Obesity amplifies genetic risk of nonalcoholic fatty liver disease

The combination of genetics and obesity can sometimes lead to serious, life-threatening health conditions for the unsuspecting. Now, an international study based at UT Southwestern has revealed a new wrinkle in this genetic-environmental correlation: Obesity significantly amplifies the effects of three gene variants that increase the risk of nonalcoholic fatty liver disease, or NAFLD.
NAFLD is a growing problem associated with obesity. The National Institutes of Health estimates that 3 to 12 percent of adults in the U.S. have nonalcoholic steatohepatitis, the most serious form of NAFLD that can lead to chronic liver disease and liver cancer.
Of the three gene variants, or alleles, examined in the Nature Genetics study published last year, the strongest genetic-environmental interactions were found in the PNPLA3 gene variant, the first genetic cause of NAFLD ever identified. That variant was identified in the Dallas Heart Study, a longitudinal, multiethnic, population-based study directed by Dr. Helen Hobbs.
“While all obese individuals who have fatty liver disease would benefit from weight loss, our data suggest that those who have the risk allele in PNPLA3 are likely to benefit more,” said Dr. Hobbs, Director of the Eugene McDermott Center for Human Growth and Development and co-senior author of the Nature Genetics study with Dr. Jonathan Cohen, Professor of Internal Medicine.
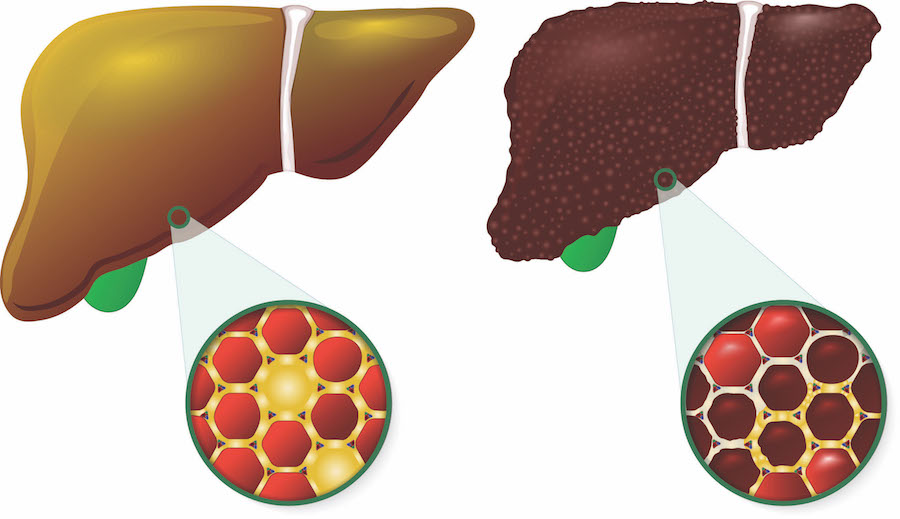
Looking first at the accumulation of fat in the liver, the researchers found that the prevalence of fat buildup ranged from 9 percent in lean individuals who did not have a PNPLA3 risk allele to 84 percent in obese individuals with two copies of the risk allele – one from each parent.
“If you are obese and have the variant – particularly if you have two copies of the variant – you are very likely to have excess fat in your liver,” said Dr. Cohen, who also has appointments in the Center for Human Nutrition and the McDermott Center and holds the C. Vincent Prothro Distinguished Chair in Human Nutrition Research.
The findings indicate that the interaction between obesity and genetics appears to promote chronic liver disease (cirrhosis) as well as the accumulation of fat in the liver.
“The risk alleles of the three strongest NAFLD risk variants confer only moderate risk in lean individuals but are major risk factors in people with higher BMIs, suggesting that genetic screening would be especially valuable in this subgroup,” Dr. Hobbs said.
Dr. Hobbs, a Howard Hughes Medical Institute Investigator and member of the National Academy of Sciences, is also Chief of Clinical Genetics, Professor of Internal Medicine and Molecular Genetics, and a faculty member in the Center for Human Nutrition. She holds the Eugene McDermott Distinguished Chair for the Study of Human Growth and Development; the Philip O’Bryan Montgomery, Jr., M.D. Distinguished Chair in Developmental Biology; and the 1995 Dallas Heart Ball Chair in Cardiology Research.