Multiple Sclerosis and Neuroimmunology
Benjamin Greenberg, M.D.
Professor
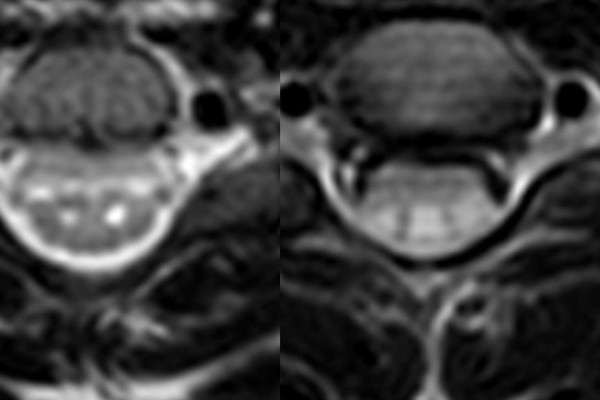
My research focuses on autoimmune conditions of the central nervous system. Our team is focused on developing new biomarkers and therapeutics by utilizing specimens collected from research participants. Serum markers, plasma markers and B cells from participants are isolated and utilized to understand the basic biology of multiple sclerosis, transverse myelitis, neuromyelitis optica and autoimmune encephalitis. This information is used to identify new therapies. Additionally, I focus on clinical trial designs and execution for these conditions.
Nancy Monson, Ph.D. Professor
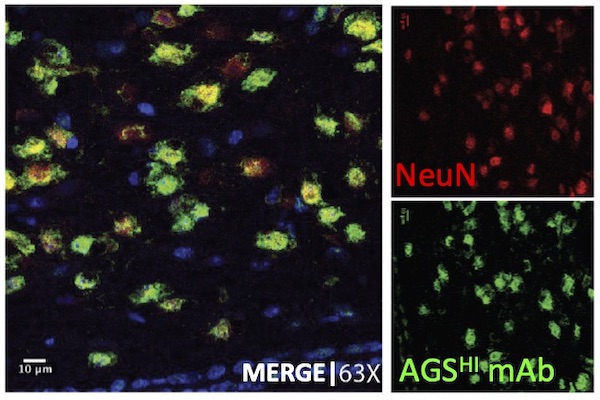
The primary focus of the Monson laboratory is to identify mechanism(s) of neuroinflammation in patient populations that will facilitate the development of therapies to prevent long-term deficits. Indeed, our work in Multiple Sclerosis has already directly contributed to novel therapies, mechanistic understanding, and biomarkers. We were also the first to demonstrate antibodies produced by B cells from MS patients bind neurons in the cortex, supporting the concept of underlying gray matter disease as a critical feature of MS pathology in addition to white matter disease. More recently, we have begun to use our ground-breaking translational neuroimmunology experience to pursue our understanding of other diseases involving the immune system including Alzheimer’s Disease, Gulf War Illness, autoimmune encephalitis, transverse myelitis, and stroke.
Shanan Munoz, M.D.
Assistant Professor
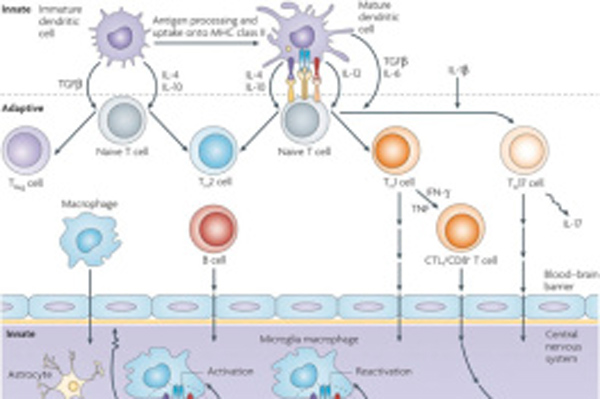
Dr. Munoz is enthusiastic about the increased understanding of the complexity of the immune system's role in causing & perpetuating MS since that has led to many new treatments with differing mechanisms of action. She has participated in trials with injectable, oral, & IV medicines for MS, helping to find effective, well tolerated options for patients.
NMO is a rare neurological disorder and until recently had no FDA approved medicine for it. Dr. Munoz is excited to be participating in studies for treatments of this devastating disease. This inflammatory disease attacks astrocytes in the central nervous system, & in most cases has antibodies to the AQP4 water channels. It can have severe relapses that could cause blindness, painful spasms, weakness, and other symptoms.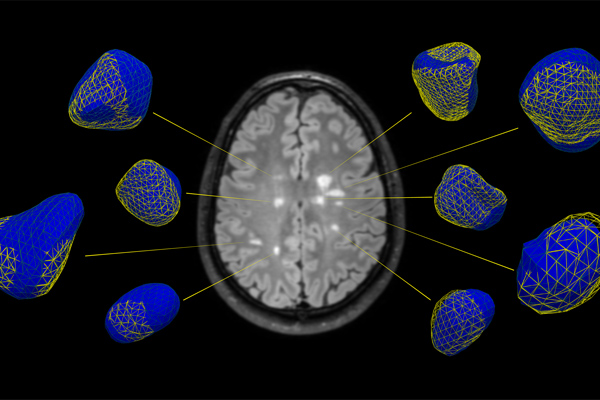
Darin Okuda, M.D.
Professor
The Okuda lab expands current in vivo imaging capabilities for patients with neurological disease through the development of software that allows for study of quantitative 3-dimensional shape, surface, and structural characteristics of brain lesions along with their impact on metabolic signatures in surrounding tissue. These efforts enhance diagnosis, disease surveillance, the study of treatment effects, and the assessment of investigational reparative therapies. Our group is also involved in medical device fabrication and creating prescription digital therapeutics.

Peter Sguigna, M.D.
Assistant Professor
Our lab studies the visual system in multiple sclerosis and other neuro-ophthalmological diseases. We use non-invasive testing to better understand how light integrates into the brain, including the ability for it to synchronize circadian rhythms.
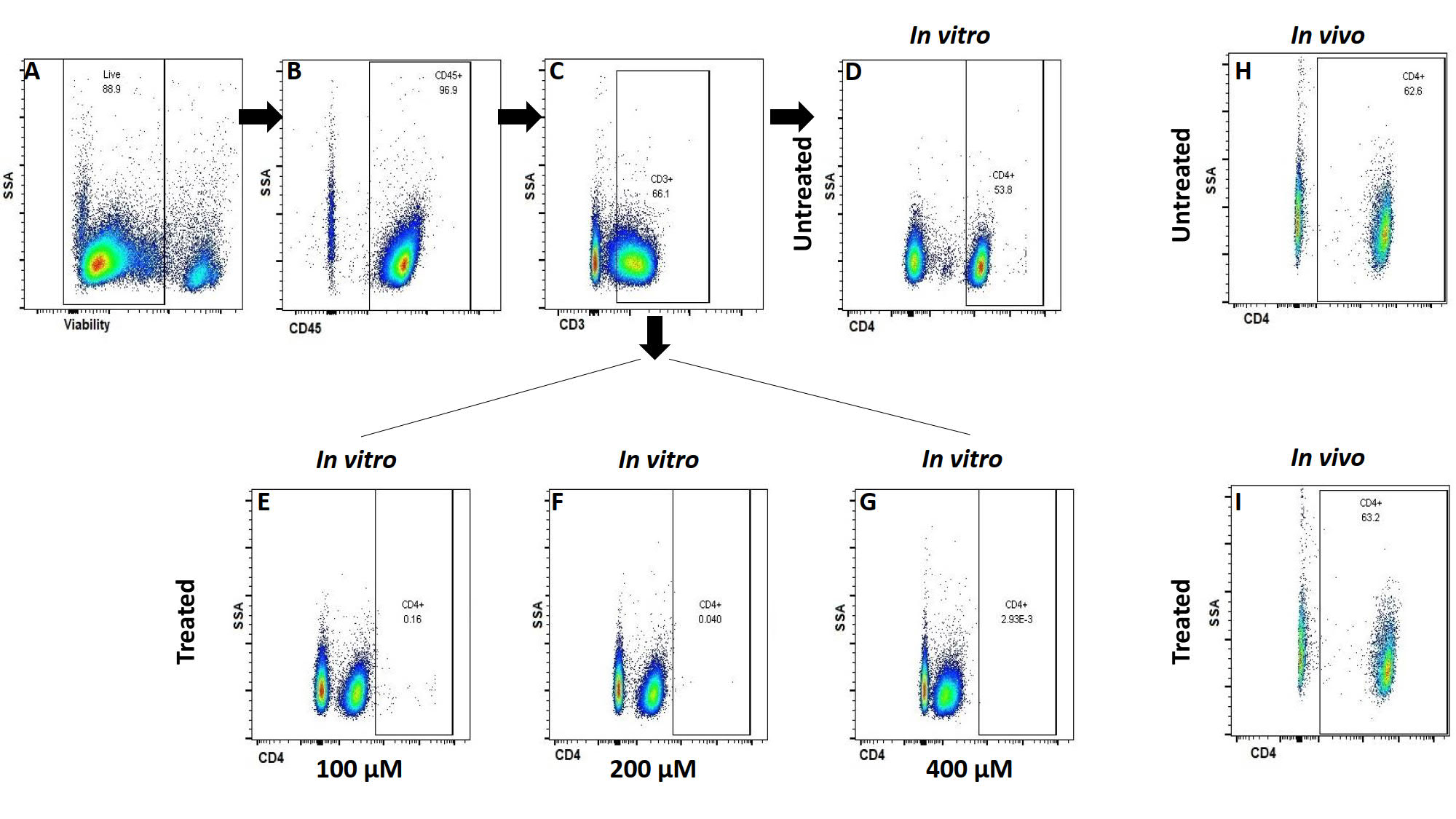
Olaf Stuve, M.D., Ph.D.
Professor
Since joining the department of Neurology, the research in my laboratory has focused on cellular and molecular events that result in the breakdown of immune tolerance in patients with inflammatory disorders of the central nervous system (CNS). One major focus has been to study the effect of pharmacotherapies on adaptive immune responses in the human inflammatory disease multiple sclerosis (MS), and its model experimental autoimmune encephalomyelitis (EAE). We also aim to characterize leukocytes that initiate and perpetuate CNS inflammation in other models of human inflammatory neurological disorders. There is an ongoing effort to translate observations made in the laboratory to the bedside, and clinical trials in MS, amyotrophic lateral sclerosis, and Alzheimer disease (AD) have served that goal.
