I got him stabilized, but didn’t think there was much hope,” he recalled. “The call went out for ‘two crazy pilots’ to volunteer to fly the patient and me to the hospital. They were warming up the ship and the door machine guns had been yanked by the time we got there with the loaded stretcher.”
The hourlong flight from the Vinh Long Airfield to the surgical hospital at Can Tho, however, quickly became a survival exercise. The Mekong Delta’s terrain provided no discernable landmarks at night, and the rain was so heavy that the windshield wipers were useless. At times, there seemed to be as much rain inside the Huey as was beating on the copter from the outside.
“It wasn’t even instrument flying,” Dr. Idris recalled. “The pilots left on the right heading and tried to hold or correct course as best they could.”
Disorientation proved nearly fatal as the medevac flight neared its end: The crew initially mistook the lights of a hangar as being those of a landing pad.
“We didn’t realize the mistake until the last second,” he remembered. “The pilot opened his window, put his head out to see better, and pulled back hard to avoid collision, standing the Huey almost straight up in the air before recovering and landing on our next pass.”
Spc. Idris never discussed the experience with the two aviators courageous enough to take to the air that night.
“The storm subsided somewhat and we flew back, totally drained. When we landed, they just sat in their seats with their heads bowed. They had their helmets on and visors down the whole time. I could have passed by them the next day and couldn’t have identified them. They did their jobs to the best of their abilities, and I did mine. It was that simple.
“The thing I hated most were the mortar attacks. All you could do was grab the dirt and wait as the noise and concussive explosions got closer or trailed away from where you took shelter. It’s like being in a submarine under depth charge attack; there’s nowhere to go.
“In general, though, I never felt too anxious until I got under 30 days,” he said. “That’s when many get ‘short-timer syndrome’ and begin to realize you actually might make it back home to the world.”
‘Back home to the world’
Home for the young Ahamed was New York. He had a year of physics and math studies under his belt at Brooklyn College when an educational hiccup – taking less than a full load of classes while working full time – made him eligible for the draft. He selected the Army and enlisted in 1967.
“I scored high in testing, was given my choice of options, and I went with the Signal Corps once I completed Officer Candidate School,” recalled Dr. Idris. “But after six months of preparation, an officer marched in and said several schools were being shut down, including Signal OCS. The new military priorities identified were infantry, armor, artillery, Special Forces, and the Medical Corps.”
He chose the Medical Corps, his high scores put him at the head of the class, and he was offered an additional year of advanced medical training at Brooke Army Medical Center, after which he was promoted to Specialist 6 (a noncommissioned rank equivalent to Staff Sergeant).
“It basically was the equivalent of a physician assistant today, but we all knew where we were eventually going – we graduated and immediately received orders to Vietnam,” he recalled. “The most sobering experience was meeting with an Army attorney to fill out my will before leaving for Vietnam.”
Once discharged, the driven young man completed his degree at Northwestern University, supplementing his GI Bill funds with side work as a medic in the Cook County Jail. After four years of military experience and three years of providing medical service to inmates, the son of two immigrants – his father from India and his mother from Austria – enrolled in Rush Medical College, a private school on the west side of Chicago.
‘Going into medicine wasn’t hypothetical’
“Going into medicine wasn’t a hypothetical to me,” Dr. Idris said. “I had real-world experience that could be frustrating at times in school. For instance, medical students weren’t allowed to suture in clinical rotations; that was for the interns to do. We served as human retractors, and this was when I already had seven years of suturing, putting in chest tubes, intubating patients.”
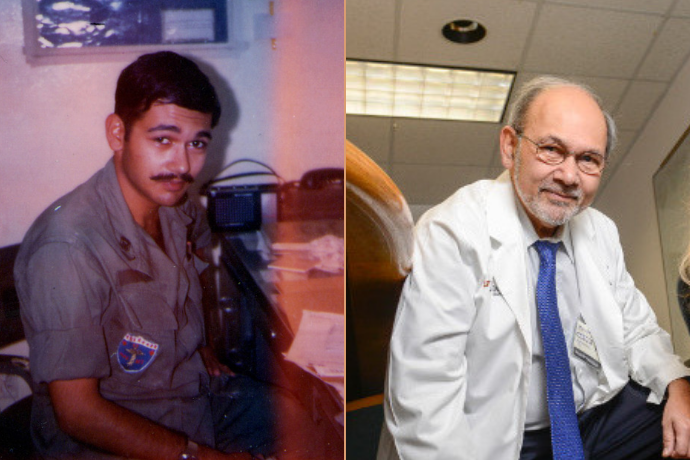
Once finished with his medical education and training, however, Dr. Idris hit his stride.
His previous 16-year tenure on the University of Florida’s faculty afforded Dr. Idris the opportunity to serve as Director of the NASA Human Space Flight Rescue Team for the Space Shuttle, where he remains a consultant. Dr. Idris was inducted into the NASA Space Technology Hall of Fame in 2008 for work he did that led to the impedance threshold device being used to treat astronauts suffering acute hypotension and autonomic dysfunction. It is now on board the International Space Station.
Recruited to UT Southwestern in 2003, he is recognized as one of the country’s leading visionaries and researchers in cardiopulmonary resuscitation. Dr. Idris’ clinical trials have changed the way chest compressions are administered, and his ongoing work with innovative programs like the Resuscitations Outcomes Consortium continues to move the needle in advancing and refining effective resuscitation techniques for people who suffer sudden cardiac arrest. In addition, he has provided expertise for numerous national organizations, including the American Heart Association, the National Institutes of Health, the Department of Defense, and NASA.
“Dr. Idris’ values remain consistent with those held by the Army, which is in part why he is viewed as one of leading researchers in the area of cardiopulmonary resuscitation,” said Dr. Deborah Diercks, Chair of Emergency Medicine and holder of the Audre and Bernard Rapoport Distinguished Chair in Clinical Care and Research.
For his part, Dr. Idris still holds to the Army leadership principle of “follow me.”
“I owe my career in medicine to the U.S. Army,” he said. “Before military service, I had little interest in biology or medicine. I think very highly of the Army, which values accountability, diligence, and integrity.”


