A national effort to understand acute liver failure – two decades and 3,000 study participants later

DALLAS – March 28, 2017 – A multicenter study on acute liver failure funded by the National Institutes of Health (NIH) has increased understanding of this sometimes fatal condition since the research effort began 20 years ago, improving patient care and saving lives.
The Acute Liver Failure Study Group, now active at 12 sites in the U.S. and Canada, including UT Southwestern Medical Center, recently recruited its 3,000th participant.
Information gathered from those patients over the years has given physicians a clearer picture of what acute liver failure (ALF) looks like and how best to treat it – as well as how acetaminophen poisoning became the No. 1 cause of ALF in the United States, dwarfing other causes of the condition such as hepatitis and other drug poisonings.
The study group’s principal investigator, Dr. William M. Lee, Professor of Internal Medicine at UT Southwestern and a world-renowned liver disease expert, began the research effort in 1997 after receiving the initial NIH grant. The NIH’s National Institute of Diabetes and Digestive and Kidney Diseases has funded the study ever since, with plans to continue support through 2020.
“ALF is extremely rare, with only about 2,000 cases in the U.S. each year,” said Dr. Lee, who holds the Meredith Mosle Chair in Liver Disease in his honor. “Because of its rarity, many physicians aren’t that familiar with this rapidly progressive and fatal liver disease and may not recognize it quickly.”
Diagnosing the condition immediately is important, Dr. Lee added. The only proven antidote, N-acetylcysteine (NAC), must be given within 12 hours of acetaminophen ingestion for maximum protection. Brain swelling, coma, extensive liver damage leading to the need for a transplant – or death – can be the result of waiting too long.
Thanks to the study group’s efforts, gains have been made in diagnosis and treatment. In 2014, the group released a free iPhone app to provide physicians with guidelines for diagnosing and treating ALF. In 2016, the group launched a second free app to assess prognosis, helping physicians determine if a patient is likely to die or need a liver transplant. Available at the iPhone app store, the apps are titled “Acute Liver Failure Prognostic Model” and “ALF Checklist.”
Currently, the study group is evaluating a test developed at the University of Arkansas that rapidly detects the toxic byproducts of acetaminophen poisoning to identify an overdose patient quickly. If the test proves to be effective, it could be available in two to three years, Dr. Lee said.
A new medication to treat all forms of ALF is also under study by the group. Working with the North Carolina biopharmaceutical company Ocera Therapeutics Inc., the group has tested the safety and tolerability of this potential drug to treat brain edema before symptoms progress.
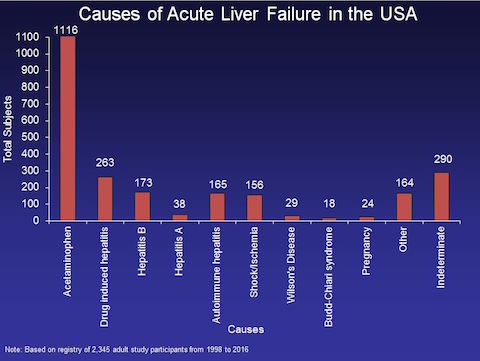
Since 1997, the Acute Liver Failure Study Group has published 94 papers on acute liver failure. These are some of its key findings:
- A 2009 study determined that the antidote NAC can effectively treat ALF caused by drugs other than acetaminophen, if given in time.
- A 2016 study showed that ALF patients whose conditions were caused by acetaminophen poisoning were more likely to die within 48 hours than those with other causes of liver failure.
- A second 2016 study found that ALF patients overall are now more likely to survive and less likely to require a liver transplant than in earlier years. The study speculated that more effective intensive care unit management may be a factor.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty includes many distinguished members, including six who have been awarded Nobel Prizes since 1985. The faculty of almost 2,800 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide medical care in about 80 specialties to more than 100,000 hospitalized patients and oversee approximately 2.2 million outpatient visits a year.
###
Media Contact: Carol Marie Cropper
214-648-3404
carol.cropper@utsouthwestern.edu
To automatically receive news releases from UT Southwestern via email, subscribe at www.utsouthwestern.edu/receivenews