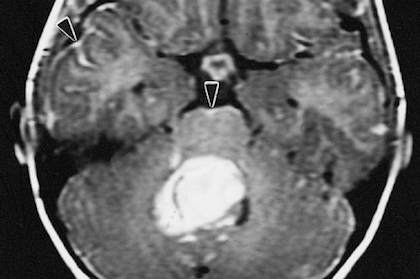
Do you really need that MRI?
Image ordering often based on factors other than patient need
DALLAS – Sept. 25, 2017 – Do you really need that MRI?
Your doctor may order an MRI based on factors other than your actual medical need for imaging, researchers in UT Southwestern’s Center for Patient-Centered Outcomes Research found. Their study in JAMA Internal Medicine showed that a physician’s prior image-ordering habits, as well as ownership of the equipment, were strong indicators of unnecessary imaging orders.
“Whether or not you get unnecessary imaging is partly explained by how much unnecessary imaging the clinician orders in general and whether or not the clinician owns the imaging equipment,” said lead author Dr. Arthur Hong, Assistant Professor of Internal Medicine and Clinical Sciences at UT Southwestern Medical Center. “For patients who got an MRI but did not need one, which doctor they went to mattered more than the injury or symptom that they had. With people more on the hook for the costs of their care, it’s increasingly important for physicians to offer financially responsible care.”
Uncomplicated back pain and uncomplicated headaches are two of the most common reasons patients with health insurance received low-value, or unnecessary, imaging such as X-rays, computed tomography (CT), or magnetic resonance imaging (MRI). Previous studies have shown that this kind of wasteful care may account for up to one-third of all medical expenditures. In addition, low-value services can trigger downstream cascades of unnecessary care and clinical harm, said Dr. Hong, a Texas Health Resources Clinical Scholar.
The JAMA Internal Medicine study examined the records and characteristics of 100,977 primary care physicians, specialist physicians, and chiropractors in search of predictors for unnecessary back pain and headache image ordering. They found:
- Chiropractors and specialists were more frequent back pain imagers.
- Primary care physicians who ordered more back pain imaging also ordered more headache imaging.
Next steps for researchers include examining other nonclinical factors that continue to influence clinician practice habits, and ultimately exploring how to help patients and clinicians make better clinical decisions together.
The study was completed in partnership with researchers from Harvard Medical School’s Department of Population Medicine at the Harvard Pilgrim Health Care Institute.
The UT Southwestern Center for Patient-Centered Outcomes Research, established in 2013, helps facilitate studies designed to ensure delivery of high-quality, patient-centered, evidence-based, equitable care. The Center was established through a grant from the Agency for Healthcare Research and Quality (AHRQ). AHRQ’s mission is to produce evidence to make health care safer, higher quality, more accessible, equitable, and affordable, and to work with the U.S. Department of Health and Human Services and other partners to ensure that the evidence is understood and used.
About UT Southwestern Medical Center
UT Southwestern, one of the premier academic medical centers in the nation, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty has received six Nobel Prizes, and includes 22 members of the National Academy of Sciences, 18 members of the National Academy of Medicine, and 14 Howard Hughes Medical Institute Investigators. The faculty of more than 2,700 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in about 80 specialties to more than 100,000 hospitalized patients, 600,000 emergency room cases, and oversee approximately 2.2 million outpatient visits a year.
###
To automatically receive news releases from UT Southwestern via email, subscribe at www.utsouthwestern.edu/receivenews.