Extensive screening effort identifies genes behind sleep disorders

Two of life’s persistent mysteries – how the body regulates deep sleep and how it creates vivid dreams – are a step closer to being solved.
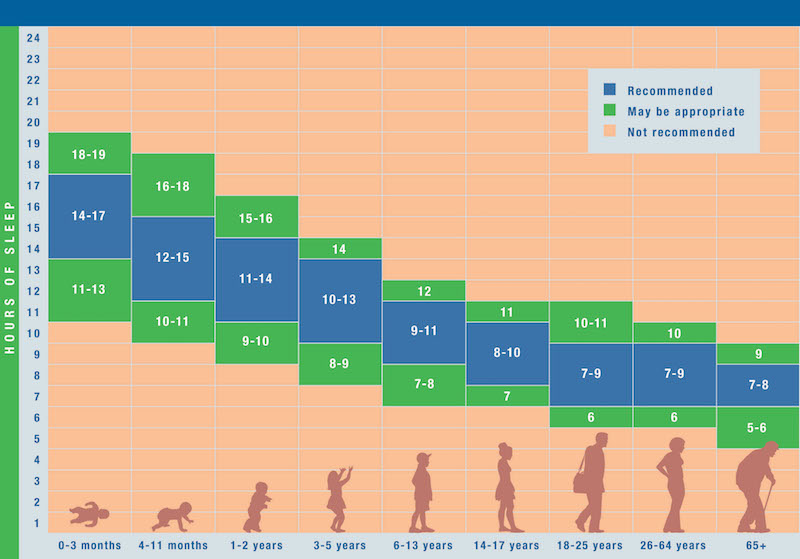
A study by Dr. Joseph Takahashi and his team at UT Southwestern’s Peter O’Donnell Jr. Brain Institute demonstrates in mice that a single gene controls the amount of non-rapid eye movement (non-REM) sleep, the stage that includes deep sleep, and that a second gene controls REM sleep, the type associated with vivid dreaming. Humans typically cycle through non-REM and REM sleep four to six times each night.
The discovery of these two genes provides an entry point to help scientists understand sleep, which in turn could lead to new treatments for the millions of people unable to get a good night’s rest.
“This research is just the beginning. We believe that these two genes are the first of many that regulate sleep,” said Dr. Takahashi, Chairman of Neuroscience within the O’Donnell Brain Institute and co-senior author of a study on the findings published in Nature.
The work required an exhaustive forward-genetic approach that screened 8,000 mice with individually applied electroencephalogy (EEG) monitors to search for brain waves indicative of sleep disorders.
The new study is closely tied to the forward genetics work Dr. Takahashi employed two decades ago in his landmark discovery of the Clock gene that regulates the body’s circadian rhythm. That finding led his laboratory to uncover a network of more than 20 other genes related to the body’s biological clock of physical and behavioral patterns that follow a roughly 24-hour cycle, mostly in response to environmental cues such as light and darkness.
Although previous research identified genes that regulate the switch between wakefulness and sleep, the mechanisms controlling the need for non-REM and REM sleep proved elusive until this latest discovery. The UT Southwestern researchers found two striking mutations: mice they called “Sleepy” that had 50 percent more non-REM sleep than wild-type mice, caused by a mutation in the Salt-Inducible Kinase 3 (Sik3) gene that showed clear dominant inheritance; and mice researchers called “Dreamless” that were severely deficient in the amount of REM sleep, a stage of rest characterized in humans by rapid eye movements and vivid dreams. This deficit was caused by a mutation in the Sodium Leak Channel Non-selective (Nalcn) gene.
When the researchers introduced the same mutations into wild-type mice, their sleep patterns mirrored those of the “Sleepy” and “Dreamless” mice, confirming each gene as the sole cause of its respective trait.
“This study opens up future possibilities to create new sleep-regulating drugs, but doing so will occur in the distant future,” said co-senior author Dr. Masashi Yanagisawa, Professor of Molecular Genetics. He now directs the International Institute for Integrative Sleep Medicine at the University of Tsukuba in Japan, where most of the mice were screened.
Many scientists agree that the REM sleep stage is involved in the formation of emotional memories and coping with negative experiences. Hence, there is a possibility that manipulation of REM sleep could aid in treatment of conditions such as post-traumatic stress disorder.
Dr. Takahashi, who holds the Loyd B. Sands Distinguished Chair in Neuroscience and received the 2016 Peter Farrell Prize in Sleep Medicine, said he had wanted to conduct such a genetic screen for sleep mutants for many years but had to overcome logistical issues. Most mouse studies involve no more than a few dozen animals and this one required thousands. Dr. Yanagisawa rapidly scaled up, optimizing his lab’s ability to screen large numbers of mice, accomplished initially at UT Southwestern and now at his institute in Japan.
“To be able to screen 8,000 mice is something that most people would say is too much work,” Dr. Takahashi said. “Technically, this project was very challenging.”